Dermatology Eponyms – sign –Lexicon (W)
Piotr Brzeziński 1, Lorenzo Martini1, Khalifa E. Sharquie2, Yorulmaz Ahu3, Khalid Al Aboud4, Rana Rafiei5, Rita Vipul Vora6, Andrzej Grzybowski7,8
1, Lorenzo Martini1, Khalifa E. Sharquie2, Yorulmaz Ahu3, Khalid Al Aboud4, Rana Rafiei5, Rita Vipul Vora6, Andrzej Grzybowski7,8
1Department of Physiotherapy and Medical Emergency, Faculty of Health Sciences, Pomeranian Academy, Slupsk, Poland; 2Department of Dermatology, College of Medicine, University of Baghdad, Iraqi and Arab Board for Dermatology and Venereology, Center of Dermatology and Venereology, Medical City, Baghdad, Iraq; 3Ankara Numune Research and Education Hospital, Department of Dermatology, Ankara, Turkey; 4Department of Dermatology, King Faisal Hospital in Makkah, Makkah, Saudi Arabia; 5Skin Research Center, Department of Dermatology, Razi Hospital, School of Medicine, Guilan University of Medical Sciences, Rasht, Iran; 6Department of Skin and VD, Shree Krishna Hospital, Karamsad, Anand, Gujarat, India; 7Chair of Ophthalmology, University of Warmia and Mazury, Olsztyn, Poland; 8Head of the Institute for Research in Ophthalmology, Poznan, Poland
Corresponding author: Dr. Piotr Brzeziński, E-mail: brzezoo77@yahoo.com
Submission: 08.07.2019; Acceptance: 26.10.2019
DOI:10.7241/ourd.20201.34
Cite this article: Brzeziński P, Martini L, Sharquie KE, Ahu Y, Al Aboud K, Rafiei R, Vora RV, Grzybowski A. Dermatology Eponyms – sign –Lexicon (W). Our Dermatol Online. 2019;11(1):103-112.
Citation tools:
BibTex | CSV | RIS | Endnote XML
Copyright information
© Our Dermatology Online 2019. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Eponyms are used almost daily in the clinical practice of dermatology. And yet, information about the person behind the eponyms is difficult to find. Indeed, who is? What is this person’s nationality? Is this person alive or dead? How can one find the paper in which this person first described the disease? Eponyms are used to describe not only disease, but also clinical signs, surgical procedures, staining techniques, pharmacological formulations, and even pieces of equipment. In this article we present the symptoms starting with (W) and other. The symptoms and their synonyms, and those who have described this symptom or phenomenon.
Key words: Eponyms. Skin diseases. Sign. Phenomenon
WALCHEREN SIGN
Malarial fever in Holland [1].
WARTENBERG’S SIGN
In ulnar nerve paralysis due to leprosy, the little finger assumes the position of constant abduction secondary to paralysis of adductor digiti minimi and is considered the earliest sign of ulnar nerve affection [2].
WAX DOLI SIGN
Bagginess of the eyelids and bloated faces that give the patient an appearance of a wax doli. A sign of myxoedema. Also known as Marshalls sign [3–5].
GEOFFREY MARSHALL
British physician.
WEGENER’S SIGN
Invasive granulomatous lesion destroying the bridge of the nose and affecting the sinuses. Granulomatosis with polyangiitis is characterized by the main violation of the upper and lower respiratory tract and kidney AND Is considered a systemic vasculitis of medium-sized and small blood vessels [6,7].
FRIEDRICH RUDOLF GEORG WEGENER
German pathologist, 1907-1990 (Fig. 1). Friedrich Wegener worked in Breslau (Poland) when he first described the condition that carries his name.
 |
Figure 1: Friedrich Rudolf Georg Wegener. |
After World War II Friedrich Wegener was suspected of being a war criminal. He was interned by the Allies but was later cleared of the charges and “denazified”. As early as in 1932, eight months before Hitler came to power, he joined the S.A (Sturmabteilung) and became a member of the Nazi party on May 1, 1933. According to documents found by Alexander Woywodt in the Bundesarchiv, Wegener in 1938 became SA Sanitäts-Obersturmbannführer [8,9].
After the outbreak of the war, Wegener worked as a military pathologist in Lodz (Poland), where he also held a position in the Gesundheitsamt.
WEGNER’S SIGN
Growth arrest lines found in the upper extremities in an infant with congenital syphilis. Growth arrest lines show an enhanced zone of provisional calcification (radiopaque band) which is associated with osteoporosis immediately below the dense zone. The growth arrest line may be smooth or serrated [10]. A serrated appearance is known as Wegner’s sign.
WEIL’S SIGN
Severe leptospirosis (Figs. 2a and 2b); also called Landouzy’s sign and Fiedler’s sign. Leptospirosis is an infectious disease caused by the pathogenic spirochete Leptospira interrogans. There is a large range of clinical manifestations in leptospirosis, and infected people can present with asymptomatic illness, self-limited systemic infection or severe and potentially fatal disease [11–14]. The severe form is characterized by jaundice, acute kidney injury (AKI) and hemorrhage, and is mainly caused by the serovars Icterohaemorrhagiae, Copenhageni and Lai. There are also severe forms of the disease that occur without jaundice or renal failure, such as hemorrhagic pneumonitis.
 |
Figure 2: Weil’s sign. |
ADOIF WEIL
German physician, 1848-1916 (Fig. 3). Adolf Weil studied at Heidelberg, receiving his doctorate in 1871, and completed his education in Berlin under Ludwig Traube and Friedrich Theodor von Frerichs, and at Vienna under Ferdinand von Hebra, Moriz Kaposi and Leopold von Schrötter-Kristelli. From 1872 to 1876 he was Frerichs’ assistant, and was habilitated for internal medicine, becoming ausserordentlicher professor in 1876. In 1886 he was called to Dorpat as ordentlicher professor of clinical medicine. Already in 1887 he had to resign from his teaching duties because of tuberculosis of the larynx, also abandoning his scientific activities. For some years he practiced in the winter in Ospedaletti and San Remo, in the summer in Badenweiler, and in 1893 settled Wiesbaden, where he died in 1916.
 |
Figure 3: AdoIf Weil. |
He was professor of medicine at Tartu, Estonia, and Berlin. He described four cases of the disease which he had observed in Heidelberg [15].
WEIR-MITCHELL’S SIGN
The term erythromelalgia (Fig. 4), specific to the myeloproliferative disorders, refers to the occlusion of the microcirculation by platelets and is characterized by redness, congestion, and painful burning sensations of the extremities. Symptoms are characteristically relieved by cold or elevation of the extremity [3,16–18].
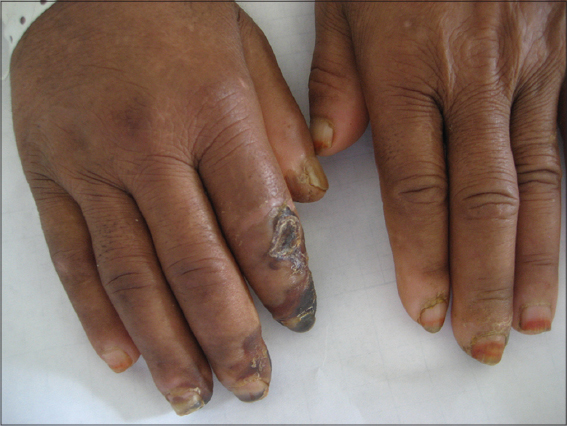 |
Figure 4: Weir-Mitchell’s sign. |
SILAS WEIR MITCHELL
American neurologist and writer known for his discovery of causalgia, 1829-1914 (Fig. 5). He studied at the University of Pennsylvania in that city, and received the degree of M.D. at Jefferson Medical College in 1850. During the Civil War he had charge of nervous injuries and maladies at Turners Lane Hospital, Philadelphia, and at the close of the war became a specialist in neurology. In this field Mitchell’s name became prominently associated with his introduction of the rest cure, subsequently taken up by the medical world, for nervous diseases, particularly neurasthenia and hysteria. His medical texts include Injuries of Nerves and Their Consequences (1872) and Fat and Blood (1877). Mitchell’s disease (erythromelalgia) is named after him. He also coined the term phantom limb during his study of an amputee. Silas Weir Mitchell discovered and treated causalgia (today known as CRPS/RSD), a condition most often encountered by hand surgeons. He is considered the father of neurology as well as an early pioneer in scientific medicine. He was also a psychiatrist, toxicologist, author, poet, and a celebrity in America and Europe. His many skills and interests led his contemporaries to consider him a genius on par with Benjamin Franklin. His contributions to medicine and particularly hand surgery continue to resonate today [3].
 |
Figure 5: Silas Weir Mitchell. |
WEREWOLF SIGN
Individuals are completely covered in hair except for their palms and soles. A sign of congenital hypertrichosis lanuginose [19,20].
WERLHOF’S SIGN
Purpura haemorrhagica [3,21,22]. Also known as Werlhoff’s sign.
PAUL GOTTLIEB WERLHOF
German physician, 1699-1767 (Fig. 6). He studied medicine at the University of Helmstedt under Lorenz Heister and Brandanus Meibom, who was the son of Heinrich Meibom. After completing his studies, he practiced medicine in Peine for four years, and in 1725 moved to Hannover, where he became one of the more influential physicians in Europe. In 1740 was appointed Königlicher Leibarzt, physician to Hannover royalty. In 1735, Werlhof presented the first description of idiopathic thrombocytopenic purpura (ITP), a bleeding disorder. In addition to his reputation as a physician, Werlhof was highly regarded as a poet, and was a good friend of anatomist Albrecht von Haller, who was also an accomplished poet. Werlhof composed his poems and hymns in German, while his medical treatises were written in Latin. Among his written works were a 1732 treatise on fevers called Observationes de febribus, and a collection of poetry titled Gedichte [23].
 |
Figure 6: Paul Gottlieb Werlhof. |
WESSELSBRON SIGN
Muscle pain, fever, super sensitive skin with possible maculopapular rash. Caused by the mosquito-borne zoonotic Wesselsbron fever flavivirus [24].
WEST NILE SIGN
Fever and rash, with respiratory and flaccid paresis caused by brain swelling. Caused by the zoonotic West Nile fever flavivirus. Can be mosquito or food borne, and has also been associated with transplants of fluids and tissues [25].
WESTBERG’S SIGN
White spot disease, morphea alba (Fig. 7) [26,27].
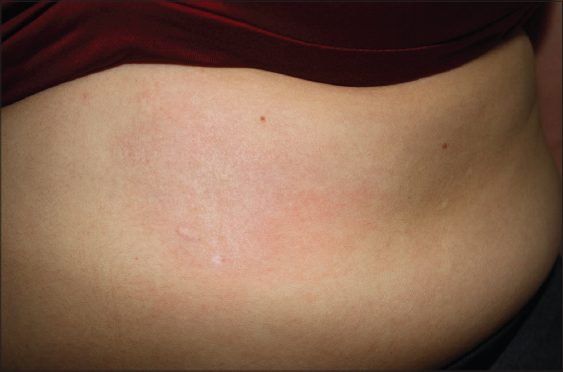 |
Figure 7: Westberg’s sign. |
FREDRICH WESTBERG
19th century German physician.
WET LEAVES SIGN
The odor of Mycobacterium tuberculosis [28–30].
MIKHAIL AFANASICVICH BULGAKOV
Russian physician, 1891-1940 (Fig. 8). Writer whose doctor stories are based on his experience as a rural physician in a small village called Nikolskoye in the province of Smolensk. Nikolskoye was his first assignment after studying medicine at Kiev University. After 18 months in Nikolskoye, he went on to specialize in venereology in Kiev. Shortly thereafter, he gave up a career in medicine for writing. All his life he was sceptical to the Soviet system and used his satire against the regime. He worked on his main work, The Master and Margarita, from 1928 until his death. The novel was not published in his lifetime [31].
 |
Figure 8: Mikhail Afanasicvich Bulgakov. |
WHALE’S FLIPPER SIGN
Obliteration of the concavity of the palm which makes the large hand look like a whale’s flipper. A sign of middle palmar space infections [32].
WHITE HAIRY TONGUE SIGN
The tongue and oral mucous membranes are covered in a white fur or plaque. An indication of an oropharyngeal infection with Candida albicans [5,33].
WHITE LEPROSY SIGN
Leukoderma, a pathologic process with the result of a deficiency in the normal pigmentation of the skin (Fig. 9). Also know by many colloquial appellations in the Indian subcontinent as sufaid-korh, cham ba, phoolyree, buras, cabbore, kuf tam, and leopard pattern [34,35].
 |
Figure 9: White Leprosy sign. |
WHITE’S SKIN SIGN
Keratosis follicularis (Fig. 10). Also known as Darier disease, Darier–White disease, Dyskeratosis follicularis [36–38].
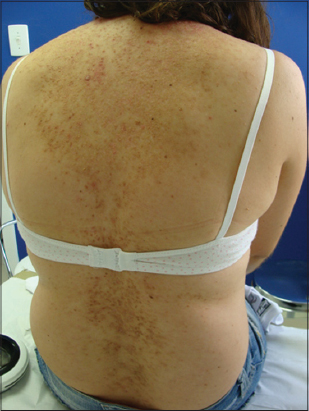 |
Figure 10: White’s skin sign. |
JAMES CLARKE WHITE
American dermatologist, 1833-1916 (Fig. 11). At the age of 16 he entered Harvard and in 1853 began his medical education at Tremont Medical School which had a semi-official connection with Harvard. He served a term as house pupil at the Massachusetts General Hospital, and received his M.D. in 1855. A European postgraduate tour, during which he worked under Oppolzer, Sigmund, and Hebra, was completed in 1857. After an early interest in toxicology and chemistry, White turned to dermatology exclusively, and in 1863 became Professor of Dermatology at Harvard. He was the first President of the American Dermatological Association, and the first to describe keratosis follicularis, also known as “Darier-White Disease” [36].
 |
Figure 11: James Clarke White. |
WHITE-SPOT SIGN
Degeneration of the papillary and reticular layers of the skin marked by the formation of white bead-like spots; morphea guttata. Also know as Westberg’s sign.
WICKHAM SIGN
Also know as Wickham’s striae (Fig. 12). There are delicate white or grey lines that course the surface of a papule of lichen planus [39]. The lines may be seen only at the periphery of a papule, but usually they form a network across the entire papule. They are most pronounced in fully developed lesions that tend to be aggregated.
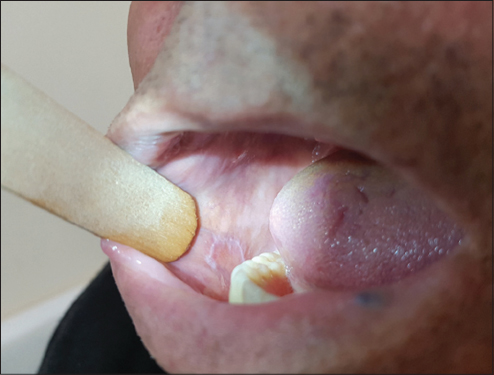 |
Figure 12: Wickham sign. |
LOUIS FRÉDÉRIC WICKHAM
French physician and pathologist (1861-1913), (Fig. 13). In 1895, Louis-Fédéric Wickham described whitish streaks, now known as Wickham’s striae, on the surface of lichen planus papules [40]. He received his education at Paris and obtained his doctorate in 1890. He then turned to the study of dermatology, worked several years at the Hôpital Saint-Louis, and in 1897 became Médecin at the Hôpital Saint Lazare. From 1905 he concerned himself with radium research, and occasioned the establishment of the Laboratoire Biologique du Radium. His work concerns the treatment of angiomas, celoids, carcinomas of the skin, and other dermatoses, and on the effect of radium on visceral carcinoses. In 1888 he was commissioned to report on the methods of teaching dermatology in England. He designed a multibladed knife for scarification treatment of lupus vulgaris.
 |
Figure 13: Louis Frédéric Wickham. |
WIDY SIGN
Hairs that showed a deposit of melanin pigment at its distal end [41].
WILLAN’S SIGN
Psoriasis circinate [42,43]. Also called Willan’s lepra. When in psoriasis the eruption involves only a limited extent of space, the epidermic scales may become loosened and fall off, leaving bright-red, slight elevated spots or we notice only a partial desquamation especially in the middle of single circular patches, giving rise to psoriasis orbicularis (lepra Willani or psoriasis laepreformis) [44].
ROBERT WILLAN
English physician, 1757-1812 (Figs. 14 and 15). A 1780 graduate in medicine from the University of Edinburgh, spent most of his professional life in London. He worked at the Carey Street Public Dispensary, which was also staffed mainly by such graduates from Edinburgh as Thomas Bateman, Richard Bright, and Thomas Addison. Willan’s major dermatology works can be categorized into two groups: an introduction of the first classification of skin diseases, and the correct clinical descriptions of many diseases. Both were based predominantly on morphologic features rather than on the etiologic or pathophysiologic characteristics of a disease. Between 1798 and 1808, Willan published a four-part work, Cutaneous Diseases, in which he developed a classification of skin diseases according to the form of their pathologic products. Willan was also the first to recognize the importance of illustrations in the description of skin disorders and to create the first atlas of skin diseases containing color pictures [45]. Willan divided all cutaneous disorders into nine orders: papulae, squamae, exanthemata, bullae, pustulae, vesiculae, tubercula, maculae, and dermal excrescences. For the first time in history, a physician with access to patients with abundant cutaneous problems scrutinized individual spots with the intention of recording every shade and detail. Willan was the first to give a comprehensive medical account of psoriasis, erythema nodosum, a skin symptom of sarcoidosis,12 herpes simplex and herpes zoster lesions of the skin,13 and Schönlein-Henoch purpura, ichthyosis hystrix,14 and ichthyosis.
 |
Figure 14: Robert Willan. |
 |
Figure 15: Robert Willan grave. |
Grounded on Willan’s famous principals of skin disease, dermatology was recognized as its own specialty within the field of medicine in 1884 [46].
WILLAN’S CHEEK SIGN
Lupus vulgaris of the cheek (Figs. 16a and 16b). Lupus vulgaris is the oldest forms of cutaneous tuberculosis described in the medical literature and were known as the king’s evil. The word ‘Lupus’, meaning wolf, was given to the lesion because of the ulcerating and devouring character of the lesion. Lupus vulgaris is a form of reinfection tuberculosis of the skin occurring in patients with moderate to high degree of immunity, originating from an underlying tuberculosis focus of the skin. However, it may also result through exogenous inoculation. Lupus vulgaris at the site of BCG vaccination has also been reported [47].
 |
Figure 16: (a, b) Willan’s cheek sign. |
WILLARD’S SIGN
Lupus vulgaris (Figs. 17a and 17b). Lupus vulgaris is the most common type of cutaneous TB often presents as an asymptomatic, slow growing plaque on the face. Approximately 1%-2% of all cases of tuberculosis are cutaneous tuberculosis [48,49].
 |
Figure 17: (a, b) Willard’s sign. |
WILSON’S SIGN
Dermatitis exfoliative [50].
SIR WILLIAM JAMES ERASMUS WILSON
English dermatologist and philanthropist 1809-1884 (Fig. 18). First described lichen planus in 1869 and attributed its cause to stress. He practiced in London, and published a “System of Human Anatomy,” (1842), which has passed through many editions, “Disease of the Skin” and other works relating to dermatology; “Cleopatra’s Needle” and “The Egypt of the Past,”. Known as Sir Erasmus, he was of the greatest dermatologists of his time. He is so well known as a dermatologist, occupying the first rank in England, that any contributions from his pen must command attention. He was also known for his philanthropy. Erasmus Wilson was knighted in 1881 [51].
 |
Figure 18: Sir William James Erasmus Wilson. |
WIMBERGER’S SIGN
Erosion of the upper end of the tibia in carly syphilis (Fig. 19).
Wimberger’s sign is the presence of bilateral, symmetrical, and well-defined metaphyseal defects on the medial surface of upper tibia, can result in pseudoparalysis, and is considered pathognomonic of congenital syphilis [52,53].
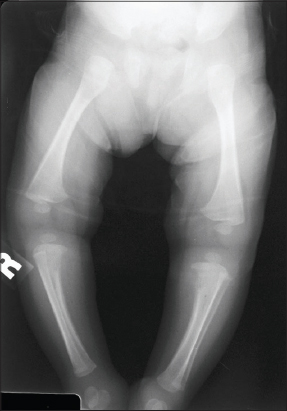 |
Figure 19: Wimberger’s sign. |
WINE SWEAT SIGN
Perspiration with the taste of wine [54].
CASPAR BARTHOLIN THE YOUNGER (SECUNDUS)
Danish anatomist and physician, born September 10, 1655, Copenhagen; died June 11, 1738 (Fig. 20). Caspar Bartholin began his medical studies in 1671, and already in 1674, aged 19, he was appointed professor of philosophy by the King, Christian IV. In 1678 he was conferred doctor of medicine by his father, Thomas Bartholin [31].
 |
Figure 20: Caspar Bartholin the Younger (Secundus). |
WINTERBOTTOM’S SIGN
Enlargement of posterior cervical lymph nodes in African trypanosomiasis [55,56]. It is seen in early stages of African trypanosomiasis caused by Trypanosoma brucei rhodensiense and Trypanosoma brucei gambiense known Sleeping sickness. Winterbottom’s sign is enlargement of lymph nodes in the posterior cervical chain.
THOMAS MASTERMAN WINTERBOTTOM
English physician, philanthropist and abolitionist 1765-1859 (Fig. 21). He studied medicine at the University of Edinburgh and then the University of Glasgow. He was appointed physician to the colony of the Sierra Leone Company in 1792. Wilson went on to become one of the first European trained African medical staff in Africa.
 |
Figure 21: Thomas Masterman Winterbottom. |
Winterbottom noted that slave traders used the sign of neck swelling as an indicator of sleepiness, and would avoid those slaves. He had no children, so his considerable estate was left to a number of charities which he had supported during his life. The bulk of this bequest was to found the South Shields Marine College, which he had established in 1837 [57].
WOOL-SORTERS’ SIGN
A form of anthrax attacking those who handle wool [58].
WRIST SIGN
Loss of pulse at the wrist, an indication of cholera [59].
WRIST SIGN (WALKER–MURDOCH SIGN)
The distal phalange of the first and fifth fingers of the hand overlaps when wrapped around the opposite wrist seen in patients having Marfan syndrome (Fig. 22) [60].
 |
Figure 22: Wrist sign (Walker–Murdoch sign). |
REFERENCES
1. Lynch J. The lessons of Walcheren Fever, 1809. Mil Med. 2009;174:315-9.
2. Kilgus M, Burg D, Loss M, Weishaupt D, Meyer VE. [Wartenberg’s Sign of Ulnar Nerve Lesion. A Contribution to Pathophysiology and to the Differential Diagnosis]. Handchir Mikrochir Plast Chir. 2003;35:251-8.
3. Brzezinski P, Bourée P, Chiriac A, Bouquot JE, Schepis C, Hofer T, et al. Dermatology Eponyms ? Sign ? Lexicon ? (M). Our Dermatol Online. 2014;4:312-26.
4. Brzezinski P, Fiorentino DF, ArunachalamP, Katafigiotis I, Matuszewski Ł, Narita M, et al. Dermatology Eponyms –Sign –Lexicon –(K). Our Dermatol Online. 2014;5:95-102.
5. Brzezinski P, Sinjab AT, Masferrer E, Gopie P, Naraysingh V, Yamamoto T, et al. Dermatology Eponyms –sign –Lexicon (G). Our Dermatol Online. 2012;3:243-57.
6. Abreu Velez AM, Brown VB, Shipp L, Smoller BR, Howard MS. N-traps and C-ancas in a lupus erythematosus-scleroderma overlap syndrome with vasculitis and panniculitis. Our Dermatol Online. 2013;4:83-6.
7. Abreu Velez AM, Brown VM, Howard MS. Immunoreactivity to dermal vessels in a patient with pyoderma gandrenosum. Our Dermatol Online. 2014;5:419-22.
8. Sowida M. Granulomatosis polyangiitis. BMJ Case Rep. 20198;12:pii:e22?.
9. Grzybowski A, Rohrbach JM. Eponyms:what’s in a name. Retina. 2011;31:1439-42.
10. Jacoby MG. The birth of Kaiser William II (1859–1941) and his birth injury. J Med Biogr, 2008;16:178-83.
11. Brzezinski P, Chiriac A, Arenas R, Dori GU, Monteiro R, Cairncross S, et al. Dermatology Eponyms –Sign –Lexicon –(L). Our Dermatol Online. 2014;5:217-30.
12. Brzezinski P, Godoy Gijón E, López-López J, Toyokawa T, Scrimshaw NS, Malard O, et al. Dermatology eponyms ? phenomen/sign ? Lexicon (F). Our Dermatol Online. 2012;3:66-78.
13. Wollina U, Hansel G, Schönlebe J. Cowpox virus infection from ped rat. Our Dermatol Online. 2018;9:31-4.
14. Martinez Braga G, Di Martino Ortiz B. Septal panniculitis:Clinico-pathological review of the literature and case presentation. Our Dermatol Online. 2014;5:74-82.
15. Alston JM, Brown HC. The epidemiology of Weil’s disease:(Section of Epidemiology and State Medicine). Proc R Soc Med. 1937;30:741-56.
16. Chaouche M, Zinoune S, Cherif AD, Barbach Y, Elloudi S, Baybay H, et al. Primary erythromelalgia –case report. Our Dermatol Online. 2019;10(e):e14.1-e14.2.
17. Lunge S, Mahajan P, Gokhale N, Pinto R. Unusal presentation of granuloma annulare restricted over the palms:a rare case presentation. Our Dermatol Online. 2014;5:45-7.
18. Ajili F, Mansour HB, Ghedira H, Zriba S, Metoui L, Gharsallah I, et al. Digital ischemia due to systemic sclerosis associated to essential thrombocythemia:A case report. Our Dermatol Online. 2013;4:508-10.
19. Al Aboud D. Hairy ears;Revisited. Our Dermatol Online. 2014;5:215-6.
20. Shah IH, Zeerak S, Sajad P, Bashir S, Bhat YJ, Mubashir S. Congenital hypertrichosis lanuginosa. Indian J Dermatol Venereol Leprol. 2018;84:248.
21. Wells LE, Kennon A. Purpura Fulminans in an adult with Pseudomonas aeruginosa septicemia. Our Dermatol Online. 2018;9:404-6.
22. Hiraiwa T, Hanami Y, Yamamoto T. Six cases of purpuric eruptions induced by epidermal growth factor receptor inhibitors. Our Dermatol Online. 2018;9:89-90.
23. Hoffmann KF. [In memory of Paul Gottlieb Werlhof]. Med Monatsschr. 1950;4:624.
24. Diagne MM, Faye M, Faye O, Sow A, Balique F, Sembène M, et al. Emergence of Wesselsbron virus among black rat and humans in Eastern Senegal in 2013. One Health. 2017;3:23-8.
25. Guarner J, Hale GL. Four human diseases with significant public health impact caused by mosquito-borne flaviviruses:West Nile, Zika, dengue and yellow fever. Semin Diagn Pathol. 2019;36:170-6.
26. Arif T, Hassan I, Nisa N. Morphea and vitiligo-A very uncommon association. Our Dermatol Online. 2015;6:232-4.
27. Nassiri A, Aqil N, Baybay H, Mernissi FZ. Porcelain plaques:what is your diagnosis. Our Dermatol Online. 2019;10(e):e4.1-e4.3.
28. Eftekhari H, Rana R, Arash D, Maryam MH, Sara NR. Lupus vulgaris of the auricle. Our Dermatol Online. 2017;8:31-3.
29. Salissou L, Adehossi E, Maman Laouali S, Mamadou S, Nouhou H. Cutaneous tuberculosis in Niger:a 9-year retrospective study. Our Dermatol Online. 2015;6:153-6.
30. Desai CA. Granulomatous reaction following mantoux test:A rare complication. Our Dermatol Online. 2017;8:507-8.
31. Grzybowski A, Dobrowolska B, Kwiatkowska J, Sak J. Mikhail Bulgakov:The man torn between medicine and literature. Clin Dermatol. 2017;35:410-5.
32. Gray FJ. Infections of the hand. P N G Med J. 1975;18:113-8.
33. El Anzi O, Maouni S, Meknassi I, Hassam B. Pigmented fungiform papillae of the tongue:Moroccan case. Our Dermatol Online. 2019;10:215-6.
34. Sharquie KE, Noaimi AA. Follicular vitiligo:the present clinical status. Our Dermatol Online. 2016;7:176-8.
35. Deepadarshan K, Gangadhar B, Mallikarjun M. Cutaneous hypopigmentary disorders – An observational study. Our Dermatol Online. 2016;7:145-8.
36. Al Aboud A, Al Aboud K. A mini-review on eponyms in the dermatology literature linked to France. Our Dermatol Online. 2013;4(Suppl. 2):440-3.
37. Brzezinski P, Martini L. Usage of unsaturated esters of retinol to defeat Hopf’s acrokeratosis verruciformis in hands and feet of a young man. Our Dermatol Online. 2018;9:339-40.
38. Brzezinski P, Wollina U, Poklękowska K, Khamesipour A, Herrero Gonzalez JE, Bimbi C, et al. Dermatology eponyms –phenomen/sign –Lexicon (D). N Dermatol Online. 2011;2:158-70.
39. Yorulmaz A, Bulut PD, Yalcin B. Nail lichen planus:a patient with atypical presentation. Our Dermatol Online. 2018;9:434-6.
40. Al Aboud K, Al Aboud A. Eponyms in the dermatology literature linked to the oral disorders. Our Dermatol Online. 2013;4:247-50.
41. Bárzaga HOV, Padrón GV, Cabrera AR, Rodríguez KMS. Alopecia areata multifocal associated to oral sepsis. A case report. Rev Arch Méd Camagüey. 2007;11:1-3.
42. De Bersaques J. Two pre-Willan descriptions of psoriasis. Clin Dermatol. 2012;30:544-7.
43. Brzezinski P, Sinjab AT. Pityriasis rosea in 12-months-old infant. Our Dermatol Online. 2012;3:119-22.
44. Brzeziński P, Martini L. A biological foray to stop the evolution from the simplest psoriasis punctata to other more serious skin disorders by the aids of natural antihistamine and antibiotics. Our Dermatol Online. 2019;10(e):e17.1-e17.4.
45. Grzybowski A, Parish LC. Robert Willan:pioneer in morphology. Clin Dermatol. 2011;29:125-9.
46. Swank A, Grzybowski A, Parish LC. Robert Willan:a Quaker physician who founded the morphologic approach to modern dermatology. Clin Dermatol. 2011;29:571-3.
47. Vora RV, Diwan NG, Jivani NB, Singhal RR. Lupus vulgaris involving both inguinal regions:a case of autoinoculation. J Clin Diagn Res. 2016;10:WJ01-2.
48. Eftekhari H, Rana R, Arash D, Maryam MH, Sara NR. Lupus vulgaris of the auricle. Our Dermatol Online. 2017;8:31-3.
49. Boulle S, Civatte J, Boulle M. [Extensive Willard type lupus following BCG vaccination]. Bull Soc Fr Dermatol Syphiligr. 1958;65:274-9.
50. Mohamed Saleem TS, Jyothi K, Babu SC. Report:A case report on Nevirapine induced exfoliative dermatitis. Pak J Pharm Sci. 2019;32:221-2.
51. Hadley RM. The life and works of Sir William James Erasmus Wilson;1809-84. Med Hist. 1959;3:215-47.
52. Goraya JS, Trehan A, Marwaha RK.Indian Pediatr. 1997;34:1133-4.
53. Krishnan A, Samayam A, Patra AK. Syphilis:case series. Our Dermatol Online. 2019;10:286-8.
54. Petrozziello M, Asproudi A, Guaita M, Borsa D, Motta S, Panero L, et al. Influence of the matrix composition on the volatility and sensory perception of 4-ethylphenol and 4-ethylguaiacol in model wine solutions. Food Chem. 2014;149:197-202.
55. Bourée P. Romana’s sign. Our Dermatol Online. 2015;6:248.
55. Xiao Z, Dong A, Wang Y. FDG PET/CT in a Case of Human African Trypanosomiasis (Sleeping Sickness). Clin Nucl Med. 2018;43:619-22.
56. Al Aboud K, Al Aboud A. Eponyms linked to „signs”in the dermatology literature. Our Dermatol Online. 2013;4:579-81.
57. Kissling E, Wattiau P, China B, Poncin M, Fretin D, Pirenne Y, et al. B. anthracis in a wool-processing factory:seroprevalence and occupational risk. Epidemiol Infect. 2012;140:879-86.
58. Morof D, Cookson ST, Laver S, Chirundu D, Desai S, Mathenge P, et al. Community mortality from cholera:urban and rural districts in Zimbabwe. Am J Trop Med Hyg. 2013;88:645-50.
59. Cocco G. Images in cardiology:The “thumb and wrist sign“in Marfan syndrome. Heart. 2001;86:602.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0001-6817-606X http://orcid.org/0000-0001-6817-606X http://orcid.org/0000-0003-4687-0522 http://orcid.org/0000-0003-4687-0522 http://orcid.org/0000-0001-6599-0058 http://orcid.org/0000-0001-6599-0058 |


Comments are closed.