Granulocyte-Colony stimulating factor induced early psoriasis – a case report and literature review
Manandhar Upasana, Wang Yue Yin, Wu Jian Bo, Song Ji Quan
Department of Dermatology and Venereology at Zhongnan Hospital of Wuhan University, Wuhan City, Hubei Province, China
Corresponding author: Prof. Song Ji Quan, E-mail: songjiq@126.com
Submission: 05.07.2019; Acceptance: 26.09.2019
DOI: 10.7241/ourd.20201.14
Cite this article: Upasana M, Yin WY, Bo WJ, Quan SJ. Granulocyte-Colony stimulating factor induced early psoriasis – a case report and literature review. Our Dermatol Online. 2020;11(1):56-58.
Citation tools:
BibTex | CSV | RIS | Endnote XML
Copyright information
© Our Dermatology Online 2019. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Human Recombinant Granulocyte colony-stimulating(G-CSF) factor is a hematopoietic growth factor; most commonly known to be used for chemotherapy induced neutropenia. A case of 43 years old lady, post radical mastectomy for breast cancer and one cycle of chemotherapy was encountered with the development of massive eruptions all over the body including the scalp with adherent silvery scales after 10 days of administration of G-CSF with failure of remission even after months of treatment. Clinical signs of psoriasis were seen positive. Munro micro abscess was also noted in the Biopsy. The patient was initially diagnosed as adverse drug reaction but the failure of complete remission and second round of extensive eruption even after drug cessation made this case unusual. Drug reaction rarely persists after drug cessation and the clinical picture noted was suggestive of early psoriasis.
Key words: Granulocyte colony stimulating factor. G-CSF. Psoriasis. Adverse drug reaction. Neutropenia
CASE REPORT
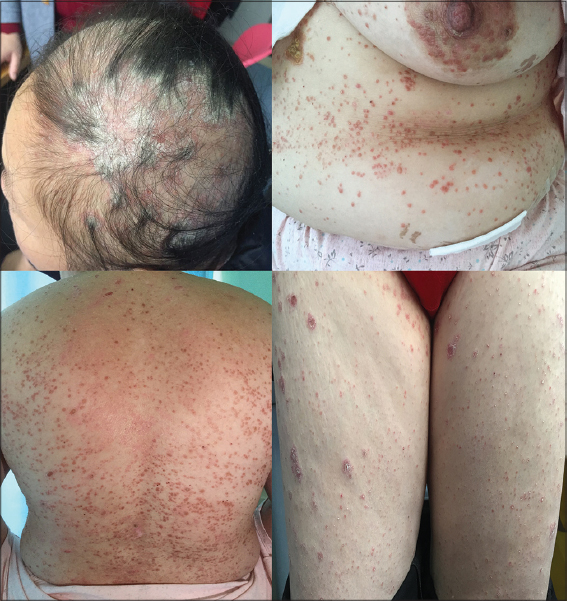
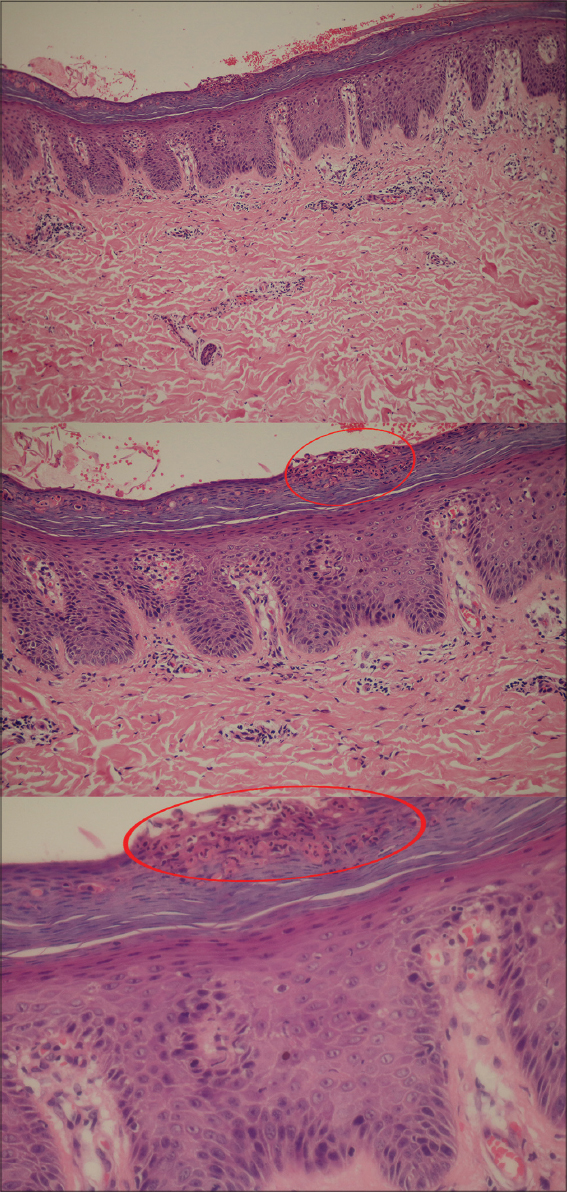
Patient, female, 43 years old, post radical mastectomy and one cycle of chemotherapy presented to the outpatient department of our hospital with extensive erythema, maculopapular rashes and desquamation for two weeks. She had undergone one cycle of chemotherapy (docetaxel 140mg, cyclophosphamide 1140mgdl, q21d) according to the TC regimen with necessary adjuvant therapy. On the tenth day after chemotherapy, the patient developed bone marrow suppression for which the patient was given recombinant Human granulocyte colony-stimulating factor (G-CSF). On the same day of the administration of G-CSF, the patient developed a red rash on the right side of her armpit, which spread to the chest and buttocks, and gradually spread over the whole body including the scalp. Numerous small miliary rashes to large erythematous patches covered with adherent silvery white scales were noted (Fig. 1) with no pruritus or pain. Her lesions were extensive and were increasing rapidly. Newly appeared fresh red rashes as well as faded brown maculopapular rashes, covered with silvery white scales could be observed on the trunk and limbs with positive Film phenomenon and dot bleeding sign (Auspitz sign). Thick white scaly patches were seen on the scalp with fine demarcation extending outside the hairline with scarce hair (Fig.1). The patient had no other significant past medical history and no systemic abnormalities were detected. Biopsy showed hyperkeratosis of the epidermis, parakeratosis, and neutrophil infiltration in the stratum corneum with Munro micro abscess formation, mild spongiotic changes in the epidermis and mild perivascular infiltration in the superficial dermis (Fig. 2). After the comprehensive analysis of patient’s medical history and ongoing chemotherapy it was termed as G-CSF induced drug eruption.
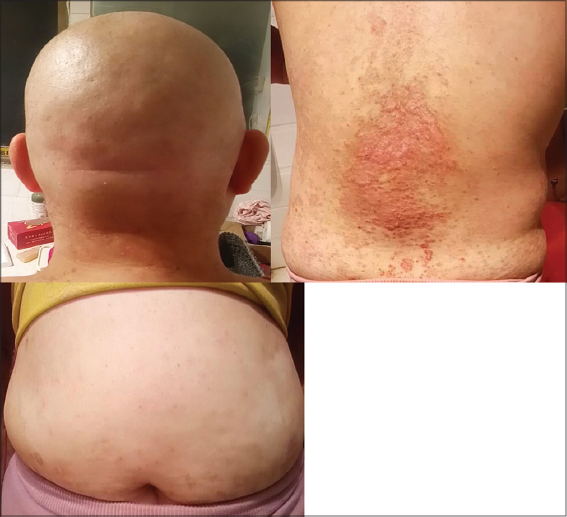
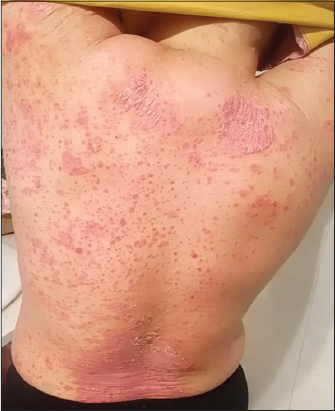
She was then treated with anti-allergic drugs in combination with topical therapies, which showed significant improvement of her rashes with no new eruptions. On follow up after two months, the rashes on her scalp, abdomen and extremities had completely cleared but islands of patches persisted on her back with large erythematous maculopapular rashes without scales (Fig. 3). Therefore, the patient was under simultaneous treatment for her cancer and the rashes. But again after 4 months of initial eruption she had second round of sudden extensive eruption all over her body (Fig. 4). The lesions varied from small red maculopapular rashes to large scaly patches with adherent silvery scales similar to the first episode of eruption. Auspitz sign and film phenomenon were seen positive. Patient however refused to do another biopsy and insisted on supportive management.
Since the second time had no any aggravating factors and the clinical manifestation was favorable for psoriasis. Finally, after overall analysis of the case, the final diagnosis was made as psoriasis induced upon the administration of G-CSF 4 months ago, the initial drug eruption being the early psoriatic presentation.
REFERENCES
1. Fariña MC, Requena L, Dómine M, Soriano ML, Estevez L, Barat A. Histopathology of cutaneous reaction to granulocyte colony-stimulating factor:Another pseudomalignancy. J Cutan Pathol . 1998;25:559-62.
2. Ferran M, Gallardo F, Salar A, Iglesias M, Barranco C, Pujol RM. Granulomatous dermatitis with enlarged histiocytes:A characteristic pattern of granulocyte colony-stimulating factor. Report of two cases and review of the literature. Dermatology . 2006;212:188-93.
3. Chapman A, El Miedany Y. Psoriasis. Comorbidity Rheum Dis . 2017:81-124.
4. Glass LF, Fotopoulos T, Messina JL. A generalized cutaneous reaction induced by granulocyte colony-stimulating factor. J Am Acad Dermatol . 1996;34:455-9.
5. Yokoyama A, Uemura S, Fujino S. Eruption caused by recombinant humanG-CSF. 1994;33:641-3.
6. Cho SG, Park YM, Moon H, Kim KM, Bae SS, Kim GB, et al. Psoriasiform eruption trigerred by recombinant granulocyte-macrophage colony stimulating factor (rGM-CSF) and exacerbated by granulocyte stimulating factor (rG-CSF) in a patient with breast cancer. Korean Med Sci. 1998;13:685-8.
7. Soutter WP, Mcindoe GA, Hospital H, Robert T, Magnetic S, Unit R. Worsening Psoriasis after treatment with g-csf in a patient with small-cell lung cancer serum basic fibroblast growth factor and vascular endothelial growth factor in metastatic renal cell carcinoma treated with interferon alfa-2b. J Natl Cancer Inst. 1997;89:6-7.
8. Glass LF, Fotopoulos T, Messina JL. A generalized cutaneous reaction induced by granulocyte colony-stimulating factor. 1996;68:455-9.
9. Ozaki S, Funasaka Y, Takubo M, Matayoshi T, Ueno T, Asayama T, et al. Granulocyte colony-stimulating factor-induced granulomatous dermatitis with enlarged histiocytes clinically manifesting as painful edematous nodules with high fever similar to Sweet’s syndrome. J Dermatol . 2015;42:414-7.
10. White JML, Mufti GJ, Salisbury JR, Du Vivier AWP. Cutaneous manifestations of granulocyte colony-stimulating factor. Clin Exp Dermatol . 2006;31:206-7.
11. Arbetter KR, Hubbard KW, Markovic SN, Gibson LE, Phyliky RL. Case of granulocyte colony-stimulating factor –induced Sweet’s syndrome. 1999;129:126-9.
12. Yamashita N, Natsuaki M, Morita H, Kitano Y. Cutaneous eruptions induced by granulocyte colony-stimulating factor in two cases of acute myelogenous leukemia. 1993;20:473-7.
13. Mössner R, Beckmann I, Hallermann C, Neumann C, Reich K. Granulocyte colony-stimulating-factor-induced psoriasiform dermatitis resembles psoriasis with regard to abnormal cytokine expression and epidermal activation. Exp Dermatol . 2004;13:340-6.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0001-7046-3711 http://orcid.org/0000-0001-7046-3711 |


Comments are closed.