Umbilical squamous papilloma: A case report
Mehmet Eren Yuksel1, Funda Tamer 2, Guler Senyildiz Hasturk3
2, Guler Senyildiz Hasturk3
1Aksaray University School of Medicine, Department of General Surgery, Aksaray, Turkey; 2Ufuk University School of Medicine, Department of Dermatology, Ankara, Turkey; 3Aksaray University Training and Research Hospital, Department of Pathology, Aksaray, Turkey
Corresponding author: Dr. Funda Tamer, E-mail: fundatmr@yahoo.com
Submission: 16.11.2018; Acceptance: 19.01.2019
DOI: 10.7241/ourd.20194.30
Cite this article: Yuksel ME, Tamer F, Senyildiz Hasturk G. Umbilical squamous papilloma: A case report. Our Dermatol Online. 2019;10(4):408-409.
Citation tools:
BibTex | CSV | RIS | refer/BiblX | Endnote XML
Copyright information
© Our Dermatology Online 2019. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Sir,
A 21-year-old Caucasian male presented with a 2-year history of an asymptomatic mass in the umbilicus. The patient stated that the lesion increased in size gradually. Therefore, the patient was complaining of cosmetic disfigurement. However, he did not receive any treatment previously. The past medical history and family history were both unremarkable. The patient denied any trauma to the umbilical region.
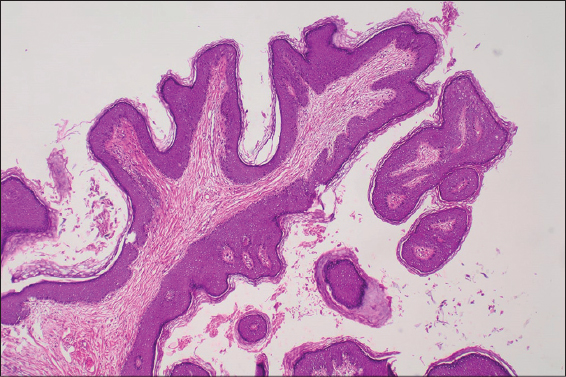
The physical examination of the patient revealed a skin colored pedunculated plaque with verrucous surface in the umbilicus measuring 1.5×1 cm in size (Fig. 1). The lesion was removed surgically under local anesthesia to reach a definitive diagnosis. Histopathological evaluation of the specimen revealed multiple finger-like projections supported by central fibrovascular cores which were covered by a stratified squamous epithelium. The longest diameter of the polipoid lesion was 1.5 cm. However, the diameter of the basis of the lesion was measured 0.4×0.3 cm. No evidence of malignancy or koilocytic changes in the epithelium were observed. The diagnosis of squamous papilloma was made based on clinical and histopathological features (Fig. 2).
 |
Figure 1: Skin colored plaque with verrucous surface in the umbilicus. |
Squamous papilloma is a benign neoplastic proliferation with finger like morphology which usually affects skin, cervix, breast duct, respiratory tract and gastrointestinal tract. Human papilloma virus (HPV) infection plays role in the etiology of squamous papilloma [1].
It has been suggested that stem cell population of the hair follicle which contains keratin 15 might contribute to the development of squamous papilloma. Li et al. investigated the role of keratin 15 + hair follicle cells in the etiopathogenesis of cutaneous papillomas in the Krt1-15CrePR1;R26R transgenic mouse. Li et al. reported that keratin 15 expressing cells contributed to papillomas following 20 weeks of promotion, and persistence of keratin 15 progeny in papillomas [2].
Terada reported a 46-year-old female patient with a squamous papilloma measuring 13 mm in size on the scalp, arising from an epidermal cyst. Squamous papilloma showed intracystic growth with fibrovascular cores. The tumor had benign character, and thus no atypia was observed. Immunohistochemical evaluation showed no association between squamous papilloma and HPV. Terada reported that squamous papilloma could arise in epidermal cysts. Therefore, differential diagnosis of squamous papilloma from trichilemmal tumor and proliferating trichilemmal cyst should be made [3].
Squamous papilloma of the umbilicus is a rare condition. Vijayabhaskar et al. reported a 47-year-old female patient with microinvasive squamous cell carcinoma of the cervix and benign squamous papilloma in the umbilicus at the same time [4]. Nathan reported coexistence of squamous papilloma arising from the umbilicus and genital warts. Nathan suggested possible role of autoinoculation from genital region to umbilicus during bathing [5].
Verrucous carcinoma is a differentiated type of squamous cell carcinoma which presents as a slow growing warty papule. Differential diagnosis of squamous papilloma from verrucous carcinoma is crucial as the verrucous carcinoma can lead to local invasion and metastasis. The risk of misdiagnosis increases in laryngeal lesions and in cases when the biopsy specimen is small [6]. In addition, Kim et al. reported a 20-year-old female patient with condyloma lata in the umbilicus, perineum and mucous patches on the lips. Even it is rare, syphilis should be kept in mind in the differential diagnosis of verrucous nodules in the umbilicus [7].
In conclusion, the patient presented hereby had a lesion diagnosed as squamous papilloma in the umbilicus which was an unusual localization for squamous papilloma. Possible initiating factors such as HPV infection, chronic irritation and rare diseases such as verrucous carcinoma and syphilis in the differential diagnosis of squamous papilloma are reminded through this case report.
Consent
The examination of the patient was conducted according to the Declaration of Helsinki principles.
REFERENCES
1. Goyal E, Gupta P, Dokania A, Rizvi Y. Squamous papilloma over lid margin:An uncommon presentation. Int J Adv Integ Med Scien. 2016;1:128-30.
2. Li S, Park H, Trempus CS, Gordon D, Liu Y, Cotsarelis G, et al. A keratin 15 containing stem cell population from the hair follicle contributes to squamous papilloma development in the mouse. Mol Carcinog. 2013;52:751-9.
3. Terada T. Squamous papilloma and squamous cell carcinoma arising from epidermal cyst:report of 4 cases. Human Pathology Case Reports. 2015;2:55-7.
4. Vijayabhaskar R, Sadasivam OL, Kirushnakumar KS. Papilloma of the umbilicus. Indian J Surg. 2014;76:329-30.
5. Nathan M. Umbilical warts:a new entity?. Genitourin Med. 1994;70:49-50.
6. Cooper JR, Hellquist HB, Michaels L. Image analysis in the discrimination of verrucous carcinoma and squamous papilloma. J Pathol. 1992;166:383-7.
7. Kim JS, Kang MS, Sagong C, Ko JY, Yu HJ. An unusual extensive secondary syphilis:condyloma lata on the umbilicus and perineum and mucous patches on the lips. Clin Exp Dermatol. 2009;34:299 301.
Notes
Source of Support: Nil
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0003-4157-5583 http://orcid.org/0000-0003-4157-5583 http://orcid.org/0000-0002-7110-0717 http://orcid.org/0000-0002-7110-0717 |


Comments are closed.