Ekbom syndrome: a case report
Ines Lahouel 1, Monia Youssef1, Amel Mrad2, Yosra Soua1, Mouna Korbi1, Hichem Belhadjali1, Jameleddine Zili1
1, Monia Youssef1, Amel Mrad2, Yosra Soua1, Mouna Korbi1, Hichem Belhadjali1, Jameleddine Zili1
1Dermatology Department, Fattouma Bourguiba Hospital, 5000 Monastir, Tunisia; 2Psychiatry Department, Fattouma Bourguiba Hospital, 5000 Monastir, Tunisia
Corresponding author: Dr. Ines Lahouel, E-mail: lahouel.iness@gmail.com
Submission: 12.09.2018; Acceptance: 30.11.2018
DOI: 10.7241/ourd.20193.30
Cite this article: Lahouel I, Youssef M, Mrad A, Soua Y, Korbi M, Belhadjali H, Zili J. Ekbom syndrome: a case report. Our Dermatol Online. 2019;10(3):315-316.
Citation tools:
BibTex | CSV | RIS | refer/BiblX | Endnote XML | Wikipedia Citation Templates
Copyright information
© Our Dermatology Online 2019. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Sir,
Ekbom Syndrome is also called delusory parasitosis, psychogenic parasitosis, or dermatozoic delusion [1]. It is an uncommon psychiatric condition, characterized by the continuous belief of being infested by parasites, although no medical evidence of infestation is found [2]. These patients seek advice from multiple practitioners and various specialties are often involved. They generally refuse psychiatric referral or treatment, and often refer to dermatologists.
We describe one case of a patient with delusory parasitosis who consulted many dermatologists for pruritic skin lesions.
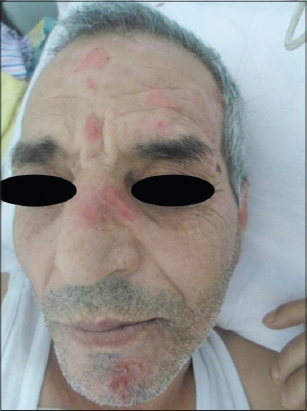
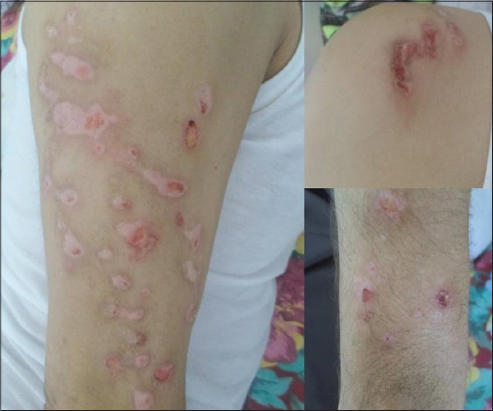
A 56-year-old man presented to our clinic with a four-month history of recurrent pruritic papular eruption evolving in erosive lesions covered by crusts. The lesions had begun on his face, and gradually progressed to his upper arm. The disease was reported as heavily troublesome, and significantly impaired the everyday activities of the patient. He had a history of choroidal melanoma diagnosed 7 years ago and treated by protontherapy. There were no local or systemic complications of his melanoma. The man denied any drugs intake. The patient had been seen by several physicians and had experienced different treatments without improvement. Physical examination revealed several erosions, hematic and serous crusts on a slightly erythematous background. The lesions were located on the left half of the face (Fig. 1), and the right upper limb (Fig. 2). No other significant skin or mucosal lesions were seen. General examination was otherwise unremarkable. No primary dermatological diagnosis was made. Skin biopsy showed chronic nonspecific inflammation of the dermis. The patient underwent routine biochemistry assays, research for parasites, chest-X-ray, abdomen ultrasonography and brain CT-scan. All those diagnostic procedures provided negative. At a more detailed interview, the patient reported that there are small living creatures in his skin which cause the itching. A psychiatrist was consulted, who diagnosed an Ekbom’s syndrome. The lesions were provoked by the patient who was trying to eliminate the parasites of his skin. The patient was treated by anti psychotic drugs associated to psychotherapy with good evolution.
Delusory parasitosis is uncommon psychiatric disorder that may represent a challenge for the dermatologist, as it was in our case. It is characterized by the fixed belief to be infested with parasites or small living creatures, although there is no medical evidence for this [1–2].
The Ekbom syndrome is relatively rare. The majority of the patients are women. The average age at the beginning of the disease is 55,6 years [3].
Patients usually experience itching, which they attribute to the presence of animals in or under the skin. They often try to self-treat the disorder by scratching or by using disinfectants or pesticides. This causes skin lesions and itching, which in turn confirm the patient’s belief of being infested and leads to a vicious circle of skin lesions, itching and delusional beliefs [2]. Cutaneous lesions are various, including discreet bruises, nodular pruritus and even ulcers and scars [3]. Like in the case presented, skin lesions typically predominate in those body regions that can be easily reached, whereas the body sides opposite to the patient’s handedness lesions are usually absent.
There are many psychiatric disorders associated such as anxiety, phobia, hypochondria, non-organic and organic delirious disorder [3].
Some cases are associated to organic diseases like hypothyroidism, diabetes, cortical lesions, mental retardation, kidney failure, hepatitis, severe anemia, intoxication by medication and cardiopathies, substance abuse, infectious and endocrine disorders [3].
The management of this condition is difficult, as patients with this disorder reject psychiatric diagnosis and treatment and often consult many specialists (dermatologists, internists or allergists). Antipsychotic drugs lead to improvement; pimozide was recommended as the drug of choice. Full remission is obtained in only half of the cases with antipsychotic treatment. Psychotherapy support is also needed [4].
Delusory parasitosis must be known by the dermatologist. This syndrome requires a multi-disciplinary approach.
Consent
The examination of the patient was conducted according to the Declaration of Helsinki principles.
REFERENCES
1. Hinkle NC, Ekbom syndrome: the challenge of “invisible bug” infestationsAnnu Rev Entomol 2010; 55: 77-94.
2. Lombardi C, Belli D, Passalacqua G, When allergology meets psychiatry: delusional parasitosis (Ekbom’s syndrome)Eur Ann Allergy Clin Immunol 2011; 43: 89-91.
3. Alves CJ, Martelli AC, Fogagnolo L, Nassif PW, Secondary Ekbom syndrome to organic disorder: report of three casesAn Bras Dermatol 2010; 85: 541-4.
4. Bellanger AP, Crouzet J, Boussard M, Grenouillet F, Sechter D, Capellier G, Ectoparasitosis or Ekbom syndrome?A case reportCan Fam Physician 2009; 55: 1089-92.
Notes
Source of Support: Nil
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
|


Comments are closed.