Sclerema neonatorum in a premature newborn
Barbach Younes , Chaouche Mohammed, Dah Cherif Abdellah, Elloudi Sara, Baybay Hanane, Mernissi Fatima Zahra
, Chaouche Mohammed, Dah Cherif Abdellah, Elloudi Sara, Baybay Hanane, Mernissi Fatima Zahra
Departement of Dermatology, CHU Hassan II, Fès, Morocco
Corresponding author: Dr. Barbach Younes, E-mail: dr.younes2011@gmail.com
Submission: 23.09.2018; Acceptance: 03.12.2018
DOI: 10.7241/ourd.20193.22
Cite this article: Younes B, Mohammed C, Abdellah DC, Sara E, Hanane B, Zahra MF. Sclerema neonatorum in a premature newborn. Our Dermatol Online. 2019;10(3):300-301.
Citation tools:
BibTex | CSV | RIS | refer/BiblX | Endnote XML | Wikipedia Citation Templates
Copyright information
© Our Dermatology Online 2019. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Sclerema of the newborn is classified among the lobular panniculitis, it is an extremely rare affection, most often lethal which occurs on a weak ground or sepsis [1]. The sclerema was announced for the first time at the beginning of the XVIIth century and the most authors have confused it with the scleroedema and cytosteatonecrosis of the newborn so the most diverse names have been given to these three conditions combined. Several theories have been proposed to explain his pathogenesis, which remains poorly understood [2]. The diagnosis of sclerema is clinical, it is manifested in newborns during their first week of life by a generalized cutaneous induration which gradually achieves, within a few days, a diffuse sclerous skin condition very paradoxically respecting the hands and feet, but may extend to compromising life-threatening dietary and respiratory functions. Sclerema treatment is based on newborn conditioning, antibiotic therapy, systemic corticosteroids, exsanguino-transfusion and currently the advent of intravenous immunoglobulins. Despite these treatments, the prognosis of sclerema remains reserved with a high rate of mortality [3].
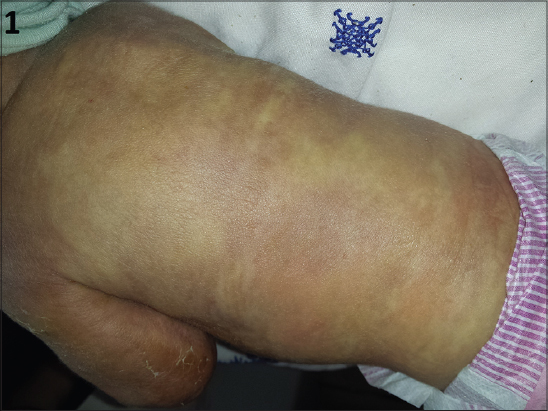
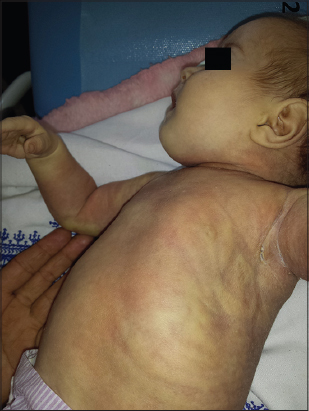
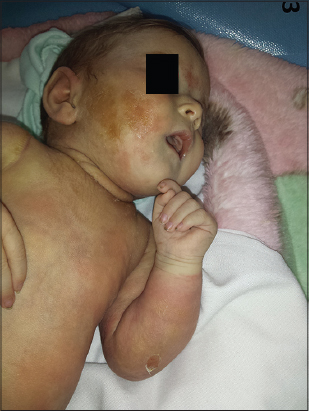
We report the case of a premature infant on D10 of life, hospitalized in neonatology for acute respiratory distress, which had since birth an induration of the diffuse skin. Dermatological examination showed the presence of a generalized sclerosis taking the whole body respecting the genitals as well as the palmo-plantar region [Figs. 1–3], the diagnosis of newborn sclerema was retained after eliminating other diagnoses including neonatal cytosteotonecrosis and scleroderma, and then was put on cortico antibiotic combination.
Consent
The examination of the patient was conducted according to the Declaration of Helsinki principles.
REFERENCES
1. Park SH, Kim S-C, Sclerema neonatorum in a full-term infant showing favorable prognosisAnn Dermatol 2017; 29: 790-3.
2. Shrestha S, Chaudhary N, Koirala S, Gupta R, Sclerema neonatorum treated successfully with parenteral steroids: an experience from a resource poor countryCase Rep Pediatr 2017; 2017: 1-2.
3. Zeb A, Darmstadt GL, Sclerema neonatorum: a review of nomenclature, clinical presentation, histological features, differential diagnoses and managementJ Perinatol Off J Calif Perinat Assoc 2008; 28: 453-60.
Notes
Source of Support: Nil
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/000-0003-3455-3810 http://orcid.org/000-0003-3455-3810
|


Comments are closed.