Dermatology Eponyms – sign –Lexicon (T). Part 2
Piotr Brzeziński 1,2, Lorenzo Martini2, Beatriz María Di Martino Ortiz3, Vijaya Sajjan4, Masashi Narita5, Yuko Ono6, Ramesh Parajuli7, Biswajit Dey8, Guilherme Moraes Krüger9, Patrice Bourée10
1,2, Lorenzo Martini2, Beatriz María Di Martino Ortiz3, Vijaya Sajjan4, Masashi Narita5, Yuko Ono6, Ramesh Parajuli7, Biswajit Dey8, Guilherme Moraes Krüger9, Patrice Bourée10
1Institute of Biology and Environmental Protection, Department of Cosmetology, Pomeranian Academy, Slupsk, Poland; 2University of Siena, Department of Pharmaceutical Biotechnologies, Via A. Moro 2, 53100 Siena, Italy; 3Department of Dermatology, Clinicas Hospital, Faculty of Medical Sciences, National University of Asuncion, Paraguay; 4Department of Dermatology, Venereology and Leprosy, Jawaharlal Nehru Medical College, Belgaum, Karnataka, India; 5Department of Medicine, Ohta Nishinouchi General Hospital, Nishinouchi 2-5-20 Koriyama, Fukushima, Japan; 6Critical Care Center, Ohta General Hospital Foundation, Ohta Nishinouchi Hospital 2-5-20 Nishinouchi, Koriyama, Fukushima, Japan; 7Department of Otorhinolaryngology, Chitwan Medical College Teaching Hospital, Chitwan, Nepal; 8Department of Pathology, Andaman and Nicobar Islands Institute of Medical Sciences, Port Blair, Andaman and Nicobar; 9Dermatology Service of the Universidade Federal do Mato Grosso do Sul (UFMS) – Campo Grande (MS), Brazil; 10Unité des maladies parasitaires, Hôpital Cochin, 75014 Paris, France
Corresponding author: Dr. Piotr Brzeziński, E-mail: brzezoo77@yahoo.com
Submission: 07.12.2018; Acceptance: 12.03.2019
DOI:10.7241/ourd.20192.35
Cite this article: Brzeziński P, Martini L, Di Martino OB, Sajjan V, Narita M, Ono Y, Parajuli R, Dey B, Krüger GM, Bourée P. Dermatology Eponyms – sign –Lexicon (T). Part 2. Our Dermatol Online. 2019;10(2):224-228.
Citation tools:
BibTex | CSV | RIS | refer/BiblX | Endnote XML | Wikipedia Citation Templates
Copyright information
© Our Dermatology Online 2019. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Eponyms are used almost daily in the clinical practice of dermatology. And yet, information about the person behind the eponyms is difficult to find. Indeed, who is? What is this person’s nationality? Is this person alive or dead? How can one find the paper in which this person first described the disease? Eponyms are used to describe not only disease, but also clinical signs, surgical procedures, staining techniques, pharmacological formulations, and even pieces of equipment. In this article we present the symptoms starting with (T) and other. The symptoms and their synonyms, and those who have described this symptom or phenomenon.
Key words: Eponyms, Skin diseases, Sign, Phenomenon
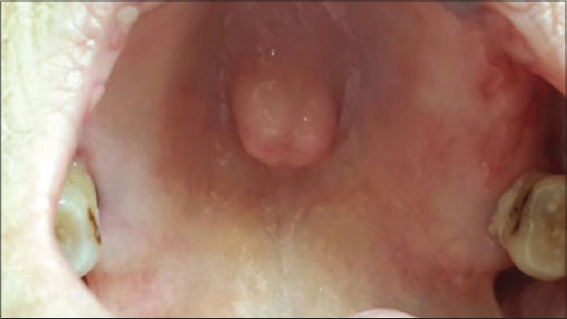
TORI SIGN
Hyperostosis occuring in the midline of the hard palate (Fig. 1), called torus palatinus or hyperostosis located on the lingual aspect of the mandible, termed torus mandibularis [1].
TRAMP STAMP SIGN
Tattoos on women that are not religious or ceremonially required for their culture. Often on the lower back area; they were originally used to signify a life of prostitution. This practice continues today but sometimes these tattoos are now seen in the non-prostitute population, as sign of admiration for the romanticized prostitution lifestyle which is linked to drug abuse, physical violence, and sexually transmitted diseases. The origin of the term dates from the 17th century Yakuza practice of tattooing prostitutes on the back. Prostitutes in the Edo period, called ‘Yujo’ tattooed themselves with the name of their regular customer as a sign of their loyalty. This tattoo is referred to as ‘Irezumiko’, which starts with the customer’s name and ends with the kanji character (inochi), which means life, so this tattoo means “I give my life to ‘name’.”
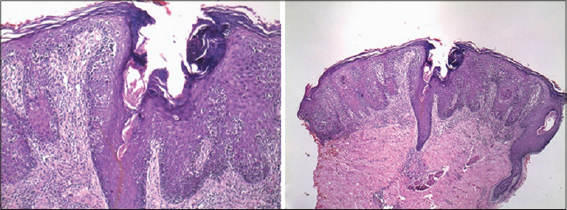
TOY SOLDIER SIGN
Linear aggregation of neoplastic lymphocytes along the dermal-epidermal junction seen in histopathology of mycosis fungoides (Fig. 2) [2].
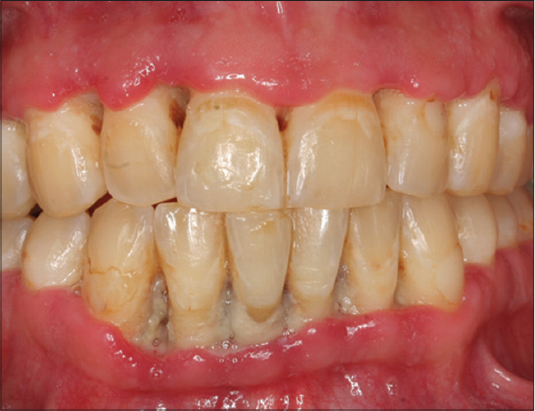
TRENCH MOUTH SIGN
Linear gingival erythema, an erythematous band an the free gingiva that follows the contour with a reddish chevron appearance (Fig. 3). An indication of HIV disease [3–6]. Painful, acute necrotizing ulcerative gingivitis. Also called HiVR and NUP signs, ulceromembranous gingivitis, Vincent’s infection, Vincent’s War sign, and ANUG sign.
HENRI VINCENT
French physician, 1862-1950. His name is associated with Vincent’s Disease or Vincent s Angina. It is also widely known as Trench Mouth, due to an outbreak in soldiers in trenches during World War One. Borrelia vincentii used to be spread out worldwide, but is now mainly in countries that are not very developed [3,4].
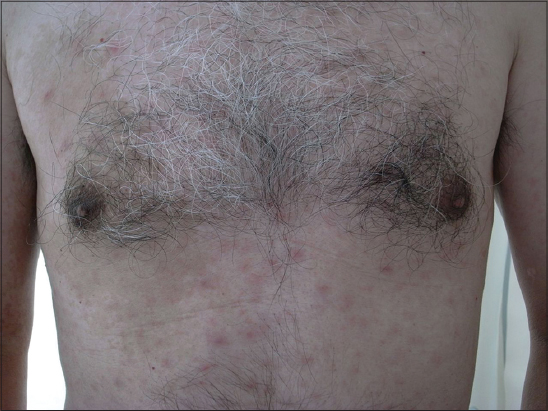
TSUTSUGAMUSHI SIGN
An epidemic disease of Japan due to a zoonotic proteus implanted by the bite of a mite (kedani). It is marked by fever, swelling of the lymph-glands, and an exanthematous eruption fever [7]. Synonym: akamushi disease, flood fever, inundation fever, island disease, island fever, Japanese river fever, kedani fever, mite typhus, scrub typhus (Fig. 4), shimamushi disease, tropic typhus, tsutsugamushi.
TUBERCULOUS ULCER SIGN
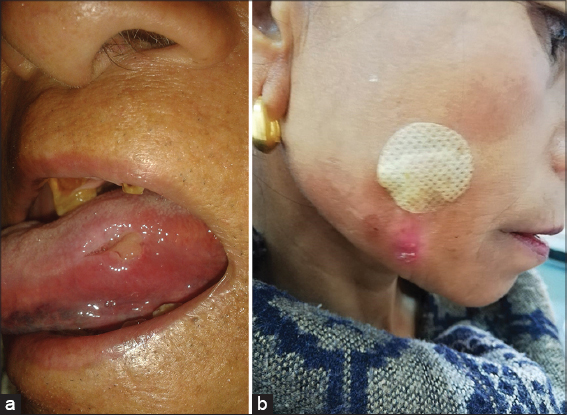
An ulcer that is characterized by undermined edges and is usually painful (Figs. 5A and B) [8,9].
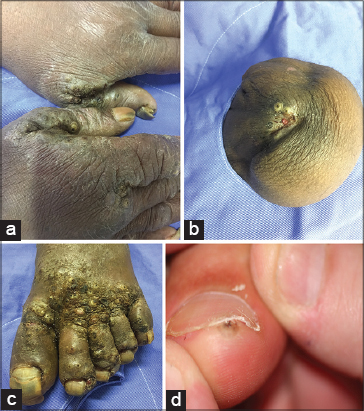
TUNGA EYE SIGN
A skin boil that has the resemblance of a small eye (Fig. 6). It can have a 10mm white area with a black center. The black center is the abdomen’s caudal tip of the parasitic chigoe flea that has burrowed into the skin to lay eggs [10,11].
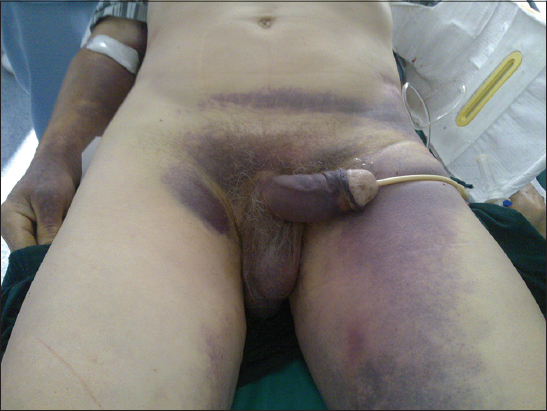
TURNER’S SIGN
Discoloration (bruising) of the skin of the loin in acute hemorrhagic pancreatitis; adverse prognostic (Fig. 7). Also known as Grey Turners sign [12].
GEORGE GREY TURNER
English surgeon, 1877-1951 (Fig. 8). Served with the Royal Army Medical Corps in the First World War. First described in 1920 Grey Turner’s sign, in the British Journal of Surgery, it was described as a sign of hemorrhagic pancreatitis. As a young surgeon, he travelled around the world, being received by the Pope, Benito Mussolini, the King of Italy and King Alfonso of Spain. Five years before his death, Grey Turner was made President of the International Society of Surgeons. After the war, Grey Turner was briefly famous for performing one of the earliest operations to attempt the removal of a bullet from a soldier’s heart. The bullet was never removed, but Grey Turner’s surgery saved the patient’s life. Worked with early cancer research, and anticipated the development of chemotherapy [12].
TWIN NEVUS PHENOMENON (TWIN-SPOTTING’ PHENOMENON)
The ‘twin-spotting’ phenomenon due to loss of heterozygosity and somatic recombination during late embryogenesis. The earlier the mutation during embryogenesis, the wider is the involvement of the skin, central nervous system and other structures, and, in contrast, later postzygotic mutations generate only skin involvement. Twin spotting phenomenon of Happle and Steijen has been proposed to explain this phenomenon (Phakomatosis pigmentovascularis) [13–15]. In this hypothesis, somatic mutations on nearby genes leads to mosaic spots in close proximity to one another. Phakomatosis pigmentovascularis has been classified into four types namely; type I: Nevus flammeus and epidermal nevus, type II: Nevus flammeus, Mongolian spots, ± nevus anemicus, type III: Nevus flammeus, nevus spilus, ± nevus anemicus, and type IV: Nevus flammeus, Mongolian spots, nevus spilus, ± nevus anemicus.
TWO GLASSES SIGN
This is sign in gonerrhea. It should be remembered that purulent leakage from the coil is not enough to definitively diagnose the disease, because it can also be caused by many other causes. Confirmation of anterior urethral involvement may be so-called try two glasses. It consists in the fact that if the urine is put into two glasses, it will be cloudy in the first glass and in the second glass it will be transparent. The cloudy urine in both glasses indicates that the rear coil is also occupied.
TWORT-D’I IERELLE SIGN
The phenomenon of transmissible bacterial lysis; bacteriophagia. When to a broth culture of typhoid or dysentery bacilli there is added a drop of filtered broth emulsion of the stool from a convalescent typhoid or dysentery patient, complete lysis of the bacterial culture will occur in a few hours. If a drop of this lysed culture is added to another culture of the bacilli, lysis will take place exactly as in the first. A drop of this culture will then dissolve a third culture, and so on through hundreds of transfers, d’I Ierelle attributes this phenomenon to the action of an ultramicroscopic parasite of bacteria which he named the bacteriophage [16].
FREDERICK WILLIAM TWORT
British bacteriologist, 1877-1950 (Fig. 9). Fellow of the Royal Society was an English bacteriologist and was the original discoverer in 1915 of bacteriophages (viruses that infect bacteria). He studied medicine at St Thomas’s Hospital, London, was superintendent of the Brown Institute for Animals (a pathology research centre), and he was also professor of bacteriology at the University of London. He researched into Johne’s disease, a chronic intestinal infection of cattle, and also discovered that vitamin K is needed by growing leprosy bacteria [17].

FELIX HUBERT D’HERELLE
French-Canadian microbiologist, 1873-1949 (Fig. 10). Generally known as the discoverer of the bacteriophage, a virus that infects bacteria. He experimented with the possibility of phage therapy. D’Herelle has also been credited for his contributions to the larger concept of applied microbiology. After studying medicine in Paris and Leiden, Hérelle went to Guatemala City to direct the bacteriology laboratory of the municipal hospital and teach microbiology at the local medical school. In 1909 he was sent by the Mexican government to study microbiology at the Pasteur Institute in Paris. While there, he experimented with a bacterium known to cause enteritis (digestive tract inflammation) in certain insects. In the course of his work Hérelle occasionally noticed clear spots (areas free of bacteria) on gelatin cultures of the bacterium under study. Subsequently he investigated a form of dysentery afflicting a French cavalry squadron during World War I, and he happened to mix a filtrate of the clear areas with a culture of dysentery bacteria. The bacteria were quickly and totally destroyed by an unknown agent in the filtrate that Hérelle termed an “invisible microbe”; he later renamed it a bacteriophage [18].
TYNDALL PHENOMENON
Tyndall effect blue appearance of melanin in dermal lesions due to selective light absorption [19,20].
TYPHUS SIGN
A rash that spreads from the armpits to the chest, abdomen, and thighs [21]. A sign of Typhus.
REFERENCES
1. Re Domínguez ML, Riveros R, Moreno T, Di Martino Ortiz BM, Rodríguez Masi M, Knopfelmacher O, et al. Torus palatinus. Report of two cases. Our Dermatol Online. 2016;7:169-71.
2. Sajjan V, Chandela M, Pandit AM, Manjunathswamy B. Mycosis fungoides:The great imitator. Our Dermatol Online. 2015;6:76-9.
3. Brzeziński P, Sinjab AT, Campbell CM, Kentorp N, Sand C, Karwan K. Dermatology Eponyms –phenomen/sign –Lexicon (supplement). Our Dermatol Online. 2012;3:147-55.
4. Brzeziński P, Pessoa L, Galvão V, Barja Lopez JM, Adaskevich UP, Niamba PA, et al. Dermatology Eponyms –Sign –Lexicon –(H). Our Dermatol Online. 2013;4:130-43.
5. Brzezinski P, Chiriac A, Rath SK. Dermatology Eponyms –Sign –Lexicon –(M). Our Dermatol Online. 2014;5:442-7.
6. Brzezinski P, Chiriac A, Arenas R, Dori GU, Monteiro R, Cairncross S, et al. Dermatology Eponyms –Sign –Lexicon –(L). Our Dermatol Online. 2014;5:217-30.
7. Brzezinski P, Fiorentino DF, Arunachalam P, Katafigiotis I, Matuszewski Ł, Narita M, et al. Dermatology Eponyms –Sign –Lexicon –(K). Our Dermatol Online. 2014;5:95-102.
8. Parajuli R, Maharjan S. Tubercular ulcer of tongue in an elderly patient masquerading as a traumatic ulcer. Case Rep Otolaryngol. 2017;2017:8416963.
9. Rana S, Monga S, Khan S, Khetrapal S, Jetley S. Tubercular abscess of the lower lip:a rare case of mistaken identity. Our Dermatol Online. 2014;5:169-71.
10. Krüger GM, Loro LS, Takita LC, Hans G Filho. Disseminated tungiasis. An Bras Dermatol. 2017;92:727-8.
11. Martini L. The way to cure a complicate syndrome caused by an insect (parasite) using a cerumen extracted from another insect (no parasite, that lives in some countries where the fi rst disease is endemic). Our Dermatol Online. 2018;9:140-3.
12. Brzezinski P, Sinjab AT, Masferrer E, Gopie P, Naraysingh V, Yamamoto T, et al. Dermatology Eponyms –sign –Lexicon (G). Our Dermatol Online. 2012;3:243-57.
13. Jehangir M, Quyoom S, Bhat J, Sajad P, Sofi I, Amin A, et al. Phakomatosis pigmentovascularis with lower limb vascular abnormalities in a young Kashmiri male child-Report of a first child from Kashmir Valley (India) and review of literature. Our Dermatol Online. 2016;7:87-90.
14. Happle R Allelic somatic mutations may explain vascular twin nevi. Hum Genet. 1991;86:321-2.
15. Karia DR, Solanki AN, Jagati AG, Shah BJ. Phacomatosis pigmentokeratotica:A very rare twin spotting phenomenon. Indian J Dermatol Venereol Leprol. 2018;84:120.
16. Zavil’gel’ski?GV, Kotova VIu, Rastorguev SM. [Antimodification activity of the ArdA and Ocr proteins]. Genetika. 2011;47:159-67.
17. Thomas GH. Frederick William Twort:Not just bacteriophage. Microbiology Today. 2014;41:70-3.
18. Summers WC Félix Hubert d’Herelle (1873-1949):History of a scientific mind. Bacteriophage. 2017;6:e1270090.
19. Xue R, Valdebran M, Terrero D, Yang B. Plaque with pearly raised borders on the forearm. Our Dermatol Online. 2016;7:103-4.
20. Valdebran M, Salinas RI, Ramirez N, Rodriguez A, Guzman L, Marte S, et al. Fixed drug eruption of the eyelids. A dermoscopic evaluation. Our Dermatol Online. 2013;4:344-6.
21. Brzeziński P, Passarini B, Nogueira A, Sokołowska-Wojdyło M. Dermatology eponyms –phenomen/sign –dictionary (C). N Dermatol Online. 2011;2:81-100.
Notes
Source of Support: Nil
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0001-6817-606X http://orcid.org/0000-0001-6817-606X http://orcid.org/0000-0002-5953-3042 http://orcid.org/0000-0002-5953-3042 http://orcid.org/0000-0003-1296-2103 http://orcid.org/0000-0003-1296-2103
|




Comments are closed.