Pruritic papular eruption of HIV: a review article
Obioma Ekpe 1, Gerald Dafe Forae2, Chibuzor Ifeanyi Okpala3
1, Gerald Dafe Forae2, Chibuzor Ifeanyi Okpala3
1Department of Internal Medicine, Federal Medical Centre Umuahia, Umuahia, Nigeria; 2Department of Pathology, University of Benin Teaching Hospital, Benin, Nigeria; 3Department of Internal Medicine, Nnamdi Azikiwe University Teaching Hospital, Nnewi, Nigeria
Corresponding author: Dr. Obioma Ekpe, PhD, E-mail: uncleprinceo@gmail.com
Submission: 26.11.2018; Acceptance: 27.01.2019
DOI:10.7241/ourd.20192.22
Cite this article: Ekpe O, Forae GD, Okpala CI. Pruritic papular eruption of HIV: a review article. Our Dermatol Online. 2019;10(2):191-196.
Citation tools:
BibTex | CSV | RIS | refer/BiblX | Endnote XML | Wikipedia Citation Templates
Copyright information
© Our Dermatology Online 2019. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Pruritic papular eruptions (PPE) are characterized by chronic pruritus and symmetric papular eruptions on the trunk and extremities, with absence of other definable causes of itching in an HIV-infected patient. The face may be involved in some patients and the condition tends to wax and wane. Systemic review of existing literature on PPE-HIV was carried out using original articles, review articles, case reports and Cochrane library data. Articles selected for inclusion in this review were evaluated critically with regards to their impact factor, source and evidenced based contribution on this topic as measured by their citation and the journals they were published in. Pruritic papular eruption is a frequent cause of substantial morbidity in HIV patients with varying geographical prevalence that ranged between 11% and 46%. Cases of PPE reported in men and women were approximately of equal frequency. Most patients with PPE-HIV have been observed resistant to treatment. In some regions, particularly in sub-Saharan Africa, PPE-HIV is often the presenting symptom of HIV infected patient and therefore may play a role in the diagnosis of HIV, especially in poor resource setting.
Key words: Pruritic papular eruption, HIV, Sub-Saharan Africa, Pruritic rash
INTRODUCTION
Itching is a common complaint among HIV patients and may cause significant morbidity and embarrassment. In most patients, careful history and physical examination will show that dermatosis accounts for their pruritus [1,2]. Pruritic papular eruption associated with Human Immunodeficiency Virus infection (PPE-HIV), was described by James et al in 1985 as a chronic pruritic papular dermatitis seen in patient suffering from Acquired Immunodeficiency Syndrome (AIDS) [3]. And this skin condition remains the most common cutaneous manifestation in the HIV-infected patient and it is more prevalent in developing countries [4–10].
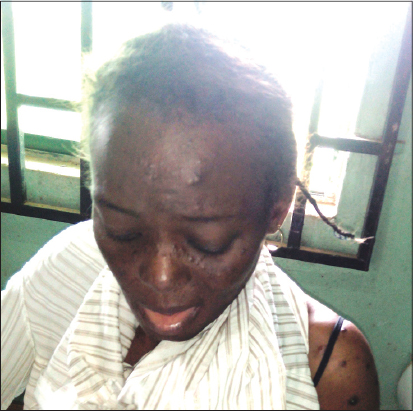
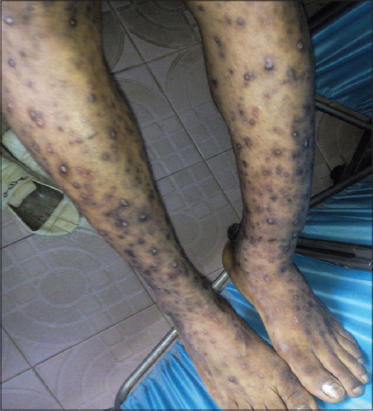
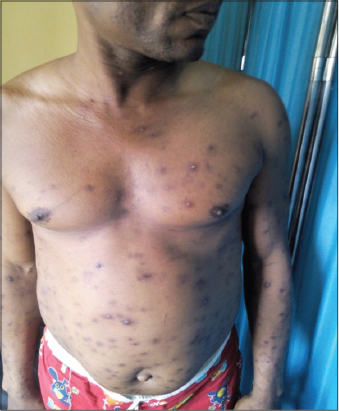
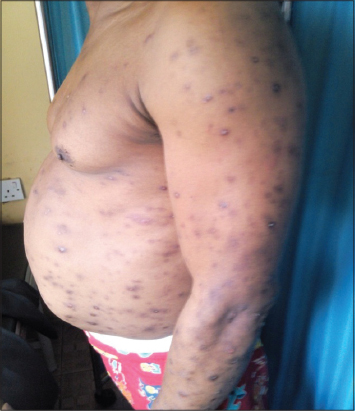
Pruritic papular eruption of HIV manifests as chronic waxing and waning intensely pruritic papules located predominantly on the extremities and trunk as shown in Figs. 2, 3, 4 and 5. Although facial involvement can also occur (Fig. 1). The resulting excoriations and hyperpigmentary changes can be distressing, disfiguring and stigmatizing for patients [11].
PPE-HIV is regarded as WHO clinical stage II for infants and children [12] however in adults, PPE manifest in advanced immunosuppressive stage with low CD4 count in majority of cases, but they may appear as an initial cutaneous disease with high CD4 count [13].
Epidemiology of PPE
Pruritic papular eruption of HIV (PPE-HIV), has been well described in some sub-Saharan Africa countries and elsewhere, with varying geographical prevalence. Report of PPE emerged early in the course of the HIV epidemic. Beginning in 1983, studies in Democratic Republic of Congo (formerly called Zaire) [14], Mali [4], Zambia [9], Tanzania [5], Nigeria [6], Togo [7] and other Africa countries described an extremely pruritic diffuse skin eruption occurring in HIV infected patient.
Reported PPE prevalence among HIV-positive patients ranged between 11% and 46%; with Southern Florida USA having a prevalence of 11% [15], Haiti 46% [8], Thailand 33-37% [16,17], hospitalized patients in Zaire 18% [10], Kenya 5% [18] and 16.7% in Nigeria [19].
There are few reported cases of pruritic papular eruption of HIV in United States of America (USA), except in areas with high mosquito prevalence such as Southern Florida [20], where a PPE prevalence of 11% was reported by Goldstein et al [15]. In a study done in Haiti on HIV patients who had pruritic skin lesions, Lautaud et al [8] found generalized PPE in 62 (46%) of 134 of Haitians examined. Sivayathorn et al [16] conducted a detailed study of the skin lesions of 248 patients infected with the human immunodeficiency virus (HIV) in Bangkok, Thailand and found a prevalence of PPE of 33%. Lowe et al [21] studied 139 HIV positive adolescents in Zimbabwe with cutaneous manifestations of HIV and found PPE to be the most common HIV skin condition seen in 42% of patients. Colebunder et al [10] studied the generalized papular pruritic eruption in African patients with HIV infection in Zaire (Democratic Republic of Congo), it was reported that out of 284 patients hospitalized with HIV infection, 18% presented with a generalized pruritic papular eruption. No significant association between this eruption and other HIV manifestation or any opportunistic infection was found. In a study done in Kenya by Ramadhan L Mawenzi et al [18] on the epidemiology and clinical spectrum of cutaneous disease manifesting among newly diagnosed HIV seropositive adult in Nakuru County-Kenya; it was reported that out of 394 newly diagnosed HIV patients seeking care at the Rift Valley Provincial Hospital in Kenya, 20 patients (5%) had PPE. Akinboro and Onayemi et al [22] in Osogbo southwest Nigeria, conducted a research on the pattern and extent of skin disease in relation to CD4 cell count among adult with HIV infection or AIDS in 2012 and they found the prevalence of PPE to be 19%. Ukonu and Eze [19], studied the pattern of skin disease at the University of Benin Teaching Hospital, Benin city, Nigeria and revealed that out of 4,786 patients seen in the dermatology and venerology clinic of the hospital over a 12 month period, 16.7% had PPE-HIV.
In addition to its presence in large number of patient, PPE is often one of the early cutaneous manifestation of HIV. Liautaud et al [8], in a study of PPE-HIV in Haitian patients, observed pruritic papular skin lesion as the initial symptom in 70% of patients and similar findings were described in Democratic Republic of Congo, by Colebunder et al [10], where 51% reported that the skin eruption was their initial manifestation of HIV. The cases of PPE reported in men and women were approximately of equal frequency [10], however Ramadhan et al [18] in Kenya reported that 70% of patients with PPE were female.
Pathogenesis of PPE
The pathogenesis of PPE-HIV remains unclear, although several etiologies have been proposed [23,24]. An altered and exaggerated hypersensitivity response to arthropod bite has been implicated as suggested by an increase in local and peripheral eosinophilia as well as an increase in immunoglobin E (lgE) levels, with involvement of uncovered skin and histologic finding consistent with arthropod bites in these patients [11,25]. Aires et al [26], studied the role of cytokines in PPE-HIV in Brazil and revealed lower levels of interleukin 2 (IL-2) and gamma interferon (γ-IFN) in HIV infected patients with the PPE compared with other HIV infected patients without the eruption. Moreover, they also reported a higher level of interleukin 2 (IL2), interleukin 12 (IL12), gamma interferon (γ-IFN) and interleukin 5 (IL5) in patients with PPE-HIV when compared to HIV-negative group. These led to the suggestion that immune dysregulation in the setting of chronic HIV infection could be responsible for the eruption [23].
A drug reaction has been proposed by some authors as a possible etiology of PPE, but it is unlikely given that inciting medications that predate the onset of PPE-HIV have not been consistently identified in patient with PPE [20]. Direct HIV infection of the skin has been suggested. This is because PPE have been shown to have good response to HAART by some researchers [27]. An observational study conducted in 2008 reported that 27 out of 29 patients with PPE had resolution of their skin lesions and two patients reported a reduction in its severity within 24 months of antiretroviral therapy (ART) [27]. As a consequence of PPE response to ART, new-onset, recurrent or worsening PPE has been proposed as part of an algorithmic approach to the clinical evaluation of treatment failure after at least 6-months of ART [28,29].
Clinical Features of PPE
Patients with PPE-HIV typically present with multiple, discrete and skin colored papules that are often eroded from scratching. Lesions are commonly distributed on the extensor surfaces of the arms and legs, the dorsum of the hands (Figs. 2–4), the trunk and face as shown in figures 5, 6, 7 and 1 [13]; but sparing the mucous membranes including the palms and soles [23]. The papules may be erythematous, and do not form confluent plaques. Pustules are infrequently present. Many patients will scratch to the point of extensive excoriation with subsequent scarring. In patient with darker skin tones, post-inflammatory hyperpigmentation is often the most visible manifestation.
An inverse relationship between the absolute CD4 cell count and the prevalence and symptom severity of PPE has been reported [30]. Symptoms have been found more often in patient with advanced HIV disease. Nnoruka et al [31], in Southeast Nigeria found PPE to occur in those with lower immune status with CD4 count that was less than 200 cell/ul. A study of 120 HIV-positive patients in Thailand found zero cases of PPE in those with CD4 Count of >500 cell/ul. In contrast, PPE was found in 34% of patient with CD4 Counts between 200 and 499 cell/ul and 81% of patient with CD4 Count of <200 cell/ul, showed evidence of PPE [17]. Boonchia et al [30] in 1999 studied the relationship between PPE and immune status of HIV patients and he discovered that 81.25% of PPE patients had advanced immunosuppression with CD4 count less than 100 cells/ul and 75% had CD4 Count less than 50 cell/ul. They concluded that PPE is a cutaneous marker of advanced HIV infection. Other researchers have also observed a significant relationship between PPE and low CD4 counts [15,18].
The clinical presentation of Eosinophilic folliculitis is similar to PPE. In eosinophilic folliculitis, patients present with chronic pruritic erythematous papules and pustules that are seen over the head, neck, proximal extremities and upper trunk with sparing of acral sites. The lesions typically waxes and wanes in severity and may spontaneously clear only to flare unpredictably [32]. In contradistinction, PPE affects the head, face, trunk, legs, arm, and acral sites (dorsum of hand and foot but sparing the sole and palm) without periods of improvement. Sometimes, eosinophilic folliculitis and PPE-HIV may look alike clinically making some investigators to suggest that PPE-HIV and eosinophilic folliculitis could be parts of the same disease spectrum [33]. Other skin conditions that can simulate PPE clinically include staphylococcal folliculitis, dermodex folliculitis, phototoxic/photo-allergic dermatitis, scabies, secondary syphylis, onchodermatitis and papulonecrotic tuberculid [11].
Histopathologic Features of PPE-HIV
Skin biopsy has been useful in distinguishing pruritic papular eruption of HIV from other potential causes of pruritus in HIV-infected patients. Histologic findings include: perivascular dermal lymphocytic inflammatory infiltrate with increased eosinophils and CD8+ lymphocytes [34]. There is also slight epidermal hyperplasia and focal area of epidermal spongiosis.
In 2003, a study of 102 HIV-positive patients indicated that a histology of arthropod bites was highly consistent with development of PPE papules. Specifically, most of the specimens revealed “superficial and deep, perivascular and interstitial infiltrates of lymphocytes and many eosinophils beneath an epidermis that was slightly hyperplastic, whereas others showed a focal areas of epidermal spongiosis surrounded by dermal infiltrates. The investigators surmised that the occurrence of PPE could represent an abnormal and exaggerated immune response to mosquito bites in individuals with low CD4 count [11]. Papular urticaria is a histologic differential diagnosis of pruritic papular eruption of HIV [35]. Papular urticaria is commonly seen in children as a result of hypersensitivity or id reaction to bites from insects [36]. In a prospective study of papular urticaria that evaluated the histopathologic features of 30 affected patients, more than 50% of patients had mild acanthosis, mild spongiosis, exocytosis of lymphocytes, mild subepidermal edema, extravasation of erythrocytes, superficial and deep mixed inflammatory cell infiltrate of moderate density, and interstitial eosinophils [35]. In patients with papular urticaria depending on the predominant cellular infiltrates 4 subtypes (Lymphocytic, eosinophilic, neutrophilic and mixed) may be recognized [35].
Ichihashi et al [37], studied the immune histochemistry of the papules of PPE and plaques of psoriasis. The study showed that in PPE, perivascular infiltrated cells in the dermis were mostly lymphocytes; while another study found a non specific inflammatory reaction in papules of PPE on histology [10]. A clinicopathologic study of pruritic papular eruption of HIV in 1991 found on histology the presence of superficial and mid-dermal perivascular and perifollicular mononuclear cell infiltrate with numerous eosinophils [20].
Because of the difficulty in differentiating PPE and eosinophilic folliculitis clinically, histology has become an important tool in differentiating the two. In eosinophilic folliculitis there is perifollicular infiltrates of eosinophils while in PPE there is a perivascular lymphocyte infiltrates with eosinophils. Recently in 2012, Afonso et al [33] studied the association between pruritic papular eruption and eosinophilic folliculitis and HIV infection in Brazil, and postulated that eosinophilic folliculitis is characterized by a folliculocentric collection of eosinophils with some overlap of these features with PPE and suggested that the two condition could be part of the same disease spectrum.
Treatment of Pruritic Papular Eruption of HIV
Pruritic papular eruption of HIV has often been observed to be resistant to treatment. However, there are a number of different treatment approach that have been shown to be effective in some patient. Topical potent corticosteroid, emollients and oral antihistamines should be the first line approach because of their availability and effectiveness in relieving itching. Moreover, it has been documented that antihistamine is superior to topical steroid in relieving itching [38]. Also, phototherapy either ultraviolet B light (UVB) or psoralens plus ultraviolet A light (PUVA) has been shown to be effective. Ultraviolet B (UVB) light therapy given three times weekly has been shown to reduce itching and improve cosmetic appearance [39]. Although concerns have been expressed regarding the ability of UVB radiation to potentially activate HIV gene expression, however there is no significant changes in HIV RNA levels, CD4 lymphocyte count or presence of opportunistic infections seen in patients receiving UVB light therapy [40]. Another reported useful agent is pentoxifylline. This is thought to work by its TNFα inhibitory effect. Pentoxifylline, dosed at 400mg three times daily, improved pruritus in an 8-weeks trial of patients with PPE [41]. But the efficacy and safety of pentoxifylline in PPE has not been studied in a randomized controlled trial.
Whether HAART makes a difference in treatment of patients with PPE-HIV is debated and the response is variable, but some researchers have shown consistent responses of PPE to HAART hence a recommendation that PPE should be used as a criteria for initiating HAART [23,27]. Because of the association of PPE-HIV with exaggerated immune response to arthropod bites, bed nets and insecticides may play an important role in its management.
CONCLUSION
Pruritic papular eruption of HIV is a frequent cause of substantial morbidity in HIV patients. In some regions, particularly in the sub-Saharan Africa, PPE-HIV is often the presenting symptom of HIV infected patient and therefore may play a role in diagnosis of HIV, especially when serologic testing is not available or affordable [10].
Consent
The examination of the patient was conducted according to the Declaration of Helsinki principles.
REFERENCES
1. Gelfand JM, Rudikoff D. Evaluation and treatment of itching in HIV infected patients. M Sinai J Med. 2001;68:298-308.
2. Smith KJ, Skelton HG, Yeager J, Lee RB, Wagner KF. Pruritus in HIV-1 disease:Therapy with drugs which may modulate the pattern of immune dysregulation. Dermatology. 1997;195:353-8.
3. James WD, Redfield RR, Lupton GP. A papular eruption associated with human T cell lymphotropic virus type III disease. J Am Acad Dermatol. 1985;13:563-6.
4. Mahe A, Simon F, Coulibaly S. Predictive value of seborrheic dermatitis and other common dermatosis for HIV infection in Bamako, Mali. J Am Acad Dermatol. 1996;34:1084-6.
5. Pallangyo KJ. Cutaneous findings associated with HIV disease including AIDS:experience from sub Saharan African. Trop Doct. 1992;22:35-41.
6. Olumide YM, Dada AJ, Sogbanmu IB, Ariuna GA. Seroprevalence study of HIV-1, HIV-II and HTLV-I among patients at the Dermato-venerology clinic of the Lagos University Teaching Hospital. Int J Dermatol. 1997;36:741-4.
7. Pitche P, Tchangai-Wallak, Napo-Koura G. Prevalence of skin manifestations in AIDS patients in the Lome-Tokoin University Hospital(Togo). Sante. 1995;5:349-52.
8. Liautaud B, Pape JW, DeHovitz JA, Thomas F, LaRoche AC, Verdier RI, et al. Pruritic skin lesions:A common initial presentation of acquired immunodeficiency syndrome. Arch Dermatol. 1989;125:629-32.
9. Hira SK, Wadhawan D, Kamanga J, Kavindel D, Macuacua R, Patil PS, et al. Cutaneous manifestations of human immunodeficiency virus in Lusaka, Zambia. J Am Acad Dermatol. 1988;19:451-7.
10. Colebunders R, Mann JM, Francis H, Bila K, Izaley L, Kakonde N, et al. Generalized pruritic papular eruption in African patients with HIV infection. AIDS. 1987;1:117-21.
11. Resneck JS Jr, Van Beek M, Furmanski L, Oyugi J, LeBoit PE, Kambugu F, et al. Etiology of pruritic papular eruptions with HIV in Uganda. JAMA. 2004;292:2614-21.
12. Guidelines for HIV care and treatment in infants and children. IAP and NACO with support from Clinton foundation UNICEF, WHO. 2006. Nov.
13. Lakshmi SJ, Rao GR, Ramalakshmi, Satyasree, Rao KA, Prasad PG, et al. Pruritic papular eruptions of HIV:a clinicopathologic and therapeutic study. Indian J Dermatol Venereol Leprol. 2008;74:501-3.
14. Bason MM, Berger TG, Nesbitt LT Jr. Pruritic papular eruption of HIV-disease. Int J Dermatol. 1993;32:784-9.
15. Goldsteins B, Berman B, Sukenik E, Frankel SJ. Correlation of skin disorder with CD4 Lymphocyte count in patients with HIV/AIDS. J Am Acad Dermatol. 1997;36:262-4.
16. Sivayathorn A, Srihra B, Lasanguankul W. Prevalence of skin disease in patients infected with human immune deficiency virus Bangkok, Thailand:Ann Acad Med Singapore. 1995;24:528-33.
17. Wiwanitkit V. Prevalence of dermatological disorder in Thai HIV-infected patients correlated with different CD4 lymphocyte count status:a note on 120 cases. Int J Dermatol. 2004;43:265-8.
18. Mawenzi LR, Oguttu RO, Williams CH, Joash A. Epidemiology and clinical spectrum of cutaneous diseases manifesting among newly diagnosed HIV seropositive adults in Nakuru County-kenya. Continental J Med Res. 2013;7:1-9.
19. Ukonu AB, Eze EU. Pattern of skin diseases at university of Benin Teaching Hospital, Benin City, Edo state, South-South Nigeria:a 12 month prospective study. Glob J Health Sci. 2012;4:148-57.
20. Hevia O, Jimenez-Acosta F, Ceballos PI, Gould EW, Pennys NS. Pruritic papular eruption of the acquired immunodeficiency syndrome:a clinicopathologic study. J Am Acad Dermatol. 1991;24:231-5.
21. Lowe S, Ferrand RA, Morris-Jones R, Salisbury J, Mongeya N, Dimairo M, et al. Skin Disease Among Human Immunodeficiency virus-infected Adolescents in Zimbabwe:A strong indicator of underlying HIV infection. Pediatr Infect Dis J 2010;29:346-51.
22. Akinboro AO, Onayemi O, Mejiuni AD. Frequency, pattern and extent of skin disease in relation to CD4 cell Counts among adults with HIV infection or AIDS in Osogbo, southwestern Nigeria. Int J Dermatol. 2014;53:416-24.
23. Eismans S. Pruritic papular eruption in HIV. Dermatol Clin. 2006;24:449-57.
24. Farsani TT, Kore S, Nadole P, Ramam M, Thiemans S, Leslie K, et al. Etiology and risk factors associated with a pruritic papular eruption in people living with HIV in India. J Int AIDS Soc. 2013;16:25-6.
25. Rosatelli JB, Roselino AM. Hyper-IgE, eosinophilia, and immediate cutaneous hypersensitivity to insect antigens in the pruritic papular eruption of human immunodeficiency virus. Arch Dermatol. 2001;137:672-673.
26. Aires JM, Rosatelli JB, Figueiredo JF, Roselino AM. Cytokines in the pruritic papular eruption of HIV. Int J Dermatol. 2000;39:903-6.
27. Castelnuovo B, Byakwaga H, Menten J. Can response of a pruritic papular eruption to antiretroviral therapy be used as a clinical parameter to monitor virological outcome?. AIDS. 2008;22:269-73.
28. Colebunders R, Moses KR, Laurence J. A new model to monitor the virological efficacy of antiretroviral treatment in resource-poor countries. Lancet Infect Dis. 2006;6:53-9.
29. Labhardt ND, Lejone T, Setoko M. A clinical prediction score in addition to WHO criteria for antiretroviral treatment failure in resource-limited settings experience from Lesotho. PLOS One. 2012;7:e47937.
30. Boonchai W, Laohasrisakul R, Manonukul J, Kalthanan K. Pruritic papular eruption in HIV seropositive patients:a cutaneous marker for immune suppression. Int J Dermatol. 1999;38:348-50.
31. Nnoruka NE, Chukwuka CJ, Anisuiba B. Correlation of mucocutaneous manifestations of HIV/AIDS infection with CD4 Counts and disease progression. Int J Dermatol. 2007;46:14-8.
32. Fearfield LA, Rowe A, Francis N, Bunker CB, Staughton RC. Itchy folliculitis and human immunodeficiency virus infection:Clinicopathological and immunological features, pathogenesis and treatment. Br J Dermatol. 1999;141:3-11.
33. Alfonso JP, Tomimori J, Michalamy NS, Nonogaki S, Porro AM. Pruritic papular eruption and eosinophilic folliculitis associated with human immunodeficiency virus(HIV) infection:a histopathological and immunohistochemical comparative study. J Am Acad Dermatol. 2013;67:269-75.
34. Ramo H, Pagliaric C, Takakura CF, Sotto MN, Duarte MI. Pruritic papular eruptions associated with HIV-etiopathogenesis evaluated by clinical, immunohistochemical and ultrastructural analysis. J Dermatol. 2005;32:549-56.
35. Jordaan HF, Schneider JW. Papular urticaria:a histopathologic study of 30 patients. Am J Dermatopathol. 1997;19:119-26.
36. Lewis-Jones MS. Papular Urticaria caused by Dermestes maculatus Degeer. Clin Exp Dermatol. 1985;10:181.
37. Ichihashi N, Seishima M, Takahashi T, Muto Y, Kitajima T. A case of AIDS manifesting Pruritic papular eruptions and Psoriasiform Lesions, an immunehistochemical study of the lesional dermal infiltrates. J Dermatol. 1995;22:428-33.
38. Navarini AA, Stoeckle M, Navarini S. Antihistamines are superior to topical steroids in managing human immunodeficiency virus (HIV)-associated popular pruritic eruption. Int J Dermatol. 2010;49:83-6.
39. Pardo RJ, Bogaert MA, Penneys NS, Byrne GE Jr, Ruiz P. UVB Phototherapy of the pruritic papular eruption of the acquired immunodeficiency syndrome. J Am Acad Dermatol. 1992;26:423-8.
40. Meola T, Soter NA, Ostreichner R, Sanchez m, Moy JA. The safety of UVB phototherapy in patients with HIV infection. J AM Acad Dermatol. 1993;29:216-20.
41. Bermann B, Flores F, Burke G 3rd. Efficacy of Pentoxifylline in the treatment of pruritic papular eruption of HIV-infected person. J Am Acad Dermatol. 1998;38:955-9.
Notes
Source of Support: Nil
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
|





Comments are closed.