|
Get Citation
|
|
|
Bazouti S, Omahsan L, Dikhaye S, Zizi N. Lipschütz ulcer: a rare diagnosis to keep in mind. Our Dermatol Online. 2018;9(3):294-295. |
|
|
Download citation file:
|
Lipschütz ulcer: a rare diagnosis to keep in mind
Sabah Bazouti1, Loubab Omahsan1, Siham Dikhaye1,2, Nada Zizi1,2
1Department of Dermatology, Mohammed VI University Hospital of Oujda, Medical School of Oujda, Mohammed First University of Oujda, Oujda, Morocco, 2Epidemiology Laboratory of Research and Public Health, Oujda, Morocco
Corresponding author: Dr. Sabah Bazouti, E-mail: Sabah.bazouti@gmail.com
DOI:10.7241/ourd.20183.16
Submission: 31.10.2017; Acceptance: 10.12.2017
ABSTRACT
Lipschütz ulcer (LU) is a rare condition that usually affects prepubertal and pubertal girls. It can be misdiagnosed as a sexually transmitted disease or even as a sign of child abuse, causing great anxiety to patients and their families. We describe a case of 15-year-old girl who developed a painful genital ulcer that healed spontaneously within 3 weeks. The pathophysiology remains unknown. However, there is some evidence of a possible link with several non-veterinary infections, including mainly acute Epstein-Barr virus infection. Differential diagnosis should be made with other sexually transmitted diseases, Behçet’s disease and Crohn’s disease. This rarely benign but disabling entity should be known by dermatologist and gynecologist to avoid unreasonable treatment and reassure patients and family about sexual transmission.
Key words: Genital ulcer, Lipschütz´s ulcer, Epstein–Barr virus
INTRODUCTION
Acute genital ulcer or Lipschütz ulcer is a rare and little known entity. It is characterized by the sudden onset of genital ulceration, of non-venereal origin, affecting mainly girls and adolescents before the start of their sexual activity. We report a typical case of a girl of 15 years old who has evolved well under symptomatic treatment.
CASE REPORT
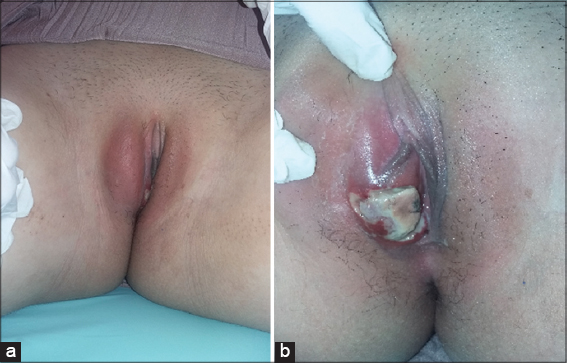
Miss O. H. is a 15-year-old girl who never had sexual relationships, and said she was a virgin. She was admitted with an extremely painful and debilitating vulvar ulcer, which had appeared suddenly five days earlier, preceded by fever, chills and odynophagia. The patient had no particular medical history, particularly no recurrent oral or genital aphthaosis and was not receiving any treatment. Examination of the vulvar mucosa found significant edema of the large right lip (Fig. 1a), with a large ulceration of 3 cm. This ulceration was hollow, necrotic, fibrinous, purulent, non-indurated, and surrounded by an inflammatory halo (Fig. 1b). The examination of other organs had revealed pharyngitis as well as small bilateral infra-centimetric inguinal lymphadenopathies. Syphilis, hepatitis, EBV, HIV1 and HIV2, as well as p24 antigenemia were negative. The biopsy showed a polymorphic inflammatory infiltrate rich in neutrophils associated with macrophages, small lymphocytes and a few rare plasma cells. Analgesic treatment as well as local treatment and antibiotic therapy based on amoxicillin-clavulanic acid were administered. The evolution was quickly favorable. The lesion healed in 20 days without any sequelae (Fig. 2), making it possible to retain the diagnosis of acute Lipschütz ulcer.
DISCUSSION
Acute ulcer of the vulva is a rare entity, initially described by Lipschütz in 1913 [1]. It usually reaches young virgin girls even before the beginning of their sexual life [2] as was the case in our observation. The etiology is most often unknown, but it is most often a contemporary episode of an infection. Primary EBV infection is most often reported, but this is not systematic [3].
Clinically, it takes the aspect of a deep, hyperalgic and often unique acute vulvar ulceration, usually preceded by a flu-like syndrome in 70% of cases [4] as in our patient. The histological aspect is not specific [5,6]. The diagnosis of Lipschütz ulcer remains a diagnosis of elimination often carried retrospectively, in front of a spontaneously and rapidly resolving evolution without subsequent recurrences. However, it is imperative to rule out other causes of more frequent genital ulcers, particularly a sexually transmitted disease, and to discuss the main differential diagnoses such as Behçet’s disease, idiopathic aphtosis or cutaneous localization of Crohn’s disease [2–6].
Therapeutic management is symptomatic and does not require systematic hospitalization. It is based on local care, analgesics or sometimes a short general corticosteroid therapy. Healing occurs within two weeks without a scar [7].
CONCLUSION
Lipschütz’s vulvar ulcer is a rare and very impressive clinical entity due to the deleterious, extremely painful and disabling ulcerations. Its diagnosis should not be ignored because of its benignity and its simple therapeutic management.
ACKNOWLEDGEMENT
Dr. Ilyas Charif for his English translation of the article.
CONSENT
The examination of the patient was conducted according to the Declaration of Helsinki principles.
REFERENCES
1. Lipschutz B. Uber eine eigenartige Geschwursform des weiblichen Genitales (Ulcus vulvae acutum). Arch Dermatol Syph. 1913;114:363-95.
2. Baron M, Mauger-Tinlot F, Resch B, Joly P, Marpeau L. Acute vulval ulcer or Lipschutz’s disease. J Gynecol Obstet Biol Reprod (Paris). 2002;31:684-6.
3. Sardy M, Wollenberg A, Niedermeier A, Flaig MJ. Genital ulcers associated with Epstein–Barr virus infection (ulcus vulvae acutum). Acta Derm Venereol. 2011;91:55-9.
4. Huppert JS. Lipschutz ulcers:evaluation and management of acute genital ulcers in women. Dermatol Ther. 2010;23:533-40.
5. Brinca A, Canelas MM, Carvalho MJ, Vieira R, Figueiredo A. Lipschütz ulcer (ulcus vulvae acutum):a rare cause of genital lesion. An Bras Dermatol. 2012;87:622-4.
6. Kluger N, Garcia C, Guillot B. Lipschütz acute genital ulcer. J Gynecol Obstet Biol Reprod (Paris). 2009;38:528-30.
7. Vera Mourinha, Sara Costa, Cecília Urzal, Fernando Guerreiro. Lipschütz ulcers:uncommon diagnosis of vulvar ulcerations. BMJ Case Rep. 2016 Feb 15;2016. pii:bcr2015214338.
Notes
Source of Support: Nil
Conflict of Interest: None declared.

Comments are closed.