|
Get Citation
|
|
|
Sharma A, Mahajan VK. Infantile perianal (perineal) pyramidal protrusion. Our Dermatol Online. 2018;9(2):217 |
|
|
Download citation file:
|
Infantile perianal (perineal) pyramidal protrusion
Aditi Sharma, Vikram K Mahajan
Department of Dermatology, Venereology & Leprosy, Dr. R. P. Govt. Medical College, Kangra (Tanda)-176001 (Himachal Pradesh) India
Corresponding author: Dr. Vikram K Mahajan, E-mail: vkm1@rediffmail.com
Submission: 31.08.2017; Acceptance: 06.11.2017
DOI: 10.7241/ourd.20182.30
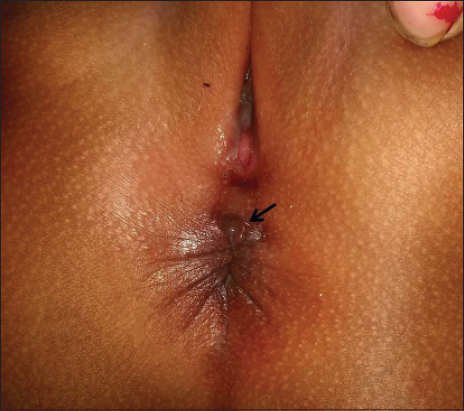
A 4-month-old infant was referred from surgery clinic for evaluation of perianal warts noticed recently by her mother. Her medical history was unremarkable and there was no suggestion of constipation, diarrhea, sexual abuse or maternal anogenital warts. Examination showed a solitary, small, fleshy, smooth surfaced, painless protrusion in the midline at superior aspect of anal verge (Fig. 1). No bleeding, excoriations, anal fissure, hemorrhoids or rectal prolapsed was noted. With a diagnosis of infantile perianal pyramidal protrusion the parents were counseled about its benign nature.
Infantile perianal (perineal) pyramidal protrusion (IPPP), a relatively newly described entity, is reported primarily in female infants. Its exact pathogenesis remains unknown but is considered as (i) embryologic remnant of urogenital septum or a congenital anatomical weakness of median raphe, (ii) functional or acquired secondary to mechanical irritation from wiping, constipation/diarrhea, or fistulas/anal fissures, and (iii) lichen sclerosus et atrophicus (LSA)-associated that results from post inflammatory rearrangement of fibrous tissue [1,2]. Resolution is spontaneous especially in functional variety once the primary trigger is removed [3,4]. Topical corticosteroid may help early resolution of LSA-associated IPPP [5]. The histologic features of PPP are not defined but will exclude other simulators [4]. Nevertheless, it is imperative to differentiate the condition from simulating lesions affecting perineum/perianum such as hemorrhoids, prianal warts, condyloma, mollascum contagiosum, sentinel tag, granulomatous lesions of Crohn’s disease, perineal midline malformation, rectal prolapse, infantile hemangioma and most importantly from signs of sexual abuse to avoid unnecessary treatment and parental anxiety.
REFERENCES
1. Patrizi A, Raone B, Neri I, D’Antuono A. Infantile perianal protrusion:13 new cases. Pediatr Dermatol. 2002;19:15-8.
2. Leung AK. Concomitant anterior and posterior infantile perianal protrusions. J Natl Med Assoc. 2010;102:135-6.
3. Cruces ML, De La Torre C, Losada A, Ocampo C, García-Doval I. Infantile pyramidal protrusion as a manifestation of lichen sclerosus et atrophicus. Arch Dermatol 1998;134:1118-20.
4. Zavras N, Christianakis E, Tsamoudaki S, Velaoras K. Infantile perianal pyramidal protrusion:a report of 8 new cases and review of the literature. Case Rep Dermatol. 2012;4:202-6.
5. Kim BJ, Woo SM, Li K, Lee DH, Cho S. Infantile perianal pyramidal protrusion treated by topical steroid application. J Eur Acad Dermatol Venereol. 2007;21:263-4.
Comments are closed.