Scalp skin primary cutaneous follicle center lymphoma – Case report
Agnieszka Giza1, Tomasz Stramek1, Andrzej Jaworek2, Grzegorz Dyduch3, Wojciech Jurczak1, Aleksander Skotnicki1
1Department of Heamatology, Jagiellonian University College of Medicine, Krakow, Poland, 2Department of Dermatology, Jagiellonian University College of Medicine, Krakow, Poland, 3Department of Pathomorphology, Jagiellonian University College of Medicine, Krakow, Poland
ABSTRACT
Primary cutaneous follicle center lymphoma is an Indolent Cutaneous B-cell Lymphoma responsible for almost 11% of primary cutaneous hematopoietic skin neoplasm. Although PCFCL has excellent prognosis of more than 95% 5 year survival rate it might be a challenge for a clinician because of diagnostic difficulties and a need to proceed complete differential diagnosis with systemic follicle center lymphoma. We present a case of a 55-year-old male patient with small, bug bite alike, erythematous, gradually extending lesion on the parietal area of the head. There were no other sign of disease on the skin and no other sides spreading of disease which was confirmed in CT imaging and no other systemic symptoms. After the diagnosis was made course of radical skin lesions 30 Gy radiotherapy were administered. In the follow-up examination skin lesion resolved completely and patient achieved complete remission of the disease.
Key words: PCFCL; Skin scalp; Lymphoma; Non-Hodgkin; Primary cutaneous follicle center lymphoma
INTRODUCTION
Primary cutaneous follicle center lymphoma is defined as the neoplastic proliferation of follicle center cells affecting the skin. It is classified as Indolent Cutaneous B-cell Lymphoma and is the most common primary B-cell lymphoma of the skin representing almost 11% of cutaneous lymphomas. There are three different growth patterns of the PCFCL: follicular, a follicular and diffuse, or a diffuse type. Neither of them is characterized by a worse or better prognosis [1,2].
Indolent cutaneous B-cell lymphomas have an excellent prognosis and 5- year survival rate for cutaneous follicle center lymphoma is more than 95%. Local recurrences are observed in about 20 % of the patients but extracutaneous involvement is rare. Complete staging investigations are necessary to distinguish between primary cutaneous follicle center lymphoma and the secondary skin involvement by systemic follicle center lymphoma because clinicopathologic features are extremely alike [1,2]. Staging procedures comprise CT scan of the whole body and bone marrow biopsy.
Local radiotherapy is preferred treatment method in PCFCL. Anthracycline-based chemotherapy might be considered in patients with widespread cutaneous disease and in cases of extracutaneous involvement [3]. Systemic or local ant-CD20 antibody administration is alternative treatment method report in some recent papers. It might be useful for advanced disease with generalized lesions as well [4].
CASE REPORT
A 55-year-old male patient presented to the Department of Dermatology of the University Hospital in Krakow in February 2015 with small, bug bite alike, erythematous, gradually extending lesion on the parietal area of the head. The lesion was asymptomatic. No pruritus or pain was reported. Since then patient was treated with topical steroids (Elitasone) without any improvement. Skin biopsy were performed in June 2015 and revealed small lymphocyte infiltration of the dermis (CD3/CD20=2/3). Expression of CD20 was positive, CD10 negative and there was faint expression of bcl-2. In two separate FR1-JH and FR2-JH amplifications reveal monoclonal proliferation of B-cells. Staging procedures were performed and patient was refered to the Department of Hematology of the University Hospital in Krakow.
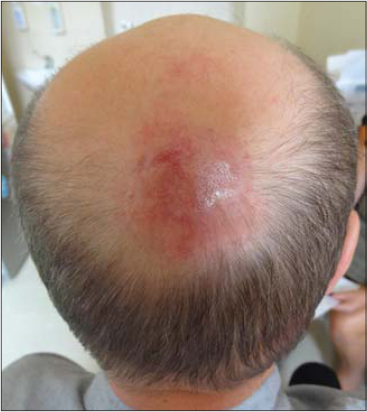
Physical examination at the admission to Outpatient Clinic of the Department of Hematology revealed 2 localized erythematous tumors on the parietal area of the scalp, 4 cm and 1,5 cm in diameter (Fig. 1). There were no other alteration on the skin and no other symptoms like fever, night sweats, weight lost, skin pruritus or malaise. Physical examination didn’t reveal lymph node enlargement and hepatosplenomegaly. The CT scans of chest, abdomen and pelvis did not show any abnormalities. USG of the neck revealed multiple lymph nodes of regular structure as in reactive lymph nodes. The laboratory tests such us CBC, LDH and beta 2 microglobulin level, liver and kidney were performed repeatedly and did not show any alterations beside slightly elevated monocyte count in CBC and CRP level. Result of a test for Borrelia Burgdorferi antibodies was negative.
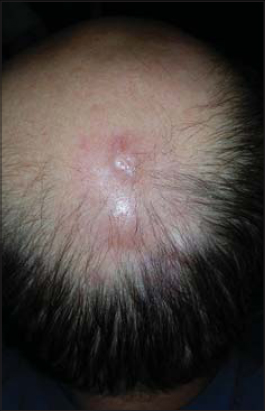
After fifth excisional biopsy the final diagnosis of the Primary Cutaneous Follicle Center Lymphoma was made. The patient was referred to Department of Radiotherapy and the course of radiotherapy from 15 to 20 December 2015 were administered. The dose of radical skin lesions 30 Gy radiotherapy was devided into 15 fractions of radiation. In the follow-up examination both skin lesions resolved completely and no other symptoms of the disease were noticed (Fig. 2). Next follow-up is planned for September 2016.
DISCUSSION
Primary cutaneous lymphoma are rare entity of all lymphomas with an estimated annual incidence of 1:100000 [5]. They are heterogenic and most, about 65%, derived from T lymphocytes and only 25% from B lymphocytes. Primary cutaneous follicle center lymphoma is the most common cutaneous B cell lymphoma and represent almost 11% of cutaneous lymphomas. In the previous classification was defined as a variant of follicular lymphoma, but since 2008 in classification WHO represent because of different clinical course new entity.
Primary cutaneous follicle center lymphoma presents clinically with characteristic erythematous solitary or grouped plaques, tumors or papules without ulceration. Lesions are preferentially located on the scalp, forehead or on the trunk [6]. Erythematous macules and papules may accompany central tumor or plaque and form a lesion called in the past “reticulohistiocytoma of the dorsum” or “Crosti’s lymphoma” [7]. These presentations of PCFCL form mainly diffuse pattern of growth and affect preferably the trunk. Typical follicle growth pattern primary cutaneous follicle center lymphomas have predilection for the head and neck [2]. Multifocal lesions might be observed but there is no association between the skin presentation and the course of the disease or prognosis [1]. Presentations of PCFCL may resemble non-malignant lesions of granulomatous rosacea, rhinophyma or even acne [8].
PCFCL may involve entire dermis and extend to the subcutaneous tissue. Lesions usually consists of small and large cleaved cells (centrocytes) and some number of non-cleaved cells (centroblasts). Small, reactive T-cells are mixed with the tumor tissue. The epidermis is not affected [9]. The follicles of the lymphoma have a reduced or absent mantle zone [10].
The usual immunophenotype of neoplastic cells include CD20+, CD79a+, bcl-6+. Diffuse type lesions may reveal CD10 expression dissimilarly to follicular growth type [11]. Expression of bcl-2 protein in primary cutaneous follicle center lymphomas is usually absent but there might be some faint bcl-2 staining in minority of follicular B-cells [12]. There are negative staining results for CD5, CD43 and MUM-1 [13].
Primary cutaneous follicle center lymphomas reveal a monoclonal rearrangement of the JH immunoglobulin gene and somatic hypermutation of variable heavy and light chain genes, which indicates their follicle center cell origin [1,14]. Interchromosomal t(14:18) translocation characteristic for systemic follicular lymphomas is extremely uncommon in PCFCL [2].
The main and most difficult issue is to make properly diagnosis quite often by some, repeated skin biopsies which should be examined in medical center with experienced histopathologist. In differential diagnosis should be considered diffuse large B cell lymphoma leg type and primary cutaneous marginal zone lymphoma. After evaluation of clinical stage and exclusion of secondary skin involvement by systemic follicle center lymphoma local, radical skin radiotherapy seem to be the best therapeutic option carries 95% of 5 years survival rate.
REFERENCES
1. Willemze R, Jaffe ES, Burg G, Cerroni L, Berti E, Swerdlow SH, WHO-EORTC classification for cutaneous lymphomasBlood 2005; 105: 3768-85.
2. Cerroni L, Gatter K, Kerl H, Skin Lymphoma: The Illustrated Guide 2011; 3rd Edition. Wiley-Blackwell, Oxford; 129-37.
3. Grange F, Bekkenk MW, Wechsler J, Meijer CJ, Cerroni L, Bernengo M, Prognostic factors in primary cutaneous large B-cell lymphomas: a European multicenter studyJ Clin Oncol 2001; 19: 3602-10.
4. Heinzerling LM, Urbanek M, Funk JO, Peker S, Bleck O, Neuber K, Reduction of tumor burden and stabilization of disease by systemic therapy with anti-CD20 antibody (rituximab) in patients with primary cutaneous B-cell lymphomaCancer 2000; 89: 1835-44.
5. Frank D. Groves, Martha S. Linet, Lois B. Travis, Susan S. Devesa, Cancer Surveillance Series: Non-Hodgkin’s Lymphoma Incidence by Histologic Subtype in the United States From 1978 Through 1995JNCI J Natl Cancer Inst 2000; 92: 1240-51.
6. Willemze R, Meijer CJ, Sentis HJ, Scheffer E, van Vloten WA, Toonstra J, Primary cutaneous large cell lymphomas of follicular center cell originJ Am Acad Dermatol 1987; 16: 518-26.
7. Berti E, Alessi E, Caputo R, Gianotti R, Delia D, Vezzoni P, Reticulohistiocytoma of the dorsumJ Am Acad Dermatol 1988; 19: 259-72.
8. Barzilai A, Feuerman H, Quaglino P, David M, Feinmesser M, Halpern M, Cutaneous B-Cell neoplasms mimicking granulomatous rosacea or rhinophymaArch Dermatol 2012; 148: 824-
9. Nathwani BN, Winberg CD, Diamond LW, Bearman RM, Kim H, Morphologic criteria for the differentiation of follicular lymphoma from florid reactive follicular hyperplasia: A study of 80 casesCancer 1981; 48: 1794-806.
10. Goodlad JR, Krajewski AS, Batstone PJ, McKay P, White JM, Benton EC, Primary cutaneous follicular lymphoma: a clinicopathologic and molecular study of 16 cases in support of a distinct entityAm J Surg Pathol 2002; 26: 733-41.
11. de Leval L, Harris NL, Longtine J, Ferry JA, Duncan LM, Cutaneous B-cell lymphomas of follicular and marginal zone types: use of Bcl-6, CD10, Bcl-2, and CD21 in differential diagnosis and classificationAm J Surg Pathol 2001; 25: 732-41.
12. Geelen FA, Vermeer MH, Meijer CJ, Van der Putte SC, Kerkhof E, Kluin PM, Bcl-2 expression in primary cutaneous large Bcell lymphoma is site-relatedJ Clin Oncol 1998; 16: 2080-5.
13. Hoefnagel JJ, Dijkman R, Basso K, Jansen PM, Hallermann C, Willemze R, Distinct types of primary cutaneous large B-cell lymphoma identified by gene expression profilingBlood 2005; 105: 3671-8.
14. Aarts WM, Willemze R, Bende RJ, Meijer CJLM, Pals ST, van Noessel CJ, VH gene analysis of primary cutaneous B-cell lymphomas: evidence for ongoing somatic hypermutation and isotype switchingBlood 1998; 92: 3857-64.
Notes
Source of Support: Nil
Conflict of Interest: None declared.


Comments are closed.