Facial nevus spilus mistakenly treated as melasma
Tasleem Arif, Syed Suhail Amin
Postgraduate, Department of Dermatology, STDs and Leprosy, Jawaharlal Nehru Medical/College(JNMC), Aligarh Muslim University (AMU), Aligarh, India.
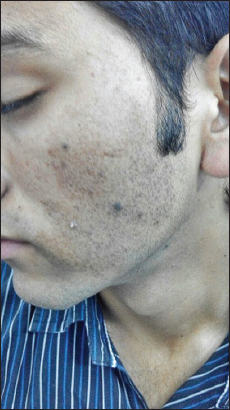
A 17 year old male visited our dermatology outpatient department (OPD) with brownish hyperpigmentation over left side of the face. The patient had visited some physicians in the past for this hyperpigmentation and had been applying several demelanizing creams but with poor response to the treatment. On further enquiry, he revealed that this pigmentation has been since his childhood. There is no history of intensification of this pigmentation during summers. On examination, there is a large macule around the size of 7cm×5cm, slightly brownish in color involving major portion of the left check and submandibular area with serrated borders on the superior and medial sides of the macule (Fig. 1a). On this light brownish macular background, there are present multiple 1-2 mm dark brownish macules along with some darker brownish papular lesions (nevi). There was no pigmentation on the right side of the face (Fig. 1b). With such a history and further supported by cutaneous examination, a diagnosis of unilateral facial nevus spilus was made.
Nevus spilus is also called as Speckled and lentiginous nevus. It is regarded as congenital melanocytic nevus. It remains usually lentiginous in early childhood and may develop palpable components at puberty in a ‘speckled’ distribution. It is composed of a flat, macular component which is slightly darker than the surrounding normal skin. There may be lentigo-like lesions or elevated darker-brown nevi interspersed within the slightly brownish macular background [1].
The present case was the nevus spilus which has been wrongly treated as melasma. Many general physicians treat any facial pigmentation as melasma with over the counter demelanizing creams especially steroid containing triple combinations. However, applying the basic principle of thorough history taking and cutaneous examination can avoid such mistakes.
CONSENT
The examination of the patient was conducted according to the Declaration of Helsinki principles. Written informed consent was obtained from the patient for publication of this article and any accompanying images.

Comments are closed.