Pseudoainhum associated with Psoriasis vulgaris
1Sudhaa Skin Centre, Jammu, India, 2Acharya Shri Chander College of Medical Sciences, Jammu, India
ABSTRACT
Pseudoainhum is the term applied to constricting bands around the digits or the limb which are either congenital or secondary to another disease. Progression of the constriction bands can lead to irreversible damage and autoamputation of the affected digit. Congenital pseudoainhum usually results due to amniotic bands or adhesions in utero while acquired pseudoainhum is usually secondary to trauma, neuropathy, systemic sclerosis or infections like leprosy. Psoriasis is a rare cause of acquired pseudoainhum with only five cases reported till date. We report a case of pseudoainhum secondary to psoriasis vulgaris in a 45 year old male which was successfully treated with topical corticosteroids and systemic methotrexate therapy.
Key words: Pseudoainhum; Psoriasis vulgaris; Autoamputation
INTRODUCTION
Pseudoainhum is the term applied to constricting bands around the digits or the limb which are either congenital or secondary to another disease. It is different from ainhum which is a specific type in which a painful constriction of the fifth toe occurs in adults, with eventual spontaneous amputation, usually seen in young African males. Acquired pseudoainhum is usually secondary to trauma, sensory neuropathy, systemic sclerosis or infections like leprosy [1]. Psoriasis is a rare cause of acquired pseudoainhum with only a few cases reported till date [2–6]. We report a case of pseudoainhum secondary to psoriasis vulgaris in a 45 year old male which was successfully treated with topical corticosteroids and systemic methotrexate therapy.
CASE REPORT
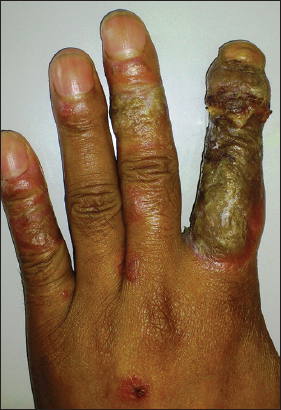
A 45 year old male presented with a three months history of development of generalized reddish scaly lesions which were associated with mild pruritus. After around four weeks, the patient started with pain and swelling of the left index finger which was associated with increased erythema and scaling of the pre-existing lesions. There was no previous history of trauma, fever, sore throat and pain in the left index finger and joints. There was also no past history of any medical illness, drug intake, personal and family history of any skin disorder. On examination, the patient had multiple well defined, erythematous, scaly plaques of psoriasis over the trunk and extensor aspects of elbows, knees and dorsum of hands. The left index finger showed the presence of a large erythematous scaly plaque and a well defined constriction band around the level of distal interphalangeal joint (Fig. 1). The nail of the left index finger was discolored with subungual hyperkeratosis and showed increased curvature while the other nails were normal. Investigations including a hemogram, liver and kidney function parameters and serum electrolytes were within normal limits. Chest X-ray, X-ray of hand and ultrasonography abdomen were normal. A skin biopsy was taken and histopathology was consistent with psoriasis.
The patient was started on emollients, clobetasol ointment 0.05% and 15mg/week methotrexate and there was marked improvement within three weeks of therapy with resolution of the constricting band and decreased erythema and scaling over the psoriasis plaques.
DISCUSSION
Pseudoainhum is a rare disease entity which, if left untreated, can lead to irreversible damage and autoamputation of the affected digit or limb. Congenital pseudoainhum usually results due to amniotic bands or adhesions in utero, although cases have been reported in Ehlers Danlos syndrome and after amniocentesis [1]. Histology of the band usually reveals broad, finger-like projections of collagen, and coarse elastic bundles which penetrate deep into the subcutaneous fat. Acquired pseudoainhum usually occurs as a result of infections like leprosy and tertiary syphilis, vascular abnormalities like Raynaud’s disease, trauma, cold injury, sensory neuropathy, syringomyelia, systemic sclerosis, etc. It may also occur in association with hereditary diseases such as palmoplantar keratodermas like Vohwinkel’s disease, pachyonychia congenita, erythropoietic protoporphyria and Olmsted’s syndrome. On histology, the bands in acquired pseudoainhum are more superficial and there may be histological features of associated disorders. Surgical management usually in the form of a staged Z-plasty is the preferred treatment modality while in late stages amputation may be required [1,7].
Psoriasis has been described as an uncommon cause of acquired pseudoainhum and till date only five cases of pseudoainhum secondary to psoriasis vulgaris have been reported in the literature. McLaurin [2] reported the acute onset of psoriasis and pseudoainhum development around the middle phalanx of a single digit in a 68 year old female while Kumar et al [3] reported acute onset of psoriasis and pseudoainhum development around multiple digits in an adult male. Almond et al [4] reported development of pseudoainhum around several digits developing over several months in the presence of long-standing psoriasis. All the three cases required surgical management of constriction bands. Ahn et al [5] reported the case of pseudoainhum with psoriasis in a five month old girl which was conservatively managed with topical pimecrolimus and low-dose narrowband UVB phototherapy. Anwar et al [6] have reported the development of pseudoainhum over a single digit in an elderly male which was successfully managed with oral acitretin and topical clobetasol propionate ointment.
The pseudoainhum in our patient occurred at the same time that he developed acute exacerbation of psoriasis but rapid initiation of topical and systemic therapy led to complete resolution of the constriction band without causing any irreversible damage. In conclusion, psoriasis is a common disorder which can rarely lead to development of pseudoainhum. It, therefore, becomes necessary to recognize the development and initiate management at the earliest to prevent the progression and autoamputation.
CONSENT
The examination of the patient was conducted according to the Declaration of Helsinki principles.
REFERENCES
1. Burrows NP, Lovell CR, Burns T, Breathnach S, Cox N, Griffiths C, Disorder of connective tissueRook’s Textbook of Dermatology 2010; 46: 8th ed. New Jersey: Blackwell Publishing; 69-70.
2. McLaurin CL, Psoriasis presenting with pseudoainhumJ Am Acad Dermatol 1982; 7: 130-2.
3. Kumar P, Gandhi V, Pseudoainhum in PsoriasisIndian J Dermatol 2012; 57: 238-9.
4. Almond SL, Curley RK, Feldberg L, Pseudoainhum in chronic psoriasisBr J Dermatol 2003; 149: 1064-6.
5. Ahn SJ, Oh SH, Chang SE, Choi JH, Koh JK, A case of infantile psoriasis with pseudoainhum successfully treated with topical pimecrolimus and low-dose narrowband UVB phototherapyJ Eur Acad Dermatol Venereol 2006; 20: 1332-4.
6. Anwar MI, Iftikhar N, Hasnain SH, Ishaq BM, Pseudoainhum in Acute PsoriasisJ Coll Physicians Surg Pak 2012; 22: 786-8.
7. Brodell RT, Helms SE, Wolff K, Goldsmith LA, Katz SI, Gilchrest BA, Paller AS, Leffell DJ, Constricting band (Ainhum and Pseudoainhum)Fitzpatrick’s Dermatology in General Medicine 2008; 7th ed. New York: Tata McGraw Hill Publishing; 562-3.
Notes
Source of Support: Nil
Conflict of Interest: None declared.
Comments are closed.