An interesting uncommon side effect of topical corticosteroids-hidradenitis suppurativa
Yugandar Inakanti1, Thimmasarthi Venkata Narsimha Rao2
1Department of Dermatology, Venerology and Leprosy, P.E.S. Medical College, Kuppam, India, 2Department of Dermatology, Venerology and Leprosy, Guntur Medical College, Guntur, India
ABSTRACT
There are many local and systemic side-effects of topical corticosteroids. To the best of our Knowledge, Hidradenitis Supportive (HS) due to topical corticosteroids has not been reported previously. We report a 39-year old, male patient who started himself a topical corticosteroid Pander Plus cream because of itching, scaly lesions over groins and buttocks since 6 months. After 4 months of topical treatment, he developed pus discharging sinuses over both groins and buttocks. Based on patient history, clinical and laboratory findings and the exclusion of other diagnoses, HS points out the use of topical corticosteroids. The case well highlights this unusual condition and represents the first case reported in India to our best of the knowledge. Having performed thorough literature search I would like to discuss in this report the evidence for this relation and stress the importance of appropriate usage of topical corticosteroids.
Key words: Hidradenitis; pus; sinus discharge; skin atrophy; striae; topical steroid
INTRODUCTION
Topical corticosteroids have now been in use for treating skin disease for over half a century, since the introduction of compound F or hydrocortisone (cortisol) in 1952 [1]. Many local and systemic side effects have become more prevalent since the uncontrolled use of high potency topical corticosteroids. The most common local side effects are atrophy, acneiform eruptions, erythema, folliculitis, hyper pigmentation, hypertrichosis, hypo pigmentation, Purpura, Striae, susceptibility to infections and Telangiectasia [2]. Here in, we report a case of HS due to using a topical corticosteroid cream.
CASE REPORT
A 39 year-old male patient reported to our department with complaints of pus discharging sinuses over both groins and buttocks since 2 months duration, past history of uncontrolled use of topical corticosteroid cream for itching over groins and buttocks for a period of 4 months. It was prescribed by friend initially and he got it over the counter sale. According to his history he did not have any systemic disease. He had only itching scaly skin lesions over groins and buttocks. He used topical corticosteroid cream by himself uncontrollably for improvement of itching without consulting dermatologist. Recently he underwent surgical excision of abscess over buttocks in private hospital. Physical examination was normal. Laboratory investigations revealed leucocytosis raised ESR, normal Liver function tests and Kidney function tests.
On Local examination:
1. Longitudinal striae over supra pubic area and flanks, hypopigmentation over both groins (Fig. 1);
Figure 1: Multiple striae over anterior abdomen, flanks and thighs. shows multiple discharging sinuses over pubic area, few with crusting.
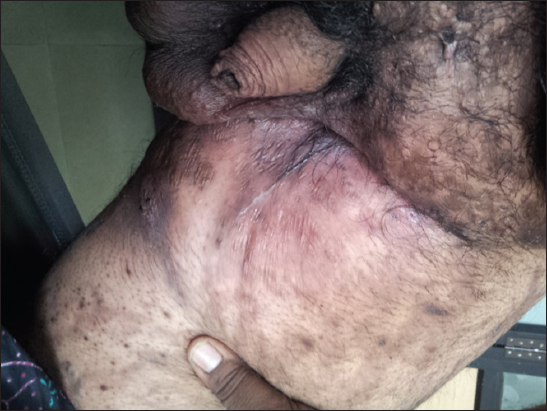
2. Skin atrophy over both groins and pubic area (Fig. 2);
Figure 2: Skin atrophy over both groins and pubic area.
3. Multiple discharging sinuses with healed scars over buttocks and hypertrichosis (Fig. 3);
Figure 3: Multiple discharging sinuses over inter gluteal region, scar and hypertrichosis.
4. Circular shaped crusted lesion over the left medial aspect of the thigh and multiple discharging sinuses over left groin with pus (Fig. 4).
Figure 4: Multiple discharging sinuses over left groin with pus.
Based on the patient’s history, clinical and laboratory findings and the exclusion of other diagnoses, the HS associated with the use of topical corticosteroids cream was diagnosed. Pus culture and sensitivity was done. In Gram stain of pus culture showed staphylococcus aureus and anaerobic streptococci. It showed Sensitivity to Vancomycin, Tecoplanin and Gatifloxacin.
DISCUSSION
Supportive hidradenitis is a chronic relapsing inflammatory disease originating in apocrine gland follicles, which may become chronic and often indolent due to subcutaneous extension with induration, scarring, destruction of skin appendages and sinus formation [3].
Comedonal occlusion of the “apocrine gland follicle” unit therefore obstructs the outflow of the apocrine gland in addition to that of the sebaceous gland, and is believed to be the initiating event in hidradenitis.
Friction and pressure accentuate the inflammatory changes that invade the fat and cause further granulomatous change extending widely over the buttocks and thighs. Persistent perineal sinuses are frequent, and deep lesions cause anal fistulae.
Keratin Plugs are identified in apocrine gland follicles, leukocyte inflammatory cells in ducts of glands. As the apocrine gland extends well below the dermis into the less supportive subcutaneous tissue, the suppuration readily breaks through the gland and extends under the skin.
Laboratory investigations show higher yield of potential pathogens Staphylococcus aureus, anaerobic streptococci and, notably, the microaerophilic organisms Streptococcus milleri from purulent disease and abscesses.
Topical corticosteroids are classified according to their potency into mild, moderate, potent, and very potent categories. It is recognized that topical corticosteroid preparations can be absorbed through the skin and may result in suppression of hypothalamo-pituitary-adrenal (HPA) axis and may cause Cushing’s syndrome. Prolonged steroid use is associated with myriad side effects. Androgen levels were on average increased compared with controls, but were normal in many individual patients. The application of topical corticosteroids on thin and damaged skin, on the elderly or paediatric population or under occlusion, intertriginous areas or moisture areas increases risk of side effects [4].
Corticosteroids can cause virilization in females and feminization in males. And also corticosteroids may increase muscle mass as well as hypertrophy of the penis, accentuate scrotal folds and stimulate sebaceous glands in men.
Corticosteroids once absorbed stimulate sebocyte proliferation [5] and aggravates sebaceous gland activity by its stimulatory effects on proliferation and differentiation in the presence of growth factors [6]. Friction and pressure accentuate the inflammatory changes that invade the fat and cause further granulomatous change extending widely over the buttocks and thighs.
Following atypical sites already noted in dermatological literature, areola, infra- mammary and inter-mammary fold, [7] abdomen, scalp, [8] external auditory meatus, ear lobes, retro auricular fold [9], abdomen and chest [10].
In our case report patient continually applied ointment, which combines a potent topical steroid and an antifungal agent, twice daily to the intergluteal folds, pubic area and both groins. The occlusive nature of this anatomical location had led to an increase in the potency of the steroid.
CONCLUSION
In conclusion, this is the first case of Hidradenitis Suppurativa due to topical corticosteroids. The clinicians should be aware of an unusual complication caused by topical corticosteroids.
ACKNOWLEDGEMENT
We gratefully acknowledge the help of the:
- Principal, PESIMSR, Kuppam.
- The professor and head of the department of DVL, PESIMSR, Kuppam.
REFERENCES
1. Mukhopadhyay AK, Baghel VA, study to evaluate the efficacy and safety of hydrocortisone aceponate 0.127% lipophilic cream in steroid responsive dermatoses in Indian patientsIndian J Dermatol Venereol Leprol 2010; 76: 591
2. Jones JB, Rooks Burns T, Breathnach S, Cox N, Griffiths C, Topical TherapyRooks textbook of Dermatology 2010; 3: 8th edition. Oxford: Blackwell; 73.16-22.
3. Hay RJ, Adriaans BM, Rooks Burns T, Breathnach S, Cox N, Griffiths C, Bacterial infectionsRooks textbook of Dermatology 2010; 3: 8th edition. 30Oxford: Blackwell; 79-81.
4. Pappas A, The relationship of diet and acne: A reviewDermatoendocrinol 2009; 1: 262-7.
5. Feingold KR, Elias PM, Endocrine-skin interactions. Cutaneous manifestations of adrenal disease, pheochromocytomas, carcinoid syndrome, sex hormone excess and deficiency, polyglandular autoimmune syndromes, multiple endocrine neoplasia syndromes, and other miscellaneous disordersJ Am Acad Dermatol 1988; 19: 1-20.
6. Slokinski A, Wortman J, Luger T, Paus R, Solomon S, Corticotrophin releasing hormone and propiomelanocortin involvement in the cutaneous response to stressPhysiol Rev 2000; 80: 979-1020.
7. Li EN, Mofid MM, Goldberg NH, Silverman RP, Surgical management of hidradenitis suppurativa of the nipple-areolar complexAnn Plast Surg 2004; 52: 220-3.
8. Jain S, Sardana K, Garg VK, Sinha S, Hidradenitis suppurativa involving the preauricular region: An unusual locationIndian J Dermatol Venereol Leprol 2012; 78: 229
9. Moul DK, Korman NJ, The cutting edge. Severe hidradenitis suppurativa treated with adalimumabArch Dermatol 2006; 142: 1110-2.
10. Poitrine FC, Revuz JE, Wolkenstein P, Viallette C, Gabison G, Pouget F, Clinical characteristics of a series of 302 French patients with hidradenitis suppurativa, with an analysis of factors associated with disease severityJ Am Acad Dermatol 2009; 61: 51-7.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.



Comments are closed.