Localised facial pityriasis versicolor-A very uncommon presentation of a common disease
Tasleem Arif
Postgraduate Department of Dermatology, STDs and Leprosy, Jawaharlal Nehru Medical College (JNMC), Aligarh Muslim University (AMU), Aligarh, India
Sir,
Pityriasis versicolor is a common superficial fungal infection of the skin which is caused by various species of yeast of the genus Malassezia and is clinically characterized by scaly hypo pigmented or hyper pigmented macules usually involving the upper trunk, upper arms, neck and abdomen [1]. Lesions of pityriasis versicolor confined to face has rarely been reported. In this article the author reports a 17 year old boy who had pityriasis versicolor localized to the face.
CASE REPORT
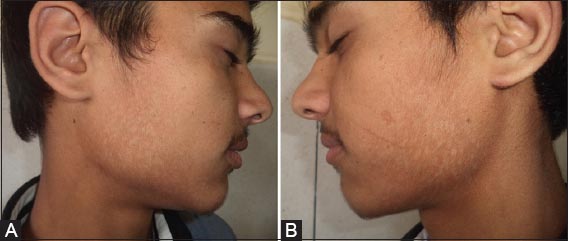
A 17 year old boy presented with three months history of multiple asymptomatic hypo pigmented macules over both cheeks. He denied any previous history of similar complaints. On examination, there were multiple discrete hypo pigmented macules with fine branny scaling present on both cheeks (Figs 1a, 1b). There were no such lesions on any other parts of the body. When the affected skin was stretched, the scaling of the lesions became prominent showing the positive Zireli’s sign. The examination of hair, nail and mucous membranes was normal. KOH examination of skin scrapings from the lesions showed multiple short hyphae and spores. Skin biopsy was not done. A diagnosis of localized facial pityriasis versicolor was made. He was treated with topical sertaconazole 2% cream applied twice daily. In addition, he was prescribed oral fluconazole 300 mg weekly for two weeks. The hypo pigmentation took about two months to recover.
DISCUSSION
Pityriasis versicolor mostly affects the upper trunk, but commonly the lesions spread to upper arms, neck and abdomen. Less commonly, it involves axillae, groins, thighs and genitalia. Lesions involving palms have been reported from the tropics but rarely described from temperate zones. Pityriasis versicolor involving face is well recognized in the tropical areas but lesions restricted to the face have rarely been reported [1].
Morphologically, various types of pityriasis versicolor have been reported. These include hypochromic (commonest), hyperchromic, combination of hypochromic and hyperchromic, erythematous, circinate, atrophying, acral, parasitic achromia, follicular, involving inguinocrural region and simulating erythrasma. A clinical variant resembling pityriasis rubra pilaris has been described [2,3]. Localized facial pityriasis is a rare presentation and hence reported. The scaling of macules of pityriasis versicolor can be made prominent by stretching the affected skin. This is called Zireli’s sign [4]. Various mechanisms have been proposed for hypopigmentation in pityriasis versicolor. Production of dicarboxylic acids like azaleic acid by Malassezia species causing a competitive inhibition of the enzyme tyrosinase and a probable cytotoxic effect on hyperactive melanocytes have been suggested by some researchers [5]. The importance of this clinical type lies in differentiating this entity from the lesions of pityriasis alba in children as both can present with hypopigmented scaly macules. However, type of scaling, Zireli’s sign, woods lamp examination and KOH examination of skin scrapings will differentiate between the two entities.
CONSENT
The examination of the patient was conducted according to the Declaration of Helsinki principles. Written informed consent was obtained from the patient for publication of this article and any accompanying images.
REFERENCES
1. Hay EJ, Ashbee HR, Burns T, Breathnach S, Cox N, Griffi ths C, MycologyRook’s Textbook of Dermatology 2010; 2: 8th edition. U.K: Wiley-Blackwell; 36.10-36.12.
2. Arif T, Rather S, Follicular pityriasis versicolor-Rare variant of a common dermatological diseaseOur Dermatol Online 2015; 6: 1-2.
3. Arif T, Acral pityriasis versicolor – A rare clinical presentationOur Dermatol Online 2015; Aprilissue 2in press
4. Framil VMS, Melhem MSC, Szeszs MW, Corneta EC, Zaitz C, Pityriasis versicolor circinata: isolation of Malassezia sympodialis Case reportAn. Bras. Dermatol 2010; 85: 227-8.
5. Nazzaro-Porro M, Passi S, Identification of tyrosinase inhibitors in cultures of PityrosporumJ Invest Dermatol 1978; 71: 389-402.
Notes
Source of Support: Nil
Conflict of Interest: None declared.
Comments are closed.