Exfoliative Cheilitis a male patient – a case report
Mohammad S. Nayaf
Dermatology, Department of Medicine, College of Medicine, University of Tikrit, Iraq
ABSTRACT
Introduction: Exfoliative cheilitis, one of a spectrum of diseases that affect the vermilion border of the lips, is uncommon and has no known cause. It is a chronic superficial inflammatory disorder of the vermilion borders of the lips characterized by persistent scaling; it can be a difficult condition to manage. The diagnosis is now restricted to those few patients whose lesions cannot be attributed to other causes, such as contact sensitization or light. Case Report: We present a 17 year-old male presented to the out clinic in Baghdad with the chief complaint of a persistent scaly on his lower lips. The patient reported that the skin over the lip thickened gradually over a 3 days period and subsequently became loose, causing discomfort. Once he peeled away the loosened layer, a new layer began to form again. Conclusion: The lack of specific treatment makes exfoliative cheilitis a chronic disease that radically affects a person’s life. The aim of this paper is to describe a case of recurrent exfoliative cheilitis successfully treated with intralesional corticosteroids and to present possible hypotheses as to the cause.
Key words: Exfoliative cheilitis; testosterone; sustanon; corticosteroid
INTRODUCTION
The definition of the vermilion as the transition area between the skin and the mucous membrane (semimucosa) was introduced for the first time by Jean Darier, a French dermatologist, in the 19th century [1].
The term cheilitis is understood as referring to an inflammatory process that affects the lips, either the cutaneous section or the contiguous semi-mucosal area called the vermilion (the lips in the common use of the term), and the mucosal section of the internal lip [2]. Cheilitis is classified into various types: angular cheilitis, actinic cheilitis, contact cheilitis, plasma cell cheilitis, cheilitis glandularis, cheilitis granulomatosa, exfoliative cheilitis and factitious chelitis. Lip lesions can be manifestations of systemic diseases, a localized expression of dermatologic diseases or a localized condition of the lips. In most cases, a good history, thorough clinical examination and relevant investigations will help the clinician arrive at a diagnosis [3].
Exfoliative Cheilitis (EC) is defined as a chronic inflammatory disorder of the vermillion border of the lips, which is characterized by the persistent formation of scales and crusts [4].
It is characterized by unremitting production and desquamation of thick scales of keratin. Crusts may be attributed to self induced trauma such as repetitive biting, picking or licking of the lips. Underlying stress or psychiatric conditions may cause or exacerbate exfoliative cheilitis which regress with psychotherapy and anxiolytic-antidepressant treatment. This condition is disabling as it causes cosmetic disfigurement and also affects daily activities such as chewing and speaking. The lack of specific treatment makes exfoliative cheilitis a chronic disease [5].
The recurrent exfoliation leaves a temporarily erythematous and tender surface. The lips are chronically inflamed and covered with crusts that from time to time tend to desquamate, leaving a glazed surface on which new crusts form. Fissures may be present, and there may be burning, tenderness, and some pain. The lower lip is more often involved, with the inflammation limited to the vermilion part [6].
Most cases occur in girls or young women, and the majorities have personality disorders [7].
Etiology and pathogenesis are unknown, although some cases may be factitious. Chronic lip biting, picking, sucking or unconscious licking of the lips may be the underlying mechanism for trauma and scaling [8].
CASE REPORT
A healthy 17-year-old man, unmarried, high school student of Arab descent complained of one year and six months history of chronic dry scaling lesion of the lower lip. The main chief was aesthetic compromising. The patient reported that the skin over the lip thickened gradually over a 3 days period and subsequently became loose, causing discomfort. Desquamation was followed immediately by the formation of new scales which became thick within days. Once he peeled away the loosened layer, a new layer began to form again.
Past medical history disclosed painful, right hemiscrotum in November 2012, and was referred to an endocrinologist after presenting to his general practitioner with diagnosis of male hypogonadism. He had no history of hypothalamic, pituitary, or testicular disorders. Physical examination was unremarkable. Biochemical investigations confirmed the presence of hypogonadism with slightly depressed testosterone levels, for which no cause (including Klinefelter syndrome) was identified.
He was then put by endocrinologist on injectable sustanon-250 mg, one injection every three weeks, in total two injections. In December he was also put on injectable sustanon-250 mg one injection every four weeks, in total four injections. Three months later, the patient returned to his general practitioner, complaining of cheilitis of the lower lip and exacerbation of preexisting acne vulgaris and he was referred to dermatologist.
Initially, there had been a tingling sensation but pain, ulceration, fissuring and bleeding were denied. He denied excessive licking or biting of the lips, and he denied skin, conjunctival and genital lesions and the patient could not identify a specific initiating cause. There was no history of any mucocutaneous problem. The family history for atopic diseases in the patient and his family was negative.
He had no symptoms of gastrointestinal disturbances or other relevant medical conditions. No member of his family had a similar condition and no use of new creams, toothpaste or cosmetic items around the lips before the problem began.
The results of a general examination revealed young man who weighed 70 kg. He had no fever and looked generally well. Examination of his head and neck revealed no palpable cervical lymph nodes. Intraoral examination showed good oral hygiene.
The patient had consulted several dental practitioners and dermatologists; Ketoconazole cream was prescribed for treatment of the fungal contaminant, but no change was noted, as was the application of Fucidin cream topically. The patient was prescribed mild topical corticosteroid this improved his condition somewhat, but did not resolve it completely. Our patient’s condition was also resistant to topical tacrolimus.
DERMATOLOGICAL CONDITION
Examination revealed small, thick, white-coloured scales of the vermilion zone at two sites one in the left and the other on the right of the middle site of the lower lip. The adjacent skin and labial mucosa were not affected. Lesions characteristic of acne vulgaris were visible on the skin of the chin, cheeks, forehead with papules, and comedones (Fig. 1).
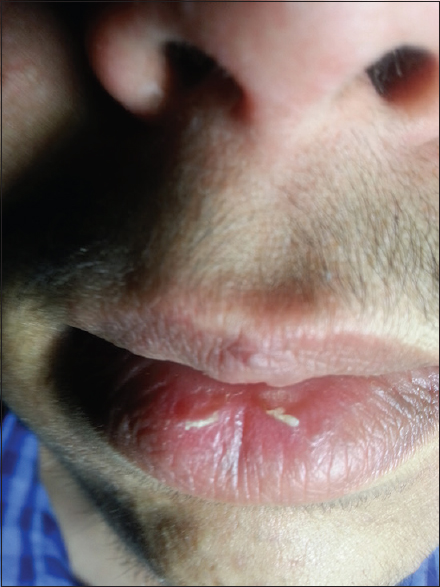
Figure 1: Scaling and crusting of lips including vermilion border
INVESTIGATION AND DIAGNOSIS
The results of a battery of tests, including complete blood work, general urine examination, liver function tests, a Mantoux test and chest radiograph showed no abnormalities. Vermilion swabbing for bacteriological examination was negative. Fungal culture for fungal examination was also negative. No antibodies against herpes simplex virus (anti-HSV1, HSV2 in the classes IgM and IgG) were found in blood serum. The concentration of vitamin B12, zinc was normal. FSH, LH, testosterone in blood serum was normal at the present time. Ultrasound examination of the abdominal cavity and scrotal ultrasound showed no deviations from the normal. Inflammatory bowel conditions were also ruled out after consultation with a gastroenterologist. Patient refused biopsy.
The overall findings suggested a diagnosis of exfoliative cheilitis. A diagnosis of exfoliative cheilitis was made based on the history and the clinical findings.
TREATMENT
Intralesional corticosteroid was successful treatment and he has not had a relapse in three months. No adverse effects from intralesional corticosteroids were noted in this patient (Fig. 2).
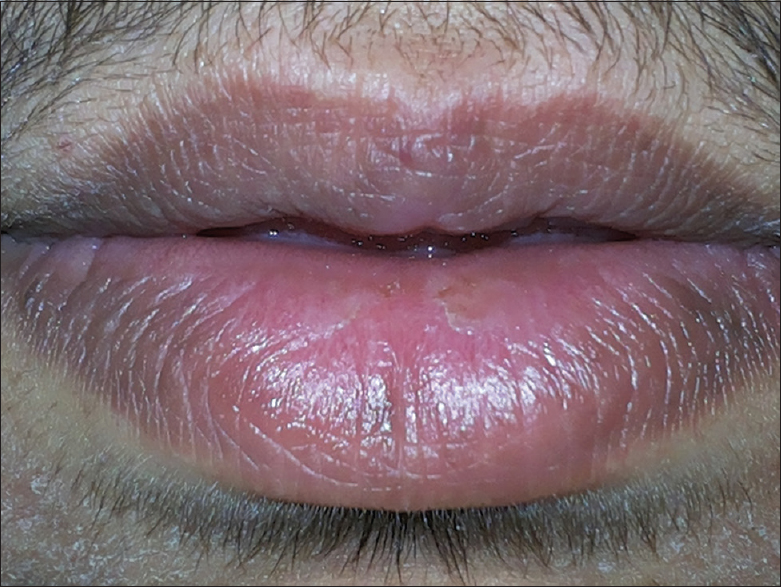
Figure 2 Marked improvement following intralesional corticosteroids.
DISCUSSION
Clinicians knowledge of the clinical course of this disease is important for accurate diagnosis. This report records in detail the clinical progress of the disease over a period of 3 days.
Daley and Gupta [9] and Brooke [10] reported a similar cyclical pattern of disease activity. Brooke mentioned a 5-day period for completion of the whole cycle. Our patient claimed that the hyperkeratotic plaque developed and became loose over a period of 3 days.
Our patient had no factitious activity. In fact, he took particular care to avoid pain and bleeding when moving his lips. However, the possibility of Munchausen’s syndrome cannot be ruled out in those cases in which the patient does not give any indication of factitious activity when questioned or observed [11].
Raede and others [12] discussed the possibility of cheilocandidosis. The authors achieved successful resolution of such lesions with antifungal therapy. However, for people who have no specific predisposing factors, such as our patient Candida could not be isolated from the lesion nor did the condition respond to antifungal therapy.
Oral sepsis has also been implicated as a cause of exfoliative cheilitis because it has resolved after implementation of good oral hygiene [13]. Our patient had very good oral hygiene.
Management of exfoliative cheilitis is difficult but it has responded to treatment with reassurance, topical steroids, psychotherapy and tranquillizers. Some cases can resolve spontaneously [14]. The few reported cases in literature describe therapeutics limitations of topic and systemic steroids, antibiotics, keratolytic agents, sunscreen and cryotherapy. Antifungal agents can be administered to patients in whom there is secondary fungal infection but it does not prevent the formation of keratin scales [15]. Medication with anti-depressants was helpful in the case of a 16-year-old male with persistent crusting of the lips with the diagnosis of exfoliative cheilitis [16]. Our patient’s condition was resistant to emollients, life-style changes, and different topical treatment as mentioned before; only intralesional corticosteroid has successfully cleared the lesions.
Although androgens have no direct anabolic effect on the epidermis, they may modulate keratinocyte maturation. Several authors reported increased speed of epidermis proliferation after testosterone treatments [17].
Transdermal testosterone-replacement therapy is associated with a variety of skin reactions, mainly erythema or pruritus, which are more common with patches than with gel preparations. Intramuscular injections of testosterone can cause local pain, soreness, bruising, erythema, swelling, nodules, or furuncles. [18]. Acne, oily skin, increased body hair, and flushing have also been observed [19].
It was also reported a case of hyperpigmentation and acanthosis nigricans in the same patient due to testosterone injections [20].
In our patient, the probable cause of the disease was due to testosterone injection. In our patient, significant improvement in scaling was seen with intralesional corticosteroids therapy without any recurrence till date.
CONCLUSION
Exfoliative cheilitis is a benign but often cosmetically unsightly condition. It predominantly affects both sexes under 30 years of age and typically follows a cyclical course. No appropriate treatment has been identified for this condition because the cause remains unclear; although some cases, such as our case, may be initiated by testosterone. This case highlights the fact that exfoliative cheilitis is may be secondary to drug such as testosterone injection and intralesional corticosteroids can be used as therapeutic option in such affected patients.
CONSENT
Written informed consent was obtained from the patient for publication of this case report and any accompanying images. The examination of patients is conducted according to the Declaration of Helsinki principles. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
REFERENCES
1. Rosińska-Więckowicz A, Misterska M, Bartoszak L, Żaba R, Cheilitis – case study and literature reviewPost Dermatol Alergol 2011; 3: 231-9.
2. Francalanci S, Sertoli A, Giorgini S, Pigatto P, Santucci B, Valsecchi R, Multicentre study of allergic contact cheilitis from toothpastesContact Dermatitis 2000; 43: 216-22.
3. Mani SA, Shareef BT, Exfoliative Cheilitis: Report of A CaseJCDA 2007; 73: 7.
4. Laskaris G, Color Atlas of Oral Diseases2003; New York: Gereg Thieme Verlag; Diseases of the Lips; Exfoliative Cheilitis; 132.
5. Gupta S, Pande S, Borkar M, Exfoliative cheilitis due to habitual lip biting and excellent response to methotrexatePJMS 2012; 2: 1.
6. James WD, Berger TG, Elston DM, Andrews’ Diseases of the Skin: Clinical Dermatology2011; Eleventh edition. Elsevier Saunders; 783.
7. Scully C, Hegarty A, Burns T, Breathnach S, Cox N, Griffiths C, The Oral Cavity and LipsRook’s Textbook Of Dermatology 2010; 4: Eighth edition. Wiley-Blackwell; 69-127.
8. Denardi Roveroni-Favaretto LH, Bortolin LK, Almeida JD, Topical Calendula officinalis L. successfully treated exfoliative cheilitis: a case reportBioMed Central 2009; 2: 907.
9. Daley TD, Gupta AK, Exfoliative cheilitisJ Oral Pathol Med 1995; 24: 177-9.
10. Brooke RI, Exfoliative cheilitisOral Surg Oral Med Oral Pathol 1978; 45: 52-5.
11. Michalowski R, Munchausen’s syndrome: a new variety of bleeding type self-inflicted cheilorrhagia and cheilitis glandularisDermatologica 1985; 170: 93-7.
12. Reade PC, Rich AM, Hay KD, Radden BG, Cheilo-candidosis – a possible clinical entity. Report of 5 casesBr Dent J 1982; 152: 305-8.
13. Brooke RI, Exfoliative cheilitisOral Surg Oral Med Oral Pathol 1978; 45: 52-5.
14. Connolly M, Kennedy C, Exfoliative cheilitis successfully treated with topical tacrolimus. British Association of DermatologistsBritish Journal of Dermatology 2004; 151: 232-257.
15. Reade PC, Sim R, Exfoliative cheilitis – a factitious disorder?Int J Oral Maxillofac Surg 1986; 15: 313-317.
16. Taniguchi S, Kono T, Exfoliative cheilitis: a case report and review of the literatureDermatology 1998; 196: 253-255.
17. Petroianu A, Veloso DFM, Alberti LR, Figueiredo JA, Carmo Rodrigues FHO, Carvalho E, Carneiro BGM, Hypoandrogenism related to early skin wound healing resistance in rats. Blackwell Verlag GmbHAndrologia 2010; 42: 117-20.
18. Bassil N, Alkaade S, Morley JE, The benefits and risks of testosterone replacement therapy: a review. DovepressTherapeutics and Clinical Risk Management 2009; 5: 427-448.
19. Rhoden EL, Morgentaler A, Risks of Testosterone-Replacement Therapy and Recommendations for Monitoring. The New England Journal of MedicineN Engl J Med 2004; 350: 482-92.
20. Karadag A, Kavala M, Demir F, Turkoglu Z, Kartal I, Zemheri E, A case of hyperpigmentation and acanthosis nigricans by testosterone injectionsHuman & Experimental Toxicology[Hum Exp Toxicol] 2014; 6: 11921-31.
Notes
Source of Support: Nil
Conflict of Interest: None declared.
Comments are closed.