Late onset ‘en coup de sabre’ following trauma: Rare presentation of a rare disease
Tasleem Arif1,2, Imran Majid3, Mir Laieq Ishtiyaq Haji2
ABSTRACT
En coup de sabre (linear scleroderma of face) is a rare type of morphea (localized scleroderma) involving fronto-parietal area of the forehead and scalp. Many triggering factors have been implicated in the development of morphea like trauma, immobilization, bacille Calmette–Guérin (BCG) vaccination, injections of vitamin K, mechanical compression from clothing, etc. Linear scleroderma primarily affects the pediatric population, with 67% of patients diagnosed before 18 years of age. In this article, we describe a case of 26 year old female who presented with a three months history of brownish indurated plaque of skin on the frontal and forehead regions of the head. The patient gave a history of trauma at the same site six years back. The diagnosis of morphea was made clinically supported by histopathological features of the skin biopsy. Her neurological examination was normal. ANA was negative. Brain MRI didn’t reveal any abnormality. She was treated with topical tacrolimus 0.1% ointment. The late onset en coup de sabre is a rare presentation and hence reported.
Key words: En coup de sabre; localized scleroderma; morphea; trauma
INTRODUCTION
Scleroderma is a connective tissue disorder of unknown etiology which is characterized by increased collagen production leading to the thickening and hardening of skin and other organs. It encompasses a spectrum ranging from localized scleroderma (LS) at one end to the systemic sclerosis (SSc) at the other extreme [1]. The localized form, also known as morphea, is characterized predominantly by the involvement of the skin; occasionally involving the underlying muscles with sparing of internal organs [2]. The exact cause of morphea is unknown, but several triggering factors have been mentioned in the literature which include trauma, immobilization, bacille Calmette–Guérin (BCG) vaccination, injections of vitamin K, mechanical compression from clothing, etc [3, 4]. Clinically, LS is subdivided into five types: plaque, linear, en coup de sabre, generalized and pansclerotic [5]. Linear scleroderma of en coup de sabre is a rare subset of LS. The typical presentation affects fronto-parietal region of the head, and the mean age of onset is around 13 years [1]. Here we present a late onset en coup de sabre in a 26 year old female who developed it at the site of trauma after six years.
CASE REPORT
A 26 year female, unmarried, presented to us in the outpatient department (OPD) with a chief complaint of dermatosis affecting her frontal and forehead regions of the head for the last three months. The disease began as a discrete area of erythema and progressed steadily forming indurated plaques. The surface became smooth and shiny. There is history of trauma at the same site six years before and she related this dermatosis to the trauma. There is no history of weakness of face. There is no history of seizures, headache or weakness of any body parts. The patient denied any systemic complaints. She didn’t give any history of sequential colour changes of digits on exposure to the cold. Physical examination revealed a well defined, brownish hyper pigmented, indurated plaque present on the frontal and forehead regions of the head reaching to the glabellar region close to the midline in a vertical fashion (Fig. 1). The plaque showed areas of atrophy at some places. Neurological examination didn’t reveal any abnormality. ANA was negative. MRI brain didn’t show any abnormal findings. Skin biopsy on histopathological examination showed atrophy of the epidermis, a dermal and subcutaneous perivascular infiltrate of lymphocytes and plasma cells and thickened and closely packed dense bundles of collagen with sparse adnexal structures. The diagnosis of en coup de sabre was made based on the patient’s history, a suggestive clinical examination and further supported by histopathological findings. She was prescribed topical tacrolimus 0.1% ointment to be applied twice daily on the affected area. After two months of treatment, the induration and the pigmentation of the lesion improved.
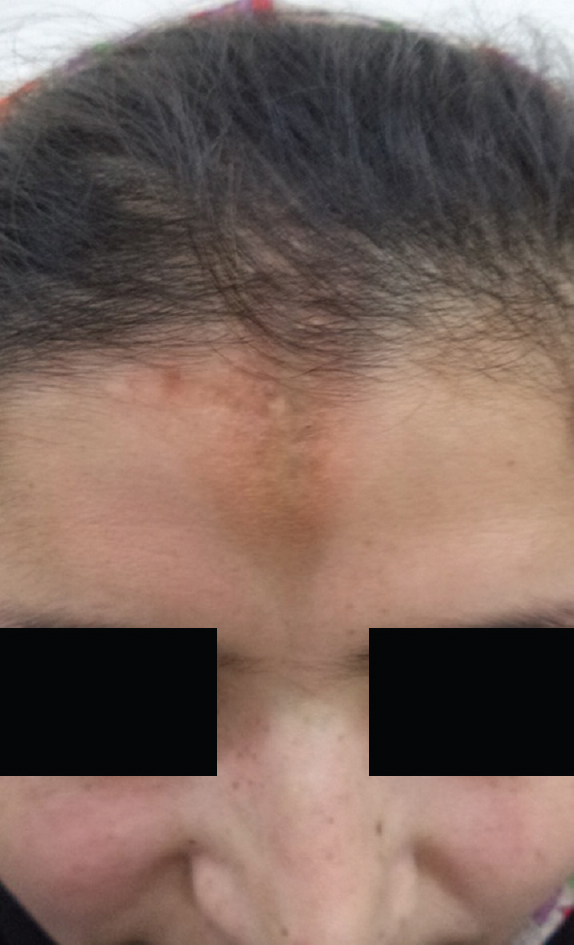
Figure 1: En coup de sabre following trauma in a 26 year old female. Brownish hyperpigmented indurated plaque with areas of atrophy
The written consent for the examination and biospy was obtained from the patient after having been informed about the procedure.
DISCUSSION
Scleroderma connotes a spectrum of disorders characterized by thickening and/or hardening of the skin and fibrosis of the tissues involved. It has been divided into localized and systemic forms. The localized form, also known as morphea, is characterized by predominant skin involvement, with occasional involvement of subjacent muscles. However, it usually spares the internal organs [5]. Linear scleroderma, a type of localized scleroderma, is unique in the sense that it primarily affects the children. Sixty seven percent (67%) of the patients of linear scleroderma are diagnosed before 18 years of age. Linear scleroderma frequently occurs on the limbs but sometimes may involve frontoparietal area of the forehead and scalp; where it is referred to as linear scleroderma en coup de sabre, as the skin lesions resemble to the stroke of a sabre (sword) [6]. The pathogenesis of skin lesions in LS, en coup de sabre and systemic sclerosis seems to be similar, though the exact mechanism is not fully clear [3]. The primary target in LS seems to be vasculature which is supported by clinical and pathological findings [6]. Early skin biopsies have revealed endothelial cell damage preceding the development of fibrosis by months to years. Later, Increase in the vascular permeability is associated with mononuclear cell infiltrate which further leads to perivascular inflammatory cell infiltrates, thickening of intima of vessels, and consequent narrowing of vascular lumina [7]. The inciting event for causing damage to the microvasculature remains elusive. However, antecedent trauma as initial event has been observed in pediatric population [8]. But in older age group, trauma as a precipitating factor has been rarely reported which makes our case a rare presentation.
En coup de sabre has been associated with a number of neurological abnormalities and is usually preceded by the development of skin lesions months to years. Central nervous system (CNS) involvement is usually not correlated with the cutaneous disease activity and may present years after skin lesions. Neurological manifestations in en coup de sabre are varied which include headache, epilepsy, movement disorders, focal neurological deficits and intellectual deterioration [9]. However, in our case there was no neurological involvement seen clinically. In addition, MRI Brain didn’t show any CNS involvement as well. However, a meticulous follow up of the patient is being taken to diagnose any incipient neurological involvement at the earliest.
The treatment of morphea has been updated. The various therapeutic options described in the literature include phototherapy, Imiquimod, topical tacrolimus, calcipotriol in combination with betamethasone dipropionate, methotrexate in combination with systemic steroids, D-penicillamine, cyclosporine, mycophenolate mofetil, photophoresis, etc [10]. In our case, the patient was prescribed topical tacrolimus 0.1% ointment twice daily. After a follow up of two months, the plaque showed reduction in skin thickening, induration and hyperpigmentation.
CONCLUSION
The authors conclude that ‘en coup de sabre’ can present with a late onset in adults and can follow trauma after many years. Hence, a periodic follow up is recommended in such cases to diagnose any CNS involvement at the earliest.
CONSENT
The examination of the patient was conducted according to the Declaration of Helsinki principles. Written informed consent was obtained from the patient for publication of this article and any accompanying images.
REFERENCES
1. Fett N, Werth WP, Update on morphea: part I. Epidemiology,clinical presentation, and pathogenesisJ Am Acad Dermatol 2011; 64: 217-28.
2. Weibel L, Sampaio MC, Visentin MT, Howell KJ, Woo P, Harper JI, Evaluation of methotrexate and corticosteroids for the treatment of localized scleroderma (morphoea) in childrenBr J Dermatol 2006; 155: 1013-20.
3. Goodfield MJD, Jones SK, Veale DJ, Burns T, Breathnach S, Cox N, Griffiths C, The Connective Tissue DiseasesRook’s Textbook of Dermatology 2010; 3: 8th ed. U.K: Wiley-Blackwell; 51.64-51.78.
4. Ehara M, Oono T, Yamasaki O, Matsuura H, Iwatsuki K, Generalized morphea-like lesions arising in mechanically-compressed areas by underclothesEur J Dermatol 2006; 16: 307-9.
5. Zancanaro PC, Isaac AR, Garcia LT, Costa IM, Localized scleroderma in children: Clinical, diagnostic and therapeutic aspectsAn Bras Dermatol 2009; 84: 161-72.
6. Holland KE, Steffes B, Nocton JJ, Schwabe MJ, Jacobson RD, Drolet BA, Linear scleroderma en coup de sabre with associated neurologic abnormalitiesPediatrics 2006; 117: e132-6.
7. Katsumoto TR, Whitfield ML, Connolly MK, The pathogenesis of systemic sclerosisAnnu Rev Pathol 2011; 6: 509-37.
8. Vancheeswaran R, Black CM, David J, Hasson N, Harper J, Atherton D, Childhood-onset scleroderma: Is it different from adult-onset diseaseArthritis Rheum 1996; 39: 1041-9.
9. Amaral TN, Marques Neto JF, Lapa AT, Peres FA, Guirau CR, Appenzeller S, Neurologic involvement in scleroderma en coup de sabreAutoimmune Dis 2012 2012; 719685
10. Fett N, Werth VP, Update on morphea: Part II. Outcome measures and treatmentJ Am Acad Dermatol 2011; 64: 231-42.
Notes
Source of Support: Nil
Conflict of Interest: None declared.
Comments are closed.