Our Dermatol Online. 2011; 5(1): 37-39
DOI:. 10.7241/ourd.20141.07
Date of submission: 06.10.2013 / acceptance: 21.11.2013
Conflicts of interest: None
CUTANEOUS LEISHMANIASIS: DIAGNOSTIC PITFALL CASE REPORT
Asmae EL Hatimi1, Salim Guellouj1, Sanae Chehbouni2, Kawtar Inani1, Hanane Baybay1, Fatima Zahra Mernissi1
1Department of Dermatology and Venereology, Hassan II Hospital University Center, Fez, Morocco
2Departement of Histopathology, Hassan II Hospital University Center, Fez, Morocco
Corresponding author: Dr Asmae EL Hatimi e-mail: asmaelhatimi@yahoo.fr
How to cite an article: EL Hatimi A, Guellouj S, Chehbouni S, Inani K, Baybay H, Mernissi FZ. Cutaneous leishmaniasis: diagnostic pitfall. Case report. Our Dermatol Online. 2014; 5(1): 37-39.
Abstract
Introduction: Cutaneous Leishmaniasis is a parasitic infection encountered in our daily dermatologic practice.
Case report: We present a case of 57 year-old man of Moroccan origin, with erythematous squamous and indurated plaque on the abdomen, treated as sarcoidosis with corticosteroids with no improvement.
Discussion: Cutaneous Leishmaniasis is endemic in 88 countries. Aside from its classical presentation it can manifest in multiple different ways. In our case, the diagnostic of Erysipeloide Leishmaniasis was corrected on the basis of the skin smear and the histopathological examination. Our observation is particular in its clinical presentation and location. To our knowledge it is the first Moroccan case.
Conclusion: Even in endemic countries it is worth reporting unusual forms and locations of Cutaneous Leishmaniasis in order to avoid inappropriate diagnosis and management.
Key words: Leishmaniasis; Leishmaniasis Cutanea; Leishmaniasis types
Introduction
Cutaneous Leishmaniasis is a widely dispersed parasitic vector-borne disease, caused by the Leishmania’s species. Its most common clinical presentation is the “classical“ ulcer which starts as a nodule over exposed area of the body after a sand-fly bite, becomes an ulcer with an indurated raised margins and sharply incised central crater and then usually heals over a period of months. In recent times the number of reports of new and rare variants of Cutaneous Leishmaniasis has been increasing which eludes the diagnosis even in endemic area. We report here a rare and unusual form and localization of Cutaneous Leishmaniasis which was misdiagnosed and treated as Sarcoidosis by dermatologists in an endemic country. To our knowledge, this is the first reported case in Morocco.
Case Report
The case is of a 53 year-old man. In the months preceding the symptoms, he had no past medical history, nor antecedent of trauma or travel. He was referred to our tertiary center for a large, painless erythematous plaque in his abdomen. It had evolved from an initial small plaque noticed 08 months before, which gradually spread. The patient consulted a private dermatologist who performed a skin biopsy revealing granuloma in the histopathologic examination and the patient was treated as sarcoidosis by topical and oral corticosteroids with no improvement. On examination we found an apyretic patient with large erythematous indurated slightly squamous plaque of 20cm at his left hypochondrium (Fig. 1). The diascopy of the lesion did not reveal the lupoidic pattern, and the erythematous color was mitigated. The dermoscopy showed diffuse glomerular vessels (Fig. 2). Our differential diagnosis were mycosis fungoide, sarcoidosis, leishmaniasis, erysipelas and morphea. The patient’s skin smear was positive for Leishmania. The histopathologic examination of the lesion showed an epithelioid geant -cell granuloma with Leishmania’s bodies in the cytoplasm of histiocytes (Fig. 3). The diagnosis of Erysipeloide Leishmania was retained and the patient was treated by oral Clarithromycine 500mg twice a day for 10 days each month during 3 months with topical Aureomycine; The evolution was good (Fig. 4).
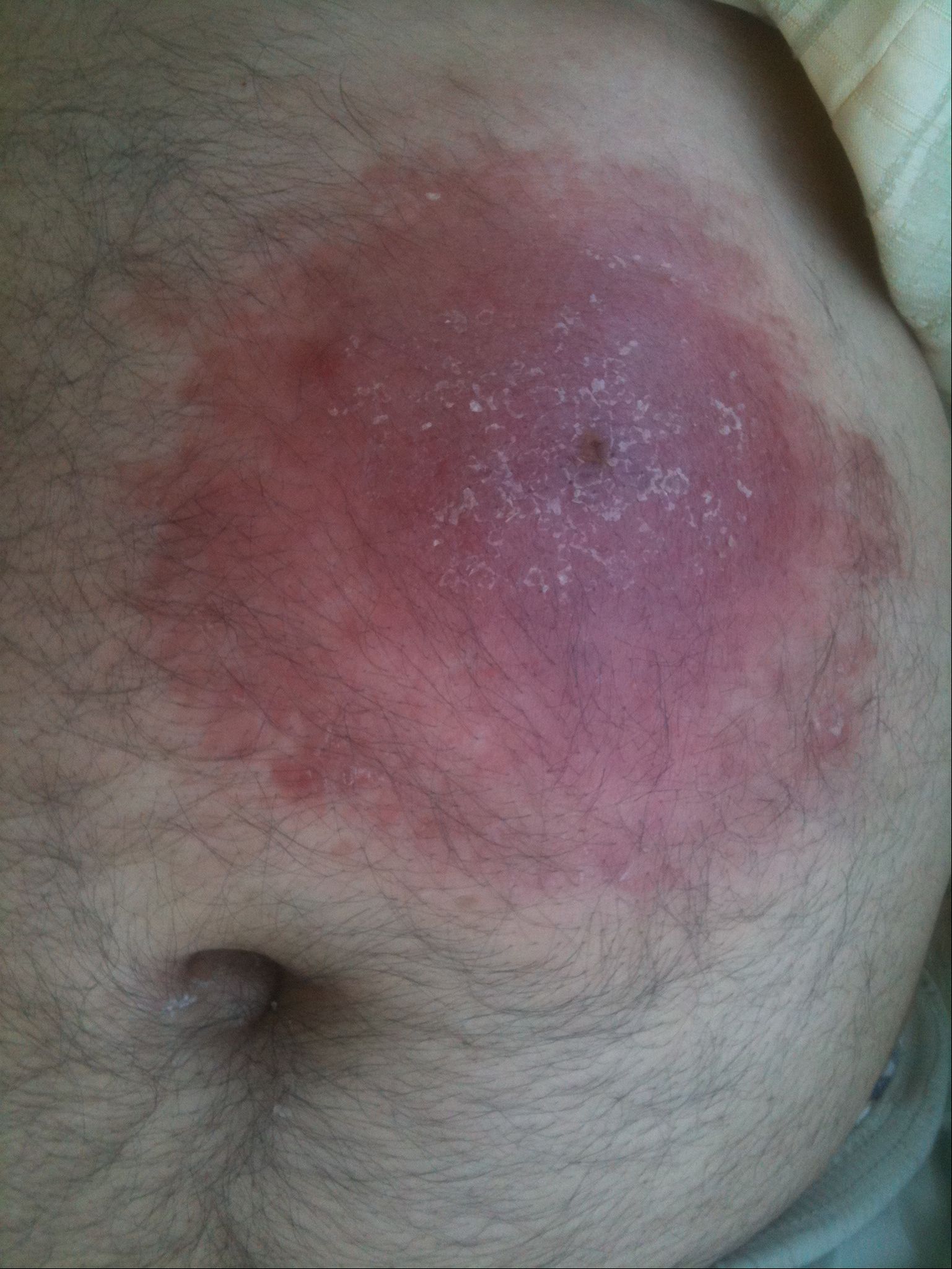 Figure 1. A large erythematous slightly squmous and indurated plaque at the left hypochondrium.
|
.jpg) Figure 2. Glomerular vessels.
|
.jpg) Figure 3. HES x 40 leishmania’s bodies in the cytoplasm of
histiocytes infiltrating the dermis. |
.jpg) Figure 4. Evolution under treatment at 3 months.
|
Discussion
Cutaneous Leishmaniasis (CL) is a parasitic vector-borne disease that is well known in the world. WHO stated that Leishmaniasis is endemic in 88 countries with 1.5 to 2 million new cases each year (WHO 1984, 1990). In Morocco, Leishmaniasis represents a serious health problem. It recognises three epidemiological entities: CL to Leishmania Tropica in the western chain of the Atlas Mountains,represented by a sporadic form with some endemic flare up, CL to Leishmania major in the south and southeast of the Atlas with endemo-epidemic evolution and finally the visceral Leishmaniasis to Leishmania infantum in the Rif and pre-rif area as sporadic form Curaneous Leishmaniasis has a spectrum of clinical presentations ranging from a single lesion to disseminated form. In the course of its typical presentation, CL starts as a small erythematous papule, which gradually enlarges to 1-2 cm in diameter in about 6 months and then ulcerates. These ulcers are painless with a necrotic base and indurated margins and are frequently covered by a firmly adherent crust. Approximately 85% of skin’s lesions are located on the exposed body sites. Recently there has been an increase in the number of reports for new and rare variants of CL [1,2]. Our case supports this finding. Our patient originated from a region that is known to experience a high prevalence of Leishmaniasis. On the eco-epidemiological level this region corresponds with a sporadic cluster of visceral Leishmaniasis to Leishmania infantum and not with Cutaneous Leishmaniasis. Clinically he presented with a slightly squamous, erythematous, indurated plaque of 20cm in diameter at his left hypochondrium. In the literature, this form corresponds with the erysipeloide form of leishmaniasis which is a very rare and unusual presentation of CL. Its frequency was estimated to less than 5% in the literature [3], and all reported cases were from Iran, Pakistan, Turkey, Italy, Tunisia and Equador [4,5]. To our knowledge, our case is the first case reported from Morocco. In all previous reports erysipeloide cutaneous leishmaniasis (ECL) is described as an erythematous and indurated diffuse plaque of the face covering the nose and cheeks with an evolution’s duration of less than 1 year and a good evolution under therapy. It affects predominatly elderly women [6]. Contrasting with all these reported cases, our patient is the first case who manifests the ECL outside the face; on the hypochondrium, but this might be explained by having had increased skin exposure during the summer months. The reasons for this clinical form are poorly understood, but clinical and experimental evidence indicates that vector, parasite and host factors all influence the evolution and outcomes of the broad clinical spectrum of CL. It has been suggested that as with leprosy ,the various atypical lesions of CL are determined by different types of immune response .The granuloma observed in ECL may be explained by the spread of the parasit in the superficial layer of the papillary dermis and the failure of the immune systeme to control parasit replication [7]. Other factors such as skin fragility due to senility, hormonal changes at menopause and trauma were evoked as facilitating factors of ECL given the predilection location to the face, the predominant affection of elderly females and the antecedent of trauma in some reports [4,6]. Our patient was of a male gender, of 53 years old and there were no skin barrier changes. Previously the specie or the strain of leishmania was understood to be the determining factor for the clinical presentation of leishmaniasis. However,currently it is postulated that the interaction between the host immune response and the strain of the parasite influence the clinical presentation of CL and not only the leishmania’s strain [5] In terms of ECL this conjecture is supported by the fact that in all previous reports different species of leishmania were incriminated: L. infantum [7], L. panamensis [5]. In our context, the identification of the leishmania’s species is not a routine test. The diagnosis of CL is easy in the usual clinical presentations. However, in unusual forms it may give rise to difficulties in diagnosis and appropriate treatments even by dermatologists in endemic areas like our patient who was diagnosed and treated incorrectly by a dermatologist as sarcoidosis with topical and oral corticosteroids. This is why the diagnosis of CL should be confirmed by a direct parasitology test and/or histopathologic examination of skin biopsy or in certain cases by PCR. There are various treatment options for CL such as pentavalent antimony compounds, cryotherapy, topical paromomycin, local heat, surgical excision, electrodissection, CO2 laser, Clarithromycine and antifungal [8-10]. In our observation, given the extension of the lesion and the age of the patient, we opted for the oral Clarithromycin with topical Aureomycin.
Conclusion
Given the importance and the complexity of the clinical features of CL, it is worth reporting rare and unusual clinical forms and localizations of this disease in order to familiarize and sensitize physicians, in particular dermatologists, with different clinical presentations to avoid inappropriate diagnosis and management.
REFERENCES
1. Desjeux P. Leishmaniasis. Public health aspects and control. Clin Dermatol. 1996;14:417–23.
2. Iftikhar N, Bari I, Ejaz A. Rare variants of cutaneous leishmaniasis:whitlow, paronychia, and sporotrichoid. Int J Dermatol. 2003;42: 807–9.
3. Raja KM, Khan AA, Hameed A, Rahman SB. Unusual clinical variants of cutaneous leishmaniasis in Pakistan. Br J Dermatol. 1998;139:111-3.
4. Özdem?r M, Çimen K, Mevlitoglu I. Post-traumatic erysipeloid cutaneous leishmaniasis. Int J Dermatol. 2007;46:1292-3.
5. Calvopina M, Gomez EA, Uezato H, Kato H, Nonaka S, Hashiguchi Y. Atypical clinical variants in New World cutaneous leishmaniasis: disseminated, erysipeloid, and recidiva cutis due to Leishmania (V.) panamensis. Am J Trop Med Hyg. 2005;73:281-4.
6. Masmoudi A, Ayadi N, Boudaya S, Meziou TJ, Mseddi M, Marrekchi S, et al. [Clinical polymorphism of cutaneous leishmaniasis in centre and south of Tunisia]. Bull Soc Pathol Exot. 2007;100:36-40.
7. Bongiorno MR, Pistone G, Aricò M. Unusual clinical variants of cutaneous leishmaniasis in Sicily. Int J Dermatol. 2009;48:286-9.
8. Mnejja M, Hammami B, Chakroun A, Achour I, Charfeddine I, Chakroun A, et al. Unusual form of cutaneous leishmaniasis: erysipeloid form. Eur Ann Otorhinolaryngol Head Neck Dis. 2011;128:95-7.
9. Monge-Maillo B, López-Vélez R. Therapeutic Options for Old World Cutaneous Leishmaniasis and New World Cutaneous and MucocutaneousLeishmaniasis. Drugs. 2013;73:1889-920.
10. Sazgarnia A, Zabolinejad N, Layegh P, Rajabi O, Berenji F, Javidi Z, et al. Antileishmanial Activity of Liposomal Clarithromycin against Leishmania Major Promastigotes. Iran J Basic Med Sci. 2012;15:1210-4.
Comments are closed.