Our Dermatol Online. 2013; 4(3): 311-315
DOI: 10.7241/ourd.20133.75
Date of submission: 09.02.2012 / acceptance: 29.02.2013
Conflicts of interest: None
A CLINICAL AND HISTOPATHOLOGICAL STUDY OF CICATRICIAL ALOPECIA
Neerja Puri, Asha Puri
Department of Dermatology and Venereology, Punjab Health Systems Corporation, Ferozepur, Punjab, India
Corresponding author: Dr. Neerja Puri e-mail: neerjaashu@rediffmail.com
How to cite an article: Puri N, Puri A. A clinical and histopathological study of cicatricial alopecia. Our Dermatol Online. 2013; 4(3): 311-315.
Abstract
Introduction: Cicatrical alopecia occurs in otherwise healthy men and women of all ages and is seen worldwide
Material and Methods: A study of 40 patients was conducted to study the clinical variants and histopathology of cicatricial alopecia.
Results and Discussion: n our study, it was seen that maximum number of cases of cicatrical alopecia were of LPP (27.5%) followed by 25% of DLE, 20% patients had pseudopelade of Brocq, SLE was seen in 5% cases followed by Scleroderma, dermatomyositis, Keratosis follicularis spinulosa decalvans, aplasia cutis, kerion, follicular mucinosis, pemphigus, dissecting cellulitis of scalp/ pyogenic folliculitis and acne keloidalis nuchae in 2.5% cases each. Regarding the morphology of lesions,epidermal atrophy was seen in 90% patients, erythema was seen in 55% cases, follicular pluging was seen in 40% patients, telangiectasias in 27.5% patients, diffuse scaling in 25% patients and mottled hyperpigmentation was seen in 20% patients. In our study, commonest histopathological feature of alopecia was perifollicular fibrosis seen in 65% patients, basal cell vacuolization was seen in 52.5% patients,perifollicular lymphocytic infiltrate were seen in 50% patients, epidermal atrophy seen in 35% patients and hyperkeratosis was seen in 20% patients.
Key words: cicatrical; alopecia; histopathological; lichen palmopilaris; folliculitis; lupus erythematosis
Introduction
Cicatricial (scarring) alopecia refers to a group of rare disorders which destroy the hair follicle and replace it with scar tissue, thereby causing permanent hair loss [1]. Causes of cicatricial alopecia are considered either primary or secondary. In primary cicatricial alopecia, the hair follicle is the target of inflammatory destruction, with little effect of the disease process on other components of the dermis [2]. Examples of Primary alopecia include lichen planopilaris, pseudopelade of Brocq, central centrifugal cicatricial alopecia, discoid lupus erythematosus, folliculitis decalvans, and acne keloidalis [3,4]. In secondary cicatricial alopecia, the hair follicle is an „innocent bystander” and is destroyed indirectly. Examples of secondary alopecia include burns and blistering disorders such as pemphigus vulgaris. In primary cicatricial alopecia, there is an inflammatory assault directed primarily at the follicular unit. Although the antigentic trigger for this inflammation is unclear, there is eventually loss of the sebaceous glands and follicular stem cells leading to permanent hair loss. The term „cicatricial alopecia” or scarring alopecia implies the potential of permanent destruction of hair follicle most likely as a result of irreversible damage to epithelial hair follicle stem cells in the region of bulge . In some cases, hair loss is gradual, without symptoms, and is unnoticed for long periods. In other cases, hair loss is associated with severe itching, burning and pain and is rapidly progressive. The inflammation that destroys the follicle is below the skin surface and there is usually no „scar” seen on the scalp. Affected areas of the scalp may show little signs of inflammation, or have redness, scaling, increased or decreased pigmentation, pustules, or draining sinuses [5].
Aims
1. To study the clinical variants of cicatrical alopecia.
2. To study the histopathology of various types of cicatrical alopecia.
Material and Methods
We selected 40 patients of cicatrical alopecia for the study. Written informed consent of all the patients was taken for the study. Prior approval of hospital ethical committee was taken for the study. All the patients were subjected to detailed clinical examination. Routine investigations of all the patients were performed including complete blood count, fasting blood sugar, Liver function tests, Renal function tests and X ray chest. Specialized investigations done included antinuclear antibodies, VDRL and scalp biopsy. For performing scalp biopsy (both vertical & horizontal sections), 4mm punch biopsy of all the patients was performed and was sent for histopathological examination.
Results
The data was tabulated and the results were analysed. Table I shows that maximum number of patients with cicatrical alopecia were between 41-50 years (37.5%), followed by 35% patients between 31-40 years, 20% patients between 21-30 years and 2.5% were between 10 years, between 11-20 years and 51-60 years each. Table II shows that there were 60% females and 40% males and female: male ratio was 1.5:1. Table III shows that 30% patients had single patch and 70% patients had multiple patches of alopecia. Table IV shows that maximum number of cases of cicatrical alopecia were of LPP (27.5%) followed by 25% of DLE, 20% patients had Pseudopelade of Brocq, SLE was seen in 5% cases followed by Scleroderma, dermatomyositis, Keratosis follicularis spinulosa decalvous, aplasia cutis, kerion, follicular mucinosis, pemphigus, dissecting cellulitis of scalp/ pyogenic folliculitis and acne keloidalis nuchae in 2.5% cases each. Table V shows that epidermal atrophy was seen in 90% patients, erythema was seen in 55% cases, follicular pluging was seen in 40% patients, telangiectasias in 27.5% patients, diffuse scaling in 25% patients and mottled hyperpigmentation was seen in 20% patients. Table VI shows that the commonest histopathological feature of alopecia was perifollicular fibrosis seen in 65% patients, basal cell vacuolization was seen in 52.5% patients,perifollicular lymphocytic infiltrate were seen in 50% patients, epidermal atrophy seen in 35% patients and hyperkeratosis was seen in 20% patients.
|
Sr no
|
Age group (years)
|
Number of patients
|
Percentage |
|
1
|
Below 10 years
|
1
|
2.5 |
|
2
|
11-20 years
|
1
|
2.5 |
|
3
|
21-30 years
|
8
|
20 |
|
4
|
31-40 years | 14 | 35 |
| 5 |
41-50 years |
15 |
37.5 |
| 6 |
51-60 years |
1 |
2.5 |
| Total |
40 |
100 |
Table I. Age distribution of patients
|
Sr no
|
Sex
|
Number of patients
|
Percentage |
|
1
|
Females
|
24
|
60 |
|
2
|
Male
|
16
|
40 |
|
|
Total
|
40
|
100 |
Table II. Sex distribution of patients
|
Sr no
|
Number of patches
|
Number of patients
|
Percentage |
|
1
|
Single patch
|
12
|
30 |
|
2
|
Multiple patches
|
28
|
70 |
|
|
Total
|
40
|
100 |
Table III. Number of alopecic patches
|
Sr no
|
Aetiological cause
|
Number of cases
|
Percentage |
|
1
|
DLE
|
10
|
25 |
|
2
|
LPP
|
11
|
27.5 |
|
3
|
SLE
|
2
|
5 |
|
4
|
Scleroderma | 1 | 2.5 |
| 5 | Dermatomyositis | 1 | 2.5 |
| 6 | Keratosis follicularis spinulosa decalvans | 1 | 2.5 |
| 7 | Aplasia cutis | 1 | 2.5 |
| 8 | Kerion | 1 | 2.5 |
| 9 | Follicular mucinosis | 1 | 2.5 |
| 10 | Pemphigus | 1 | 2.5 |
| 11 | Dissecting cellulitis of scalp/ pyogenic folliculitis | 1 | 2.5 |
| 12 | Acne keloidatis nuchae | 1 | 2.5 |
| 13 | Pseudopelade of Brocq | 8 | 20 |
| Total | 40 | 100 |
Table IV. Aetiology of cicatrical alopecia
|
Sr no
|
Morphology of alopecia
|
Number of cases
|
Percentage
|
|
1
|
Erythema
|
22
|
55 |
|
2
|
Diffuse scaling
|
10
|
25 |
|
3
|
Follicular plugging
|
16
|
40 |
| 4 |
Telangiectasia |
9 |
27.5 |
|
5
|
Mottled hyperpigmentation | 8 | 20 |
| 6 |
Atrophy |
36 |
90 |
Table V. Morphology of alopecia
|
Sr no
|
Histopathological features
|
Number of cases
|
Percentage |
|
1
|
Hyperkeratosis
|
8
|
20 |
|
2
|
Follicular plugging
|
22
|
5,5 |
|
3
|
Basal cell vacuolization
|
21
|
52.5 |
|
4
|
Perifollicular lymphocytic infiltrate | 20 | 50 |
| 5 |
Perifollicular fibrosis |
26 |
65 |
| 6 |
Epidermal atrophy |
14 |
35 |
Table VI. Histopathological features of alopecia
Discussion
In our study, maximum number of patients with cicatrical alopecia were between 41-50 years (37.5%), followed by 35% patients between 31-40 years, 20% patients between 21-30 years and 2.5% were between 10 years, between 11-20 years and 51-60 years each. There were 60% females and 40% males and female: male ratio was 1.5:1. Out of all the patients, 30% patients had single patch and 70% patients had multiple patches of alopecia. It was seen that maximum number of cases of cicatrical alopecia were of LPP (Fig. 1a) (27.5%) followed by 25% of DLE (Fig. 2), 20% patients had pseudopelade of Brocq, SLE was seen in 5% cases followed by Scleroderma, dermatomyositis, Keratosis follicularis spinulosa decalvans (Fig. 3), aplasia cutis (Fig. 4), kerion (Fig. 5), follicular mucinosis (Fig. 6), pemphigus, dissecting cellulitis of scalp/ pyogenic folliculitis (Fig. 7) and acne keloidalis nuchae in 2.5% cases each. Regarding the morphology of lesions, epidermal atrophy was seen in 90% patients, erythema was seen in 55% cases, follicular pluging was seen in 40 % patients, telangiectasias in 27.5% patients, diffuse scaling in 25% patients and mottled hyperpigmentation was seen in 20% patients. In our study, commonest histopathological feature of alopecia was perifollicular fibrosis seen in 65% patients,basal cell vacuolization was seen in 52.5% patients,perifollicular lymphocytic infiltrate were seen in 50% patients, epidermal atrophy seen in 35% patients and hyperkeratosis was seen in 20% patients. The combination of diffuse scaling, erythema, telangiectases, and mottled hyperpigmentation within areas of scarring alopecia was a distinctive feature of DLE [6,7]. In most patients with LP, the histologic changes involved only the follicles and the perifollicular dermis. Less frequently, the inflammatory process extended to the epidermis and the papillary dermis. In all cases, histopathologic features allowed LP (Fig. 1b) to be distinguished from DLE (Fig. 2) regardless of the stage of the disease. The finding of a bandlike fibrotic thickening of the papillary dermis accompanied by fibrotic tracts at sites of destroyed follicles appeared to be a hallmark of „burnt out” lesions of LP. Most early lesions of lichen planopilaris showed a focally dense band like perifollicular lymphocytic infiltrate at the level of infundibulum and the isthmus where the hair ‘bulge’is located.
Three types of alopecia have been described in patients with SLE.
1. Discoid lesions with associated scarring alopecia;
2. A diffuse non-scarring alopecia with transient hair loss related to the activity of the disease (a telogen effluvium like picture);
3. Lupus hair which is an unusual non-scarring alopecia characterized by thin weakened hairs at the periphery of the scalp. The hairs fragment and result in a characteristic unruly appearance. In addition alopecia areata has been discovered in patients with SLE rarely scarring DLE and non-scarring AA like lesions may coexist in the same patient.
In a study of 89 patients with scarring alopecia and DLE showed a lymphocytic infiltrate mainly directed to the mid portion of the follicle and a normal anagen: telogen ratio [8]. The authors postulated that the loss of follicle may be due to the destruction of the stem cells which reside in the bulge area where the arrector pili muscle inserts. Pseudopelade of Brocq (PB) is a permanent progressive scarring alopecia characterized by numerous alopecic patches localized only in the scalp, that tend to coalesce into larger, irregular plaques with policyclic borders. PB can be considered either the final atrophic stage of several scarring disorders such as lichen planus pilaris (LPP) and discoid lupus erythematosus (DLE) (secondary PB) or an autonomous disease (primary PB). PB is a type of scarring alopecia of the scalp associated with a peculiar clinical presentation and evolution, which cannot be considered an autonomous nosologic entity because in 66.6% of patients it is the end stage of other inflammatory chronic diseases such as LPP and DLE [9]. The early evolving lesions of the hair follicles are described in pseudopelade, a type of cicatricial alopecia where clues for the diagnosis of lupus erythematosus or lichen plano-pilaris are lacking. A sudden and synchronized cell death of all the cells of the epithelial sheaths of the hair follicles occurs and is associated with a dense infiltration by lymphocytes. The epidermis remains uninvolved. The histopathology of pseudopelade of Brocq is of ‘burn out’ scarring alopecia. The classical description of PPB is one of predominantly follicular scarring chaarcterized by columns of fibrosis replacing hair follicles and sometimes extending into subcutaneous fat. This is accompanied by a loss or decrease of sebaceous glands. Absence of widespread (interfollicular) scarring. Epidermis is normal or rarely atrophic, Sweat glands are normal and marked inflammation is absent. The inflammatory phase is short with lymphocytic inflammation in superficial dermis which is perivascular or perifollicular, centred about the infundibulum or mid point of the follicle. The inflammation remains patchy, mild perivascular and eventually disappears. Follicles are destroyed with marked hair shafts remaining fibrous tracts mark the site of obliterated follicles. The histopathology of folliculitis decalvans is characterized by patchy pustular alopecia with areas of scarring with pustules at periphery. Early pustular lesions show an abscess centered about the affected follicle at the level of the lower to the upper infundibulum, which may show comedonal dilataion. Later lesions typically show perifollicular inflammation composed predominantly of lymphocytes with fewer plasma cells, neutrophils, eosinophils and giant cells. There may be hyperkeratosis and follicular plugging. Late stage lesions show follicular destruction secondary to diffuse dermal scarring. In such lesions, the inflammation is less pronounced and is composed of lymphocytes, macrophages and some giant cells in response to follicular remnants.
.jpg) Figure 1a. Atrophic violaceous plaque of lichen plano pilaris
|
.jpg) Figure 1b. Photomicrograph showing lymphocytic band like infiltrate involving the infundibulum (H&E stain 100X)
|
.jpg) Figure 2. Erythematous scaly plaque of DLE on forehead
|
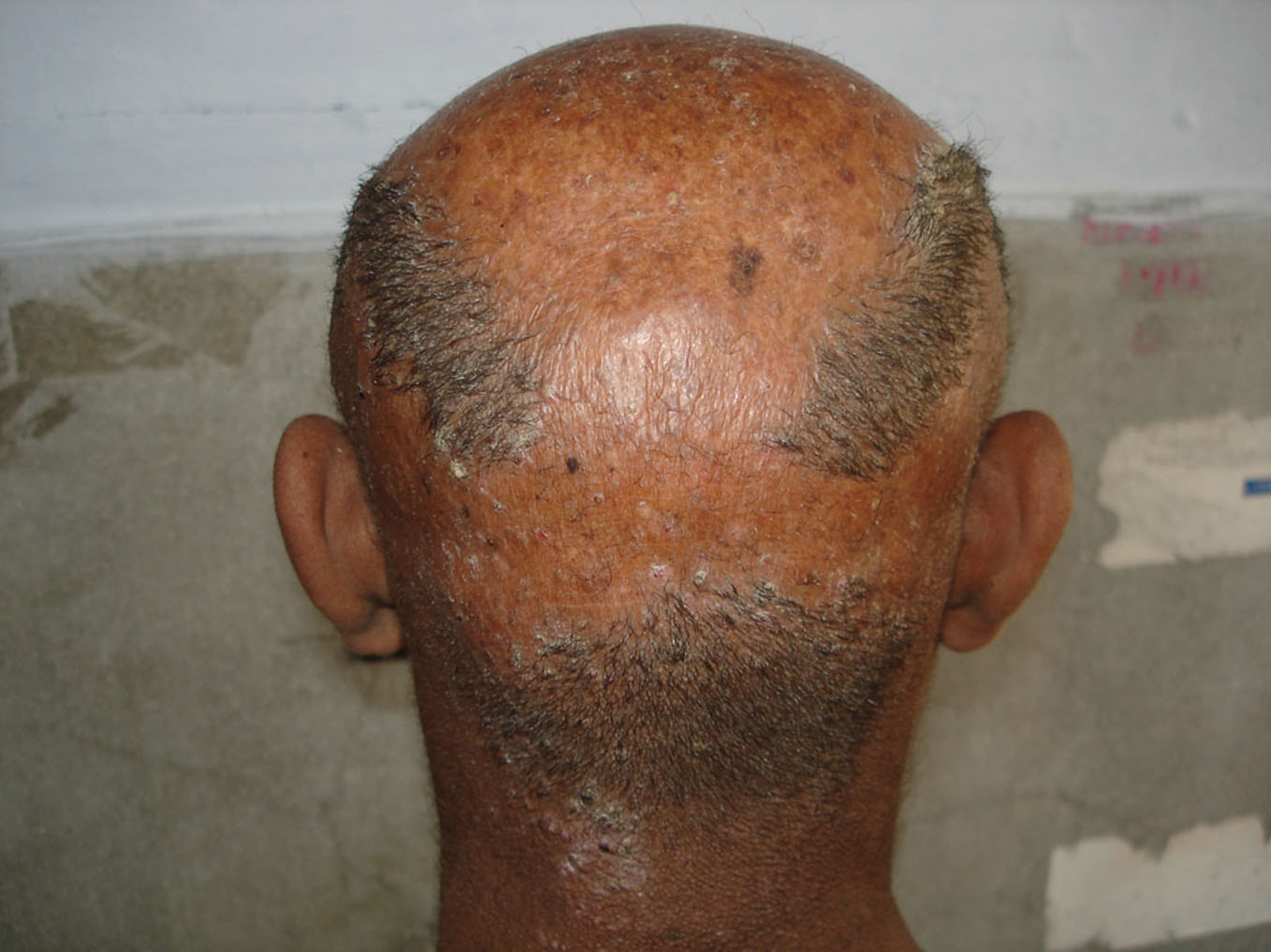 Figure 3. Atrophic scaly plaque of keratosis follicularis atrophicans decalvans
|
 Figure 4. Atrophic patch over the scalp of 8 months old child with aplasia cutis
|
 Figure 5. Kerion in a 4 year old child
|
 Figure 6. Follicular mucinosis in a 70 year old man
|
 Figure 7. Pustular folliculitis in a 50 year old man
|
REFERENCES
1. Ross EK, Tan E, Shapiro J: Update on primary cicatricial alopecias. J Am Acad Dermatol. 2005;53:1.
2. Olsen E, Bergfeld W, Cotsarelis G, Price VH ET AL: Workshop on Cicatricial Alopeica. Summary of North American Hair Research Society (NAHRS). J Am Acad Dermatol. 2003;48:103-10.
3. Whiting D, Olsen E: Central centrifugal cicatricial alopecia. Dermaol Ther. 2008;21:268-78.
4. Templeton SF, Solomon AR: Scarring alopecia: a classification based on microscopic criteria. J Cutan Pathol. 1994;21:97-109.
5. Headington JT, Astle N: Familial focal alopecia. A new disorder of hair growth clinically resembling pseudopelade. Arch Dermatol. 1987;123:234-7.
6. Werth VP, White WL, Sanchez MR, Franks AG: Incidence of alopecia areata in lupus erythematosus. Arch Dermatol. 1992;128:368-71.
7. Wilson CL, Burge SM, Dean D, Dawber RP: Scarring alopecia in discoid lupus erythematosus. Br J Dermatol. 1992;126:307-14.
8. Annessi G, Lombardo G, Gobello T, Puddu P: A clinicopathologic study of scarring alopecia due to lichen planus: comparison with scarring alopecia in discoid lupus erythematosus and pseudopelade. Am J Dermatopathol. 1999;21:324-31.
9. Nayar M, Schomberg K, Dawber RP, Millard PR: A clinicopathological study of scarring alopecia. Br J Dermatol. 1993;128:533-6.
10. Sobhy N, Aly H, El Shafee A, El Deeb M: Evaluation of the effect of injection of dutasteride as mesotherapeutic tool in treatment of androgenetic alopecia in males. Our Dermatol Online. 2013;4:40-5.
11. Abreu Velez AM, Deo Klein A, Howard MS: Immunologic findings in central centrifugal cicatricial alopecia. Our Dermatol Online. 2012;3:202-5.
12. Kasumagić-Halilovic E, Ovcina-Kurtovic N: Serum levels of interleukin-1 (IL-1α, IL-1β) in patients with alopecia areata. Our Dermatol Online. 2012;3:161-3.
13. Abreu Velez AM, Deo Klein A, Howard MS: Skin appendageal immune reactivity in a case of cutaneous lupus. Our Dermatol Online. 2011;2:175-80.
Comments are closed.