N Dermatol Online. 2010; 1(2): 22-25
Conflicts of interest: None
MALLASEZIA FOLLICULITIS ON THE NECK
Brzeziński Piotr1, Kaczmarek Danuta2
16th Military Support Unit, Ustka, Poland
210 Military Clinical Hospital with Polyclinic, ALAB, Bydgoszcz, Poland
Corresponding author: Dr. Piotr Brzeziński e-mail: brzezoo77@yahoo.com
How to cite this article: Brzeziński P, Kaczmarek D. Malassezia Folliculitis na szyi. N Dermatol Online 2010; 1(2): 22-25.
Abstract
Folliculitis caused by Malassezia spp. classified as yeasts in our climate (Poland) is fairly rare disease . MF is most commonly found on the chest, back, upper arms, and less frequently on the face. Permanent symptom is persistent itching. The favorable external conditions, which are largely due to high temperature and humidity, and endogenous factors, such as immunosuppression, there is a lipophilic yeast multiplication in the hair follicles. The aim of this article is presentation of the patient with Malassezia Folliculitis on the neck. Patient age 33 with 1- to 2-mm monomorphic papules and pustules on chest. Skin lesions accompanied by itching. In the treatment used topical: ketoconazole containing shampoo, 1% clindamycin cream, 0,5% hydrocortisonum cream, fluconazole 400 mg once p.o.
Key words: folliculitis; Malassezia furfur
Introduction
Weary et al first described Pityrosporum folliculitis in 1969, and later in 1973 Potter et all identified Pityrosporum folliculitis as a separate clinical and histologic diagnosis [1]. Folliculitis caused by Malassezia spp in our climate (Poland) is fairly rare disease. MF is most commonly found on the chest, back, upper arms, and less frequently on the face [2,3]. Rare symptom is persistent itching. The favorable external conditions, which are largely due to high temperature and humidity, and endogenous factors, such as immunosuppression, there is a lipophilic yeast multiplication in the hair follicles. The occurrence of MF reported in patients after bone marrow transplant, kidney and heart [4], patients with white-meadow [5] and Hodgkin’s disease [6]. and was repeatedly questioned, however many Malassezia is a dimorphic lipophilic yeast that can be found in the stratum corneum and hair to 90% of studies confirm the role of fungus in the etiology of inflammation of hair follicles [7]. individuals without symptoms [8.9]. Often it is misdiagnosed as acne vulgaris [10].
Aim
The aim of this article is presentation of the patient with Malassezia Folliculitis on the neck.
Case Report
Patient age 33, generally healthy with 1- to 2- mm monomorphic papules and pustules on chest (fig. 1,2). Skin lesions accompanied by itching. Skin lesions persisted for 3 days. In the treatment used topical: ketoconazole containg shampoo, 1% clindamycin cream, 0,5% hydrocortisonum cream, fluconazole 400 mg once p.o. (tabl. 1). In addition, the patient reports that periodically affects his erythematous-exfoliative specified below in the folds of the nasal and eyebrow area.
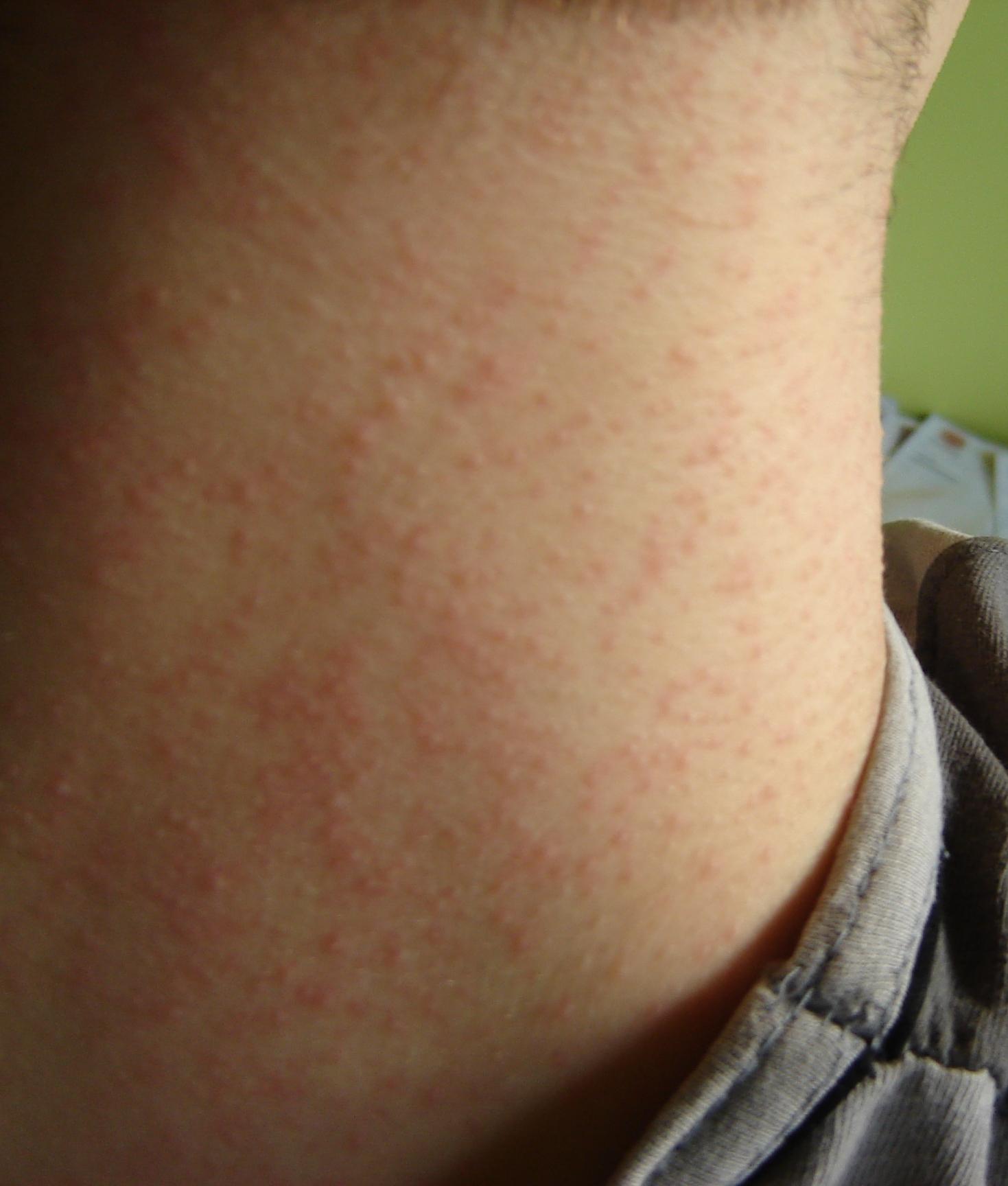 Figure 1. Mallasezia Folliculitis on the neck
|
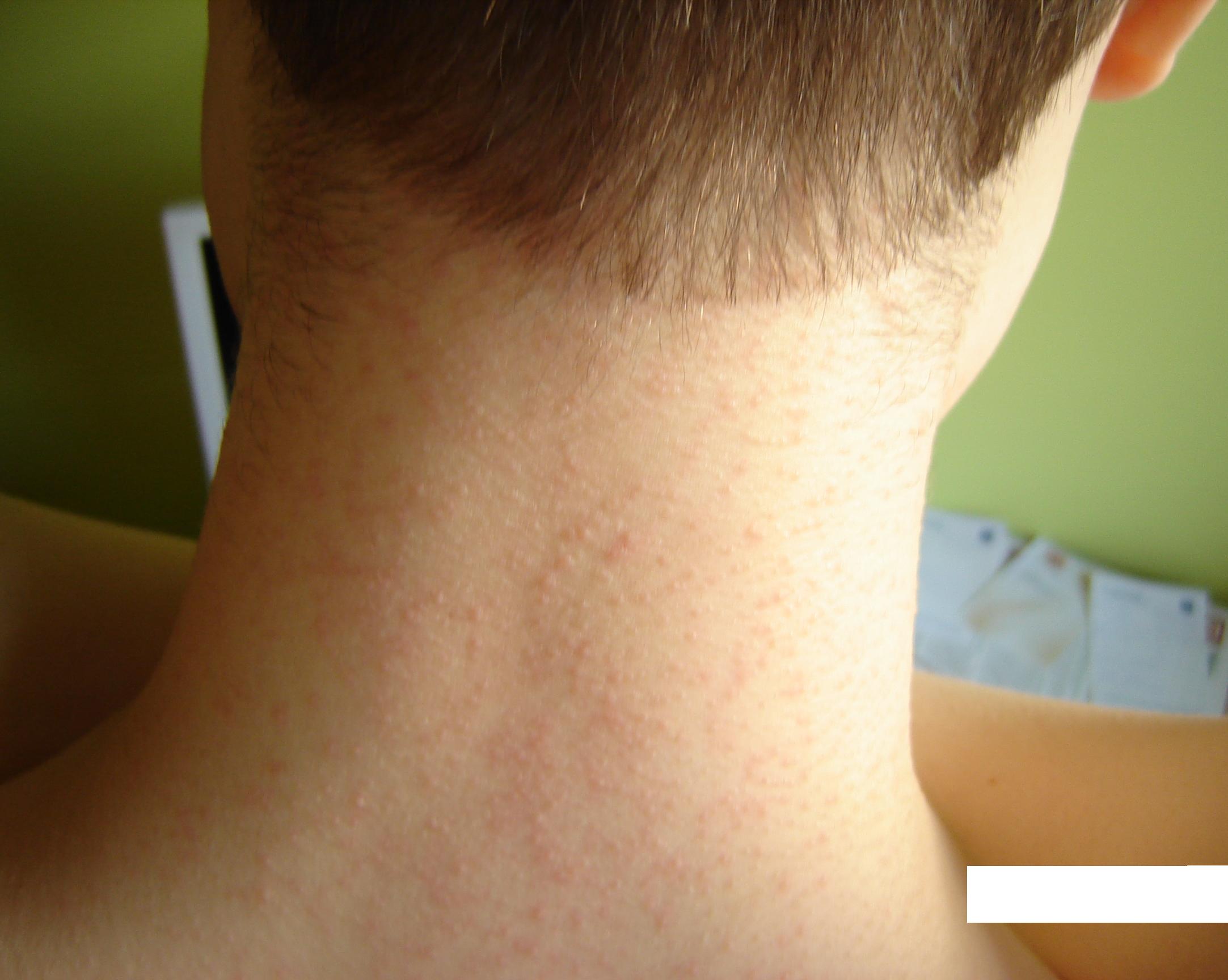 Figure 2. Mallasezia Folliculitis on the neck
|
Discussion
Yeast of the genus Malassezia are a component of normal comensal human skin and can isolate them from areas rich in sebaceous glands. Malassezia furfur (Pityrosporum ovale, Pityrosporum orbiculare) is a lipophilic, saprophytic, unipolar, dimorphic, Grampositive, double-walled, oval-to-round yeast [11]. Probably the function of the disorder pilosebaceous leads to proliferation of the yeast Malassezia and folliculitis. Leeming et al [12] studied healthy skin up in 20 points. The highest average concentration of cells, Malassezia furfur was found on the skin of the chest, upper parts of back, pinna, skin of cheecks and brow. MF can occur after corticosteroid therapy, in diabetes mellitus, after organ transplantation, chemotherapy or stress [13]. MF is commonly found in adolescents presumably because of the increased activity of their sebaceous glands. In them, too often comes to the development of pityriasis versicolor and seborrheic dermatitis [14,15]. Katherine Ayers et al report increased incidence of MF in girls [10]. MF is also more common in hot and humid climate [8,16]. Many patients have coexisting seborrheic dermatitis [17], as in our case. The diagnosis of MF is based on clinical suspicion of the classic presentation of pruritic papulopustules found in a follicular pattern on the back, chest, upper arms, and, occasionally the neck. They are rarely present on the face. An improvement in the lesions with empiric antimycotic therapy supports a clinical diagnosis of MF. Differential diagnosis are presented in table number 2. MF may be underdiagnosed because it can mimic acne vulgaris. Typical patients will not respond to or only partially respond to topical and oral antibiotics, topical retinoids, and other acne treatments. A potassium hydroxide (KOH) preparation may be helpful for microscopic identification of the yeasts associated with MF. In a study with KOH skin lessions under a microscope you can see the spores. This allows for immediate diagnosis than either skin biopsy or culture. Breeding Malassezia is rarely useful. Malassezia grows only within a medium rich in C12, C13, and C14 fatty acids, which can be achieved by adding olive oil to the medium [8,18]. Both topical and oral antifungals are effective agents in the treatment of MF. Oral antifungals have the advantage of immediate clearing of the lesions. Patients have been successfully treated with oral pulse itraconazole, fluconazole, ketoconazole. Other that are used to treat MF are ciclopiroxolamine cream, econazole cream, alcohol and salicylic acid solution, propylene glycol 50% in water, selenium sulfide [19,20,21]. There is no one specific treatment regimen that can be suggested to eradicate MF. Therefore, close patient follow-up to monitor response to therapy is important. In that case received a good response to the topical clotrimazolum cream, hydrocortisone cream and oral fluconazole in single dose.
REFERENCES
1. Potter BS., Burgoon CF Jr., Johnson WC.: Pityrosporum folliculitis. Report of seven cases and review of the Pityrosporum organism relative to cutaneous disease. Arch Dermatol. 1973; 107: 388-391 2. Zawirska A., Adamski Z.: Grzyby z rodzaju Malassezia.Nowe informacje. Post Dermatol Alergol 2004; 2: 97-103 3. Masmoudi A., Ben Salah H., Makni F., Chikrouhou F., Boudaya S., Ayadi A., Turki H.: Folliculite à Malassezia sp : 21 cas. Ann Dermatol Venereol. 2010; 137: 305-306 4. Vicente Alves EJ., Costa Martins JE., de Ribeiro EB., Sotto MN.: Pityrosporum folliculitis: renal transplantation. Case report. J Dermatol. 2000; 27: 49-51 5. Yohn JJ., Lucas J., Camisa C.: Malassezia folliculitis in immunocompromised patients. Cutis. 1985; 35: 536-538 6. Helm KF., Lookingbill DP.: Pityrosporum folliculitis and severe pruritis in two patients with Hodgkin’s disease. Arch Dermatol. 1993; 129: 380-381 7. Faergemann J., Johansson S., Back O.: An immunologic and cultural study of Pityrosporum folliculitis. J Am Acad Dermatol. 1986; 14: 429-433 8. Hort W., Nilles M., Mayser P.: Malassezia-Hefen und ihre Bedeutung in der Dermatologie. Hautarzt 2006; 57: 633-645 9. Kortüm AK., Meller S., Hengge U., Kruse R., Reifenberger J., Bruch-Gerharz D.: Pityrosporumfollikulitis (Malasseziafollokulitis). Hautarzt 2006; 57: 908-909 10. Ayers K., Sweeney SM., Wis K.: Pityrosporum Folliculitis. Diagnosis and Management in 6 Female Adolescents With Acne Vulgaris. Arch Pediatr Adolesc Med. 2005; 159: 64-67. 11. Akaza N., Akamatsu H., Sasaki Y., Kishi M., Mizutani H., Sano A., Hirokawa K., Nakata S., Nishijima S., Matsunaga K.: Malassezia folliculitis is caused by cutaneous resident Malassezia species. Med Mycol. 2009; 47: 618-624. 12.Leeming JP., Notman FH., Holland KT.: The distribution and ecology of Malassezia furfur and cutaneous bacteria on human skin. J Appl Bacteriol 1989; 67: 47-52. 13. Ashbee HR, Evans EGV (2002) Immunology of diseases associated with Malassezia species. Clin Micro Rev 15:21–57 14. Lévy A., Feuilhade de Chauvin M., Dubertret L., Morel P., Flageul B.: Folliculites à Malassezia. Caractéristiques et réponses thérapeutiques chez 26 malades. Ann Dermatol Venereol. 2007; 134: 823-828 15. Tajima M.: Malassezia species in patients with seborrheic dermatitis and atopic dermatitis. Nippon Ishinkin Gakkai Zasshi 2005; 46: 163-167 16. Bulmer GS., Pu XM., Yi LX.: Malassezia folliculitis in China. Mycopathologia 2008; 165: 411-412 17. Gupta AK., Batra R., Bluhm R., Boekhout T., Dawson TL Jr.: Kin diseases associated with Malassezia species. J Am Acad Dermatol. 2004; 51: 785-798 18. Ljubojević S., Skerlev M., Lipozencić J., Basta-Juzbasić A.: The role of Malassezia furfur in dermatology. Clin Dermatol. 2002; 20: 179-182 19. Hill MK., Goodfield JD., Rodgers FG., Crowley JL., Saihan EM.: Skin surface electron microscopy in Pityrosporum folliculitis. The role of follicular occlusion in disease and the response to oral ketoconazole.Arch Dermatol.1990; 126: 181-184 20. Ford GP., Ive FA., Midgley G.: Pityrosporum folliculitis and ketoconazole. Br J Dermatol. 1982; 107: 691-695 21. Aytimur D., Sengöz V.: Malassezia folliculitis on the scalp of a 12-year-old healthy child. J Dermatol. 2004; 31: 936-939.
Comments are closed.